Key Takeaways: Assessing Your Situation
- Immediate Assessment: If you observe confusion, seizures, or difficulty breathing, these are critical signs of detoxing that require immediate emergency care (Call
911). - Success Factor: Medical supervision reduces the risk of fatal complications like delirium tremens by providing stabilization medications that are not available at home.
- Next Action: If symptoms are present but not yet life-threatening, contact Arista Recovery to verify insurance coverage—a process that typically takes less than 30 minutes.
Why Medical Detox Supervision Saves Lives
- Is the person confused about where they are or what day it is?
- Are they experiencing uncontrollable shaking or tremors?
- Is their heart rate noticeably rapid or irregular?
- Are they seeing or hearing things that aren’t there?
If you answered “Yes” to any of these, immediate medical attention is required.
The Neurobiology Behind Withdrawal Risks
Mistake 1: Ignoring the Brain’s Role in Withdrawal Danger
Many people believe withdrawal is just about feeling sick or uncomfortable, like a bad flu. However, the real danger starts deep inside the brain. When you stop using alcohol, opioids, or benzodiazepines after regular use, the brain’s chemical balance shifts rapidly. This sudden change causes the nervous system to become dangerously overactive, leading to signs of detoxing such as seizures, hallucinations, or life-threatening complications like delirium tremens.
“Without medical support, the body can’t always handle these changes safely. For example, delirium tremens has a mortality rate of up to 25% if not treated by professionals.” 1
What to do instead: If you or a loved one is showing physical distress—such as shaking, confusion, heavy sweating, or rapid heart rate—do not try to “tough it out” at home. Follow this safer approach:
- Recognize severe symptoms early: Watch for sudden confusion, seizures, or hallucinations.
- Contact a medical detox provider immediately: Ohio has resources like Arista Recovery, where medical staff are trained to monitor and stabilize brain and body function.
- Avoid cold turkey: Never stop alcohol, benzodiazepines, or opioids suddenly on your own. Gradual, supervised detox is much safer.
Understanding the neurobiology behind withdrawal empowers you to make safer choices. Arista Recovery is here to help you or your family take the first step toward lasting recovery.
Ohio’s Overdose Crisis Context
Mistake 2: Underestimating Ohio’s Overdose Crisis During Detox
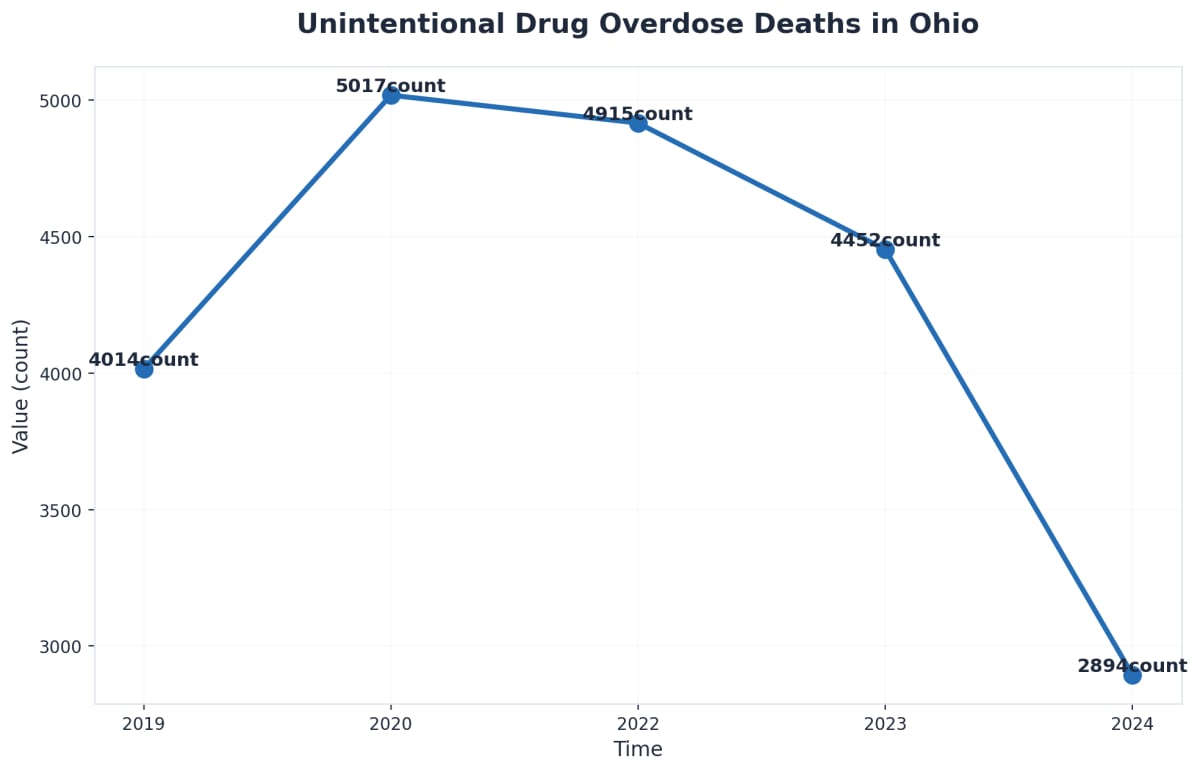
Many families assume that if withdrawal symptoms seem mild at first, home detox is safe. This is a dangerous assumption in the context of Ohio’s current landscape. Ohio has faced some of the highest rates of unintentional drug overdose deaths in the country. In 2022 alone, nearly 5,000 Ohioans lost their lives to overdose, with opioids like fentanyl playing a major role7.
What to do instead: Even if symptoms seem manageable, reach out for medical help. Here is how to stay safe:
- Acknowledge the relapse risk: Withdrawal—especially from opioids—can lead to relapse and fatal overdose after just a few days of sobriety due to lowered tolerance.
- Utilize local resources: Use Ohio resources like Arista Recovery for medical detox supervision. Trained staff can monitor symptoms and respond quickly if complications arise.
- Monitor vitals: Watch for changes in breathing, alertness, or heart rate. These may signal a medical emergency.
Ohio’s overdose crisis is a reminder to never take chances with detox. Reaching out for professional help can truly save lives.
Alcohol Withdrawal: Recognizing Deadly Signs of Detoxing
Early Warning Signs Within 24-48 Hours
Mistake 3: Overlooking Early Warning Signs in the First Two Days
The first 24 to 48 hours after stopping drinking are critical. Families often dismiss sweating, shaking, or insomnia as mere discomfort, failing to realize these are early signs of detoxing that can escalate quickly. In Ohio, where alcohol use is widespread, this misunderstanding puts loved ones at significant risk.
| Symptom Category | Specific Warning Signs | Action Required |
|---|---|---|
| Physical | Sweating, racing heart, nausea, headache | Monitor closely; hydrate |
| Psychological | Anxiety, irritability, agitation | Reduce stimuli; calm environment |
| Critical | Confusion, hallucinations, seizures | Call 911 Immediately |
More than 5% of people who go through alcohol withdrawal without treatment develop seizures1. Don’t wait for symptoms to worsen. If you notice confusion or a major behavioral change, seek emergency care immediately.
Delirium Tremens Emergency Symptoms
Mistake 4: Missing the Emergency Signs of Delirium Tremens (DTs)
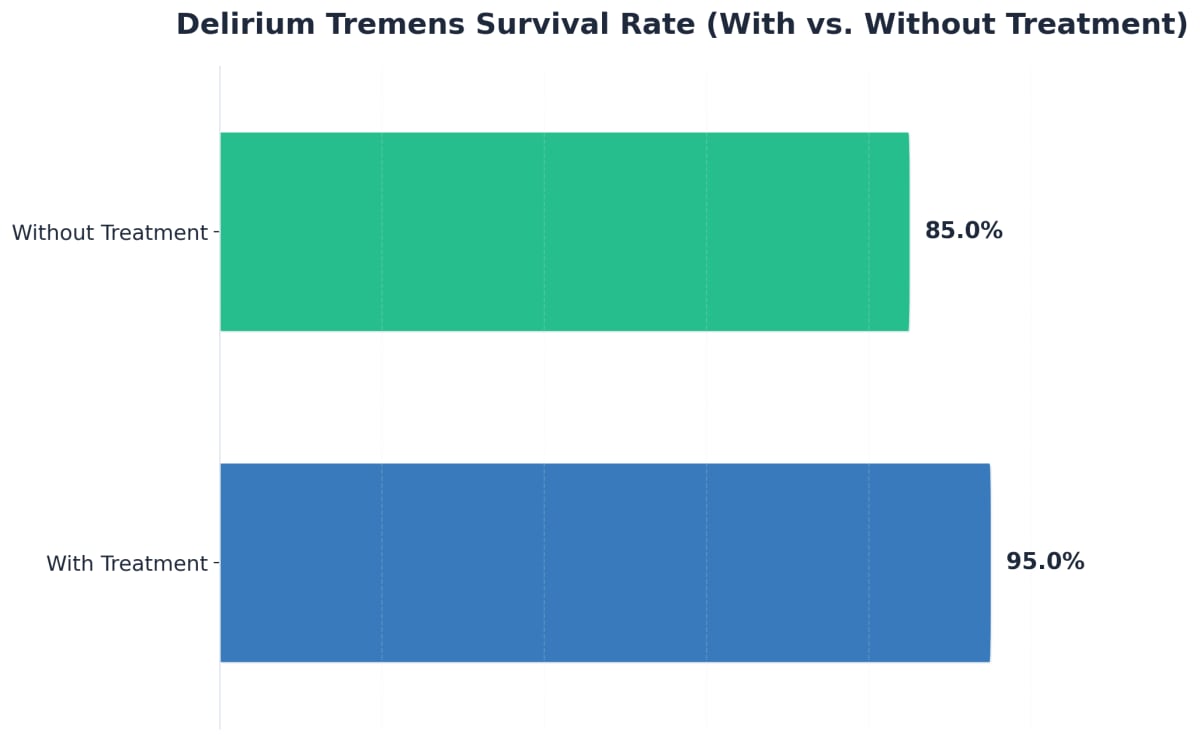
Delirium tremens (DTs) is the most dangerous complication of alcohol withdrawal. It typically develops 2-4 days after the last drink but can appear later. The mortality rate can be as high as 15-25% without treatment1, 2, 3. However, with medical support, most people survive and recover.
What to do instead:
- Know the signs: Sudden confusion, severe agitation, shaking all over, heavy sweating, hallucinations, and high blood pressure.
- Act fast: Never wait it out—delirium tremens is a true emergency.
- Seek expert help: Reach out to Arista Recovery or your nearest Ohio hospital immediately.
Opioid Withdrawal Complications and Signs of Detoxing
Physical Symptoms and Timeline Variations
Mistake 5: Overlooking the Range and Timing of Opioid Withdrawal Symptoms
It is a common misconception that all opioid withdrawals follow the same timeline. With the prevalence of fentanyl and synthetic opioids in Ohio, signs of detoxing can appear in as little as 12 hours and are often more intense than heroin withdrawal4.
Click to see the Symptom Progression Timeline
Early Stage (12-24 hours): Muscle aches, runny nose, yawning, sweating, anxiety.
Peak Stage (24-72 hours): Nausea, vomiting, diarrhea, stomach cramps, rapid heart rate, high blood pressure.
Late Stage (4+ days): Lingering anxiety, insomnia, drug cravings.
What to do instead:
- Monitor hydration: Watch for dehydration caused by vomiting and diarrhea.
- Seek early intervention: Reach out to Arista Recovery or an Ohio-based detox provider early, even if symptoms seem mild at first.
- Track changes: Keep a log of symptoms and timing to help medical staff provide the most accurate care.
Relapse and Overdose Danger Window
Mistake 6: Not Realizing the High Risk of Relapse and Overdose After Detox
The period immediately following withdrawal is when the risk of fatal overdose is highest. As the body detoxes, tolerance drops rapidly. Returning to the same dose used previously can overwhelm the system, especially given the potency of fentanyl in Ohio’s drug supply4.
What to do instead:
- Plan for the danger window: Discuss overdose prevention and relapse support with a medical team immediately.
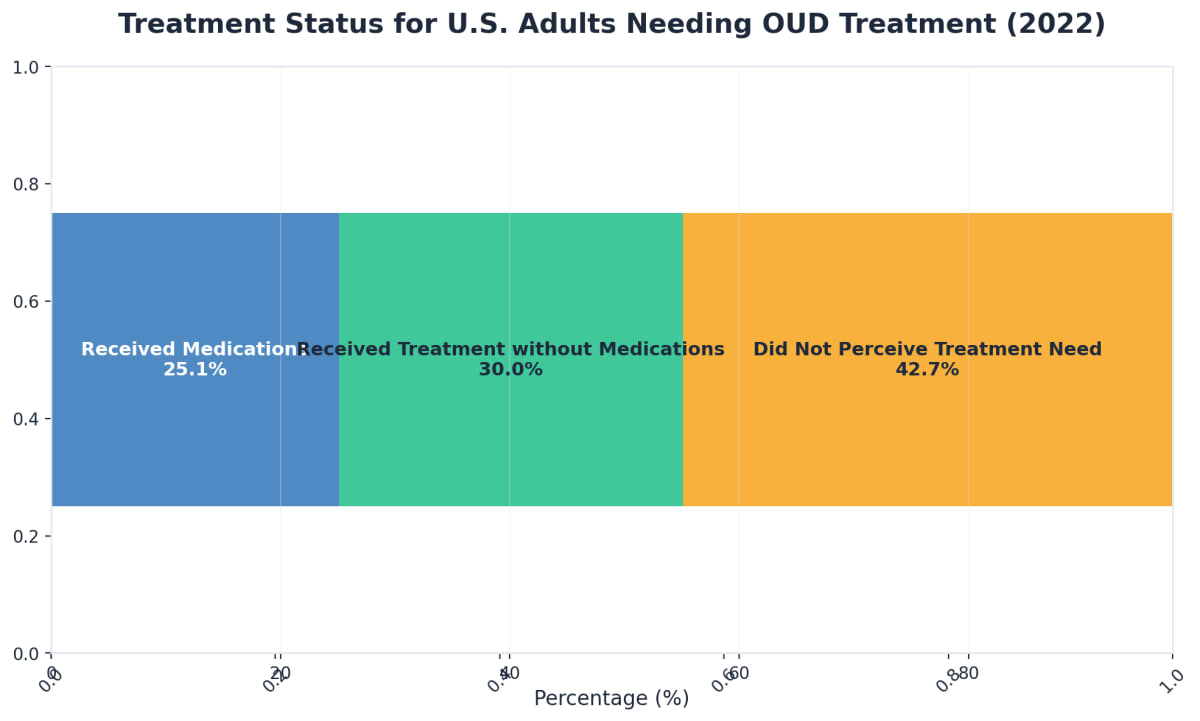
- Consider MAT: Ask about medication-assisted treatment (MAT) like buprenorphine or methadone. Only about 25% of people with opioid use disorder in the U.S. receive these life-saving medications5, 7.
- Create a safety plan: Work with Arista Recovery to establish a plan that includes naloxone access and ongoing support before leaving detox.
Benzodiazepine and Stimulant Withdrawal
Benzo Withdrawal: Seizure Risk Factors
Mistake 7: Stopping Benzos Suddenly and Missing Seizure Warning Signs
Stopping benzodiazepines “cold turkey” is incredibly risky. About 10-15% of long-term users face protracted withdrawal, including seizures, if they stop suddenly8. Early signs of detoxing include anxiety and insomnia, but these can rapidly escalate.
911 immediately.
What to do instead:
- Never stop abruptly: Always consult a doctor or Arista Recovery for a tapering plan.
- Monitor closely: Watch for increasing anxiety, shakiness, or confusion.
Meth and Cocaine Psychological Symptoms
Mistake 8: Overlooking the Psychological Signs of Meth and Cocaine Detox
With stimulants like methamphetamine or cocaine, the most severe dangers are often psychological rather than physical. Withdrawal can trigger intense mood swings, paranoia, deep depression, and hallucinations. These symptoms can persist for weeks, creating a mental health crisis10.
What to do instead:
- Watch for mood changes: Be alert to severe fatigue or sudden isolation.
- Take threats seriously: Any talk of hopelessness or self-harm is a medical emergency.
- Seek professional support: Reach out to Arista Recovery or a mental health professional in Ohio immediately if these signs appear.
- Prevent isolation: Check in regularly and encourage basic self-care routines like eating and resting.
Frequently Asked Questions
How do I know if my loved one needs to go to the emergency room during withdrawal?
If your loved one is showing signs of detoxing—like confusion, seizures, trouble breathing, chest pain, hallucinations, or passing out—don’t wait. These are all medical emergencies that can be life-threatening, especially during alcohol or benzodiazepine withdrawal12. In Ohio, experts recommend going to the emergency room if symptoms get worse fast, or if the person can’t stay awake, communicate clearly, or starts acting very differently. Call 911 right away for severe symptoms. When in doubt, it’s always safer to seek help. Arista Recovery can guide you and connect you to the right Ohio emergency care if you’re unsure.
Does insurance in Ohio cover medically supervised detox programs?
Yes, most insurance plans in Ohio—including Medicaid, Medicare, and commercial options like Aetna or Blue Cross Blue Shield—typically cover medically supervised detox programs when they’re deemed medically necessary12. Coverage may include both inpatient and outpatient detox, depending on the plan and the severity of the withdrawal symptoms. If you or your loved one is experiencing signs of detoxing, it’s a good idea to call your insurance provider or contact a treatment center like Arista Recovery. Their team can help you verify benefits and explain what costs are covered, so you can focus on safety and recovery instead of paperwork.
Can someone safely detox at home with family support instead of going to a facility?
Detoxing at home in Ohio, even with caring family support, is rarely safe for most substances. The warning signs of detoxing—such as confusion, seizures, or hallucinations—can come on quickly and become life-threatening, especially with alcohol, benzodiazepines, or opioids18. Families often miss these critical symptoms or don’t have the tools to respond. Medical detox centers like Arista Recovery provide constant monitoring, medications to ease symptoms, and emergency care if things go wrong. If you notice any severe signs of detoxing, don’t wait. Reach out to a professional in Ohio for guidance. Medical supervision gives the best chance for a safe and lasting recovery.
What happens if withdrawal symptoms return weeks after completing detox?
It’s possible for withdrawal symptoms—sometimes called post-acute withdrawal syndrome (PAWS)—to return weeks or even months after detox, especially with substances like benzodiazepines or alcohol8. These delayed signs of detoxing might include anxiety, trouble sleeping, mood swings, or body aches. While these symptoms can be scary, they’re often a normal part of the brain and body healing. If symptoms come back, reach out to Arista Recovery or your Ohio treatment provider right away. They can help you manage symptoms safely, adjust your recovery plan, and make sure nothing more serious is going on.
How long does medically supervised detox typically last in Ohio treatment centers?
Medically supervised detox in Ohio treatment centers usually lasts between 3 and 7 days, but the exact length depends on the substance, how long it was used, and the severity of withdrawal symptoms. For alcohol and benzodiazepines, detox may take closer to a week, especially when there are strong signs of detoxing like seizures or confusion18. Opioid detox is often shorter, but some people may need extra time for stabilization. Arista Recovery in Ohio tailors each detox plan to individual needs, with medical staff monitoring progress and adjusting care as needed. After detox, continued support is key for lasting recovery.
What medications are used to manage withdrawal symptoms safely?
Medical professionals in Ohio use different medications to make withdrawal safer and more comfortable, depending on the substance. For alcohol withdrawal, benzodiazepines like diazepam or lorazepam are often given to prevent seizures and calm the nervous system1. Opioid withdrawal can be managed with buprenorphine or methadone, which help reduce cravings and ease symptoms—these are known as medication-assisted treatments and are proven to save lives5. For benzodiazepine detox, doctors usually recommend a slow taper rather than stopping suddenly, sometimes using longer-acting benzos to make the process gentler8. If you see signs of detoxing, reach out to Arista Recovery in Ohio for guidance on safe, supervised care.
How can families support someone through the detox process without enabling?
Supporting someone through detox in Ohio means walking a careful line between being helpful and not enabling unhealthy behaviors. Start by learning the signs of detoxing, such as mood swings, sweating, or confusion. Offer encouragement and a safe environment, but don’t make excuses for risky choices or ignore serious symptoms. Set clear boundaries—for example, help with meals and rides to appointments, but avoid covering up mistakes or giving money that could be misused. Stay connected with medical professionals, like those at Arista Recovery, to ask questions and get advice if you’re unsure. Family support improves recovery outcomes when it balances care with accountability1.
Conclusion
Recovery from addiction is deeply personal, and finding the right path forward takes courage and support. Whether you’re exploring options for yourself or someone you care about, understanding the different levels of care available helps you make informed decisions that align with your unique needs and circumstances.
From medical detox and residential treatment to partial hospitalization programs (PHP), intensive outpatient programs (IOP), and standard outpatient care, Ohio offers a complete continuum of treatment options designed to meet people wherever they are in their recovery journey. Each level provides specific tools and support systems that address different stages of healing. The key is matching your current situation—considering factors like substance use severity, medical needs, living environment stability, and support system strength—with the appropriate intensity of care.
Remember that seeking help is a sign of strength, not weakness. Recovery is possible, and you don’t have to navigate this journey alone. If you’re ready to explore treatment options or have questions about which level of care might be right for you or your loved one, contact the Ohio Department of Mental Health and Addiction Services’ CareLine at 1-877-275-6364 for free, confidential guidance 24/7. You can also reach out to SAMHSA’s National Helpline at 1-800-662-4357 to connect with local treatment providers who can assess your needs and recommend the most appropriate starting point for your recovery journey.
References
- Understanding Alcohol Withdrawal – National Institute on Alcohol Abuse and Alcoholism (NIAAA). https://www.niaaa.nih.gov/publications/brochures-and-fact-sheets/understanding-alcohol-withdrawal
- Alcohol Withdrawal: Symptoms and Causes – Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/alcohol-withdrawal/symptoms-causes/syc-20353014
- Delirium Tremens: What It Is, Causes, Symptoms & Treatment – Cleveland Clinic. https://www.clevelandclinic.org/health/diseases/25052-delirium-tremens
- Opioid Withdrawal – StatPearls – National Center for Biotechnology Information (NCBI). https://www.ncbi.nlm.nih.gov/books/NBK526012/
- Medications for Opioid Use Disorder – National Institute on Drug Abuse (NIDA). https://nida.nih.gov/research-topics/medications-opioid-use-disorder
- FDA Identifies Serious Harm from Sudden Discontinuation of Opioid Pain Medicines – U.S. Food and Drug Administration. https://www.fda.gov/drugs/drug-safety-and-availability/fda-identifies-harm-reported-sudden-discontinuation-opioid-pain-medicines-and-requires-label-changes
- Treatment for Opioid Use Disorder: Population Estimates – Centers for Disease Control and Prevention (CDC). https://www.cdc.gov/mmwr/volumes/73/wr/mm7325a1.htm
- Protracted Withdrawal Syndrome (PWS) / Post-Acute Withdrawal Syndrome (PAWS) – BenzoInfo. https://www.benzoinfo.com/protracted-withdrawal-syndrome/
- Mortality and Alcohol-Related Morbidity in Patients with Delirium Tremens, Alcohol Withdrawal State or Alcohol Dependence – Norwegian Register Study. https://onlinelibrary.wiley.com/doi/10.1111/add.16297
- Withdrawal from Methamphetamine – Alberta Health Services. https://www.myhealth.alberta.ca/alberta/Pages/Methamphetamine-what-to-expect-when-someone-quits.aspx
- SAMHSA National Helpline. https://www.samhsa.gov/find-help/national-helpline
- U.S. Food and Drug Administration (FDA). https://www.fda.gov/

