Key Takeaways: Your Path to Healing
- Assess Your Safety: If you feel unsafe or cannot manage daily tasks, residential care provides the 24/7 support needed to stabilize.
- Choose Evidence-Based Care: Look for programs offering CPT, PE, or EMDR, as these are the gold standards for recovery.
- Demand Integrated Treatment: If you struggle with addiction or depression alongside trauma, ensure your provider treats both simultaneously for lasting results.
- Know Your Timeline: Most people see significant improvement within 6 months; patience and consistency are your best tools.
Understanding PTSD and Its Impact in Ohio
What PTSD Is and Who It Affects
In this section, you’ll learn what PTSD really means and who can be affected—especially here in Ohio. You’ll know you’ve learned it when you can explain PTSD to someone else and recognize that it doesn’t just impact one kind of person. Finding effective PTSD treatment in Ohio starts with understanding that this is a biological response, not a character flaw.
PTSD, or post-traumatic stress disorder, is a mental health condition that can happen after someone faces or witnesses a traumatic event. This might be a serious accident, violence, natural disaster, or even something that happens on the job. PTSD isn’t just about the event itself; it’s about how your brain and body respond and hold onto those memories.
Common symptoms often include:
- Intrusive Memories: Flashbacks or nightmares that feel real.
- Avoidance: Staying away from places or people that remind you of the trauma.
- Hyperarousal: Feeling jumpy, on edge, or having trouble sleeping.
- Negative Mood: Persistent feelings of guilt, fear, or hopelessness5.
Anyone can develop PTSD. In Ohio, it’s seen among veterans, first responders, survivors of accidents or violence, and even children who have experienced trauma. Nationally, about 3.6% of adults have PTSD each year, but women are nearly three times as likely as men to be affected3. For veterans and first responders, the numbers are even higher—almost one in three first responders develop PTSD during their career9.
Practice This: Try explaining what PTSD is in your own words to a friend or family member. If you can do that, you’re ready for the next level!
Next, we’ll look at how PTSD actually changes the brain and why those changes matter for recovery.
How PTSD Changes Your Brain
In this section, you’ll learn how PTSD actually changes your brain, and why those changes are important for recovery. You’ll know you’ve learned it when you can describe how the brain’s alarm system gets stuck on high alert after trauma, and why that’s not your fault.
Think of your brain like a smoke detector. After trauma, certain parts can get rewired:
| Brain Area | Function | Impact of PTSD |
|---|---|---|
| Amygdala | Senses danger (The Alarm) | Stays stuck in emergency mode, causing constant anxiety. |
| Hippocampus | Organizes memories (The Librarian) | Struggles to sort memories, making past trauma feel like it’s happening now. |
| Prefrontal Cortex | Decision making (The CEO) | Becomes weaker, making it harder to calm down or think clearly5. |
These changes in the brain aren’t permanent. With the right PTSD treatment in Ohio, like therapy and support at Arista, your brain can heal and relearn how to respond to stress in a healthier way1.
Practice This: Draw a simple diagram of a brain and label the amygdala, hippocampus, and prefrontal cortex. Explain to someone how each part is affected by trauma.
Next, let’s explore what therapies actually work to help your brain recover.
Evidence-Based Therapies for PTSD Treatment in Ohio
Cognitive Processing Therapy Explained
Here, you’ll discover how Cognitive Processing Therapy (CPT) works and why it’s one of the main evidence-based options for PTSD treatment in Ohio. You’ll know you’ve learned it when you can explain how CPT helps people challenge the thoughts and beliefs that keep trauma “stuck” and recognize the steps involved in the process.
CPT is a type of talk therapy that helps you look at how trauma has changed the way you see yourself, others, and the world. Imagine your brain like a puzzle—after trauma, some pieces might not fit right. CPT helps you notice and question thoughts that make you feel unsafe, guilty, or hopeless. Over 80% of people who complete CPT or a similar therapy experience significant improvement in symptoms1.
In Ohio, CPT is available at many treatment centers, including Arista, and is used with both adults and teens. Sessions often involve learning about PTSD, writing about your trauma, and practicing new ways to think about what happened. The goal is to help you reclaim your sense of safety and control, so trauma doesn’t define your life.
Practice This: Take a moment to write down a thought you have about your trauma. Ask yourself: Does this thought help me heal, or hold me back? You’re ready for the next level when you can spot an unhelpful thought and challenge it with a more balanced one.
Prolonged Exposure and EMDR Options
In this section, you’ll learn how Prolonged Exposure (PE) and Eye Movement Desensitization and Reprocessing (EMDR) work as evidence-based tools for PTSD treatment in Ohio. You’ll know you’ve learned it when you can explain what happens during these therapies and decide which might feel right for you or your loved one.
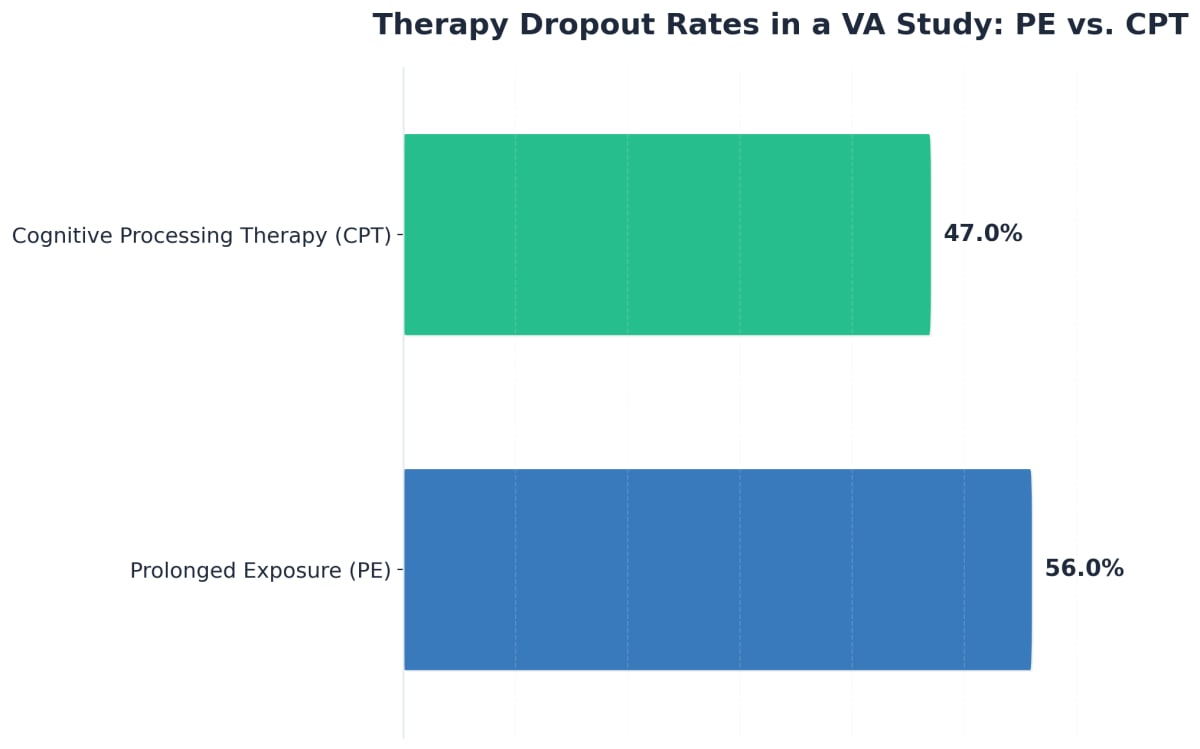
Think of PE as helping you gently face the memories or situations you’ve been avoiding. In PE, a trained therapist guides you to talk through your trauma in a safe, step-by-step way, helping your brain realize you’re not in danger anymore. This process lowers anxiety over time, and over 80% of people who complete PE or similar therapies see major symptom improvement1. A major VA study found both PE and other therapies effective, so finding the right fit matters7.
EMDR takes a different approach. During sessions, you’ll focus on parts of your trauma while following a therapist’s moving hand or another type of gentle, back-and-forth motion. This helps your brain “re-file” painful memories, making them feel less overwhelming6. EMDR is recognized worldwide as a proven PTSD treatment, including here in Ohio.
Practice This: Write down any worries or questions you have about facing trauma memories. Bring them to your next therapy session, or talk them over with a supportive friend or family member.
You’re ready for the next level when you can describe the basics of both PE and EMDR and feel confident asking a provider, like Arista, which might fit your needs best.
Treating PTSD with Co-Occurring Conditions
Why Integrated Treatment Matters
In this section, you’ll discover why treating PTSD together with other conditions—like addiction or depression—makes a real difference for long-term healing. You’ll know you’ve learned it when you can explain why focusing on both at the same time is safer and works better than tackling them one after the other.
“Imagine trying to patch a leaky boat but only fixing one hole while water pours in from another. That’s what happens when PTSD and substance use or depression are treated separately.”
In Ohio, nearly 45% of people with PTSD also struggle with a substance use disorder11. The latest research shows that integrated treatment—where both PTSD and other conditions are addressed together—leads to better outcomes, lower relapse rates, and improved quality of life8. This approach helps you build healthy coping skills and tackle the roots of both problems at once, rather than just managing symptoms.
Arista Recovery uses this integrated model for PTSD treatment in Ohio, so you don’t have to choose which challenge to face first. Your care team will help you set goals that make sense for your whole life, not just your diagnosis.
Practice This: Make a list of all the challenges you’re facing (not just PTSD). Bring it to your next appointment to talk about how they connect and how you can start addressing them together. You’re ready for the next level when you can describe why integrated care is important, especially if you have more than one diagnosis.
Next, we’ll see how combining therapy and medication supports recovery when multiple conditions are present.
Medication and Therapy Combined
In this section, you’ll learn how combining medication and therapy can help people with PTSD and other conditions heal more fully. You’ll know you’ve learned it when you can explain why a mix of both can be more effective than using just one approach—especially if you or your loved one are dealing with depression, anxiety, or addiction along with PTSD.
Think of therapy and medication as two parts of the same toolkit. While therapy (like CPT or EMDR) helps you process trauma and build new coping skills, medication can help manage intense symptoms that make it hard to focus or stick with therapy. For many in Ohio, especially those facing multiple challenges, medications such as SSRIs or SNRIs are used to ease anxiety, depression, and sleep problems2. This can make therapy more approachable and successful.
Research shows that for people with co-occurring PTSD and substance use or depression, treatment works best when talk therapy and medications are used together8. Arista Recovery uses this combined approach for PTSD treatment in Ohio, so your care plan is tailored to your unique needs.
Practice This: Make a list of your current symptoms and any medications you take. Bring it to your next session to talk about if adjustments or new supports might help you get more from therapy. You’re ready for the next level when you can describe how both therapy and medication support your recovery, not just one or the other.
What to Expect During Your Recovery
Treatment Settings and Timeline
In this section, you’ll discover what types of settings are available for PTSD treatment in Ohio and how long recovery might take. You’ll know you’ve learned it when you can describe the difference between outpatient, intensive outpatient, and residential treatment—and set realistic expectations for your healing journey.
PTSD treatment in Ohio can happen in several places. The right setting depends on your symptoms, safety, and whether you’re also dealing with things like depression or substance use:
| Setting | Best For… | Typical Structure |
|---|---|---|
| Outpatient | Stable housing, strong support system, mild to moderate symptoms. | Therapy 1-2 times per week. |
| Intensive Outpatient (IOP) | Need more structure but can live at home safely. | Therapy 3-5 days per week for several hours. |
| Residential (Inpatient) | Safety concerns, severe symptoms, or co-occurring addiction. | 24/7 support in a safe facility. |
Most people begin to see real improvement within about six months of starting treatment, especially when using therapies like CPT or PE110. Long-term studies show that gains can last for years, so the work you put in now can pay off for a long time10. At Arista, your care team will help you find the setting and timeline that fits your needs—and support you at every step.
Practice This: Make a list of questions you have about different treatment settings and bring them to your next appointment. You’re ready for the next level when you can explain which setting might help you feel most supported.
Next, we’ll talk about how to overcome barriers and keep hope alive during your recovery.
Overcoming Barriers and Building Hope
In this section, you’ll learn how to spot common barriers in PTSD recovery and discover real ways to keep hope alive while you heal. You’ll know you’ve learned it when you can name at least two obstacles—and list at least one new way to overcome each.
Barriers like stigma, worries about treatment, or even just finding the right provider in Ohio can make recovery feel tough. Did you know that over half of people starting gold-standard PTSD therapies like Prolonged Exposure or Cognitive Processing Therapy drop out before finishing? This shows how normal it is to hit roadblocks along the way7. In Ohio, provider shortages and long waitlists can add to the stress, but support is available.
Building hope starts with small steps. Try writing down your progress each week, even if it’s just “I showed up to my appointment” or “I reached out for help.” At Arista, we encourage you to bring a support person to sessions and to talk openly about struggles—no shame, just teamwork.
Practice This: List one barrier you’re facing right now, like self-doubt or transportation. Then, brainstorm one practical solution, such as asking for help with rides or joining a telehealth session.
You’re ready for the next level when you can ask for support and remember that setbacks are a normal part of PTSD treatment in Ohio. Next, we’ll show you how to find the right care team and resources to support your journey.
Frequently Asked Questions
Will my insurance cover PTSD treatment in Ohio?
Most insurance plans in Ohio, including Medicaid and private insurers, do cover PTSD treatment, but coverage details can vary. Under the Mental Health Parity and Addiction Equity Act, insurance must cover mental health care, including evidence-based PTSD treatment in Ohio, on the same level as other medical care1. That means you can usually get help for therapy and sometimes medication, too. It’s smart to call your insurance provider for specifics, or reach out to a trusted team like Arista—our staff can help you understand your options and check your benefits so there are no surprises. Recovery support should be within reach for you and your family.
What if I’m worried about dropping out of therapy before I finish?
Feeling worried about dropping out of therapy is common, and you’re not alone—studies show that nearly half of people starting top therapies like CPT or Prolonged Exposure don’t finish the full course7. In Ohio, barriers like busy schedules, transportation, or even feeling discouraged can get in the way. The good news: talking honestly with your therapist about your worries can help create a plan that fits your life, not just the treatment manual. At Arista, we work with you to set realistic goals and adjust as needed, so you feel supported even if things get tough. Recovery is a journey, not a race.
Can I receive PTSD treatment through telehealth in Ohio?
Yes, you can receive PTSD treatment through telehealth in Ohio. Many providers, including Arista, offer virtual therapy sessions using secure video or phone calls. Research confirms that evidence-based therapies like Cognitive Processing Therapy (CPT) and Prolonged Exposure (PE) are just as effective when delivered online as they are in person1. Telehealth can make it easier to access care if you have a busy schedule, transportation challenges, or live far from a clinic. If you’re interested in starting PTSD treatment in Ohio from home, reach out to Arista’s team—they can help you get set up with virtual appointments and explain how the process works.
How do I know if I need residential treatment or outpatient care?
Choosing between residential and outpatient care for PTSD treatment in Ohio depends on your symptoms, safety, and daily needs. Residential treatment offers 24/7 support if you’re feeling unsafe, struggling with daily activities, or dealing with severe symptoms that make outpatient care too tough. Outpatient care works well if you have stable housing, a strong support system, and can manage daily life while attending therapy a few times a week. Research shows both settings use evidence-based therapies like Cognitive Processing Therapy and Prolonged Exposure, so the main difference is the level of support1. Arista’s care team can help you decide which path is best for you.
Is it safe to work on my trauma if I’m also struggling with addiction?
Yes, it is safe—and often recommended—to work on trauma even if you’re struggling with addiction, as long as you have the right support. New research shows that treating PTSD and addiction together (called integrated treatment) is safer and leads to better results than trying to tackle one before the other811. In Ohio, many programs, including Arista, use this approach so you don’t have to choose between getting help for trauma or for substance use. Your care team will help you move at a pace that feels right and adjust your plan if things get overwhelming. You deserve support for all parts of your recovery.
What happens if my symptoms get worse during treatment?
It can feel scary if your PTSD symptoms get worse during treatment, but this is actually a normal part of the healing process for many people. Sometimes, talking about trauma or starting new therapies can bring up strong feelings or memories before things start to improve1. In Ohio, your care team at Arista is trained to help you manage these ups and downs. Let your therapist know right away if things feel harder—together, you can adjust your plan and add extra support if needed. You’re not alone, and reaching out for help is a sign of strength, not failure.
How can my family support me during PTSD treatment?
Family support can make a big difference during PTSD treatment in Ohio. You might find it helpful when loved ones listen without judgment, encourage you to attend therapy, and respect your need for space when things feel tough. Sometimes, family members join sessions to learn about PTSD or practice new skills together—this is often encouraged at Arista and can help everyone understand what you’re going through1. Let your family know that showing up, asking how they can help, and learning about PTSD are all ways to support your healing. Remind them that recovery is a team effort, and just being there matters.
Finding Comprehensive PTSD Treatment in Ohio
With over 200 mental health facilities across Ohio, choosing the right PTSD treatment can feel overwhelming. When searching for care, finding a provider that offers truly comprehensive treatment makes all the difference in your recovery journey. Comprehensive care goes beyond standard weekly therapy sessions—it includes coordinated treatment that addresses the full spectrum of trauma’s impact on your life (mental, physical, emotional, and social), such as integrated medical care for trauma-related health issues and structured support between sessions, rather than isolated appointments with limited follow-up.
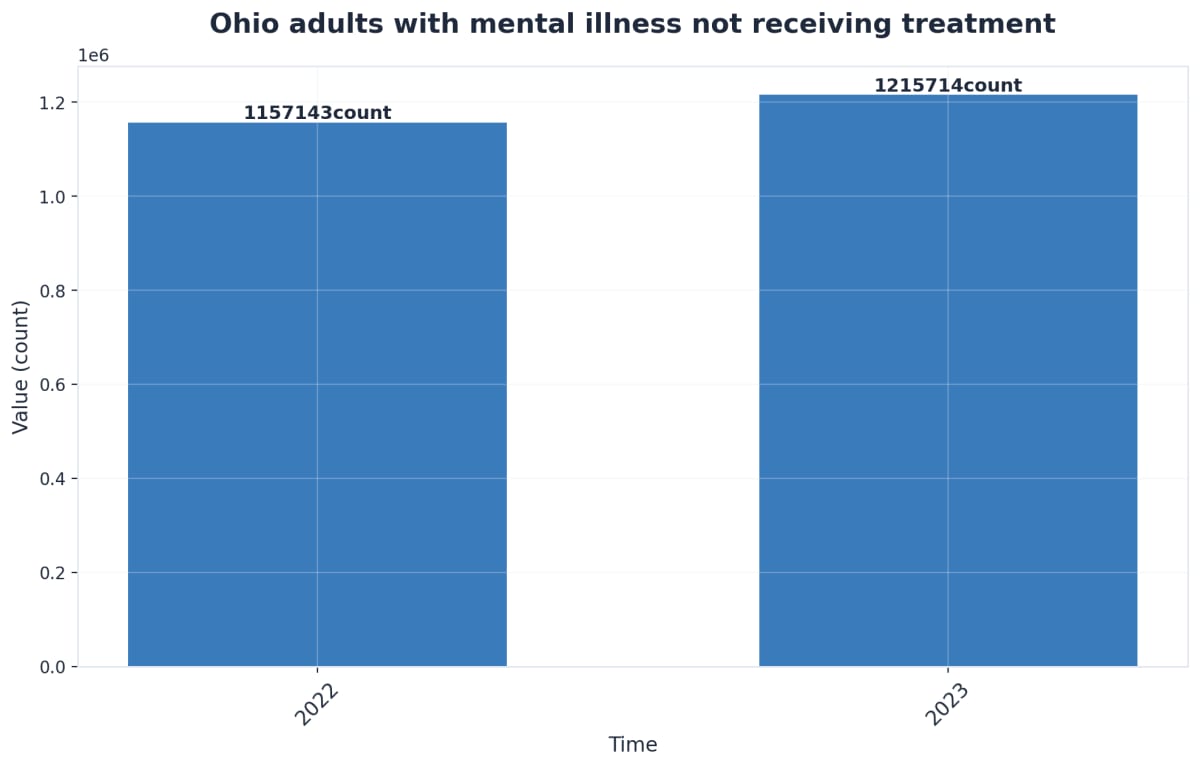
So what should comprehensive PTSD care actually include? Effective treatment should combine evidence-based therapies like Cognitive Processing Therapy and EMDR, along with holistic approaches such as mindfulness practices, art therapy, and wellness activities. The best programs also provide family education and support, recognizing that trauma affects your entire support system.
Arista Recovery offers specialized PTSD treatment in Ohio designed specifically for residents seeking lasting healing. Our integrated approach combines proven clinical methods with personalized care plans tailored to your unique experiences and goals. From initial assessment through aftercare planning, we walk alongside you every step of the way.
Recovery from PTSD is absolutely possible with the right support. Whether you’re in Columbus, Cleveland, Cincinnati, or anywhere across Ohio, compassionate, expert care is available to help you reclaim your life and build the future you deserve.
References
- Clinical Practice Guideline for the Treatment of Posttraumatic Stress Disorder. https://www.apa.org/ptsd-guideline
- Medications for PTSD. https://www.apa.org/ptsd-guideline/treatments/medications
- Post-Traumatic Stress Disorder (PTSD). https://www.nimh.nih.gov/health/statistics/post-traumatic-stress-disorder-ptsd
- Post-traumatic stress disorder. https://www.who.int/news-room/fact-sheets/detail/post-traumatic-stress-disorder
- Post-traumatic stress disorder (PTSD) – Symptoms and causes. https://www.mayoclinic.org/diseases-conditions/post-traumatic-stress-disorder/symptoms-causes/syc-20355967
- EMDR Therapy: What It Is, Procedure & Effectiveness. https://my.clevelandclinic.org/health/treatments/22641-emdr-therapy
- Prolonged exposure or cognitive processing therapy? https://www.research.va.gov/currents/0122-Prolonged-exposure-or-cognitive-processing-therapy.cfm
- Concurrent Treatment of Substance Use and PTSD. https://pmc.ncbi.nlm.nih.gov/articles/PMC4928573/
- Conceptualization, Assessment, and Treatment of Traumatic Stress in First Responders. https://pmc.ncbi.nlm.nih.gov/articles/PMC6624844/
- Long-Term Outcomes of Cognitive-Behavioral Treatments for PTSD. https://pmc.ncbi.nlm.nih.gov/articles/PMC3336190/
- Treatment of Co-Occurring PTSD and Substance Use Disorder in VA. https://www.ptsd.va.gov/professional/treat/cooccurring/tx_sud_va.asp

