Key Takeaways: Your Decision Path
- Assess Your Risk Score: If you have used fentanyl, have a history of seizures, or lack a stable home, inpatient medical supervision is non-negotiable for safety.
- Choose Your Setting: Compare Inpatient (24/7 monitoring, best for high risk) vs. Outpatient (daily visits, best for mild symptoms and strong family support).
- Immediate Action: Call for insurance verification today. Ohio mandates coverage for medically necessary detox, and facilities like Arista can verify your benefits in minutes.
Understanding Opioid Detox Ohio and Recovery
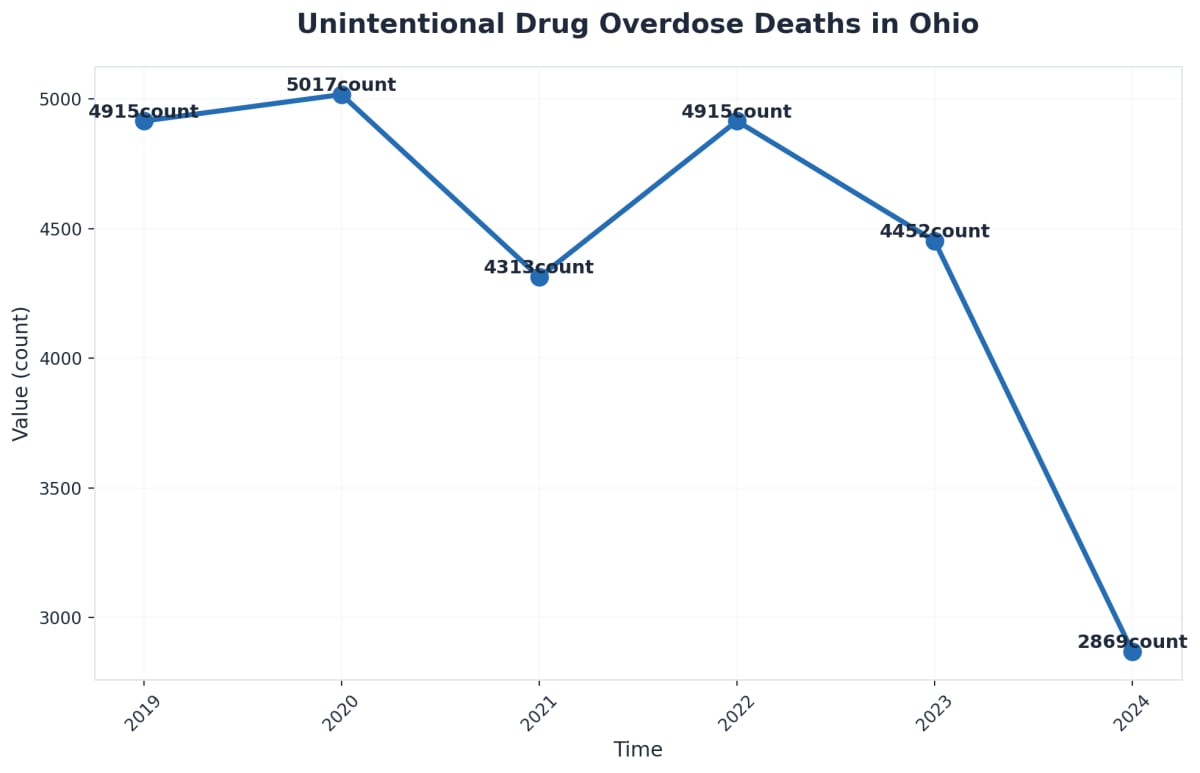
Opioid detox is the critical first step in breaking free from opioid dependence. Throughout the state, where opioid-related overdose deaths have remained persistently high, understanding what opioid detox Ohio involves can guide you or someone you love toward that essential first step in recovery. In 2022, Ohio reported over 4,000 unintentional drug overdose deaths, with opioids involved in approximately 80% of these fatalities, underscoring the urgent need for accessible detox and treatment services.
During opioid detox, your body clears itself of opioids while managing withdrawal symptoms. These symptoms typically begin within 6-12 hours for short-acting opioids like heroin or within 24-48 hours for long-acting opioids like methadone. You might experience muscle aches, anxiety, sweating, nausea, and intense cravings. While opioid withdrawal isn’t typically life-threatening, the discomfort can be severe enough to derail recovery attempts without proper support.
Medical detox programs across Ohio provide 24/7 supervision and medication-assisted treatment to ease these symptoms. Medications like buprenorphine, methadone, or naltrexone can significantly reduce cravings and withdrawal discomfort, making the process more manageable. This medical support dramatically increases your chances of completing detox successfully compared to attempting withdrawal alone.
Ohio has expanded access to these services through RecoveryOhio, a statewide initiative that coordinates prevention, treatment, and recovery resources, and Project DAWN (Deaths Avoided With Naloxone), which distributes naloxone kits to reverse overdoses throughout communities.
Ohio offers various detox settings, from inpatient facilities to outpatient programs. Inpatient detox provides the most intensive support, with round-the-clock medical care in a structured environment. This option works best for those who’ve struggled with severe addiction, have co-occurring mental health conditions, or lack a stable home environment. Outpatient detox allows you to live at home while attending regular medical appointments, which may suit those with milder dependence and strong family support.
The detox process typically lasts 5-10 days, though your timeline depends on factors like which opioid has been in your system, how long the dependence has lasted, and your overall health. Remember that detox addresses only the physical dependence—comprehensive treatment following detox is essential for addressing the psychological aspects of addiction and building lasting recovery skills.
What Medical Detox Really Means
Medical detox in Ohio isn’t just about checking into a clinic—it means you’re getting care from trained professionals using proven methods to handle opioid withdrawal safely. This process is closely regulated across Ohio, so if you’re seeking help, you’ll find programs that use FDA-approved medications like buprenorphine and methadone, along with medical monitoring for your comfort and safety1.
These medications are shown to cut the risk of overdose death in half compared to going without treatment5. The main goal is to get your body through withdrawal in a way that’s as safe and steady as possible, while also preparing you for ongoing recovery. When you hear “medical detox,” think of a supportive medical team, round-the-clock supervision, and a plan that doesn’t leave you on your own after the first few days.
Three Essential Components of Safe Detox
Safe opioid detox in Ohio always includes three key parts: evaluation, stabilization, and a plan for what comes next.
- Evaluation: A medical team checks your overall health and substance use history to spot any risks.
- Stabilization: Using FDA-approved medications—like buprenorphine or methadone—to ease withdrawal and keep you comfortable1, 6.
- Transition of Care: Connecting you to ongoing treatment so you’re not left without support after those first tough days8.
Programs that skip any of these steps aren’t complete and may not be safe. When looking for opioid detox Ohio, prioritize places that walk you through all three.
Why Detox Alone Isn’t Treatment
“Detox by itself isn’t a full treatment for opioid addiction. Medical detox clears opioids from your system and helps manage withdrawal, yet studies show only about 20% of people who leave detox in a hospital get further substance abuse treatment.”7
Without ongoing support, the risks of relapse and overdose stay high. A safe opioid detox in Ohio should always connect you to counseling, medication-assisted treatment, or a longer-term recovery plan8. This solution fits people who want lasting change, not just short-term relief. Arista Recovery teams up with you to plan next steps, so you’re supported well beyond those first days.
Ohio’s Opioid Crisis Landscape in 2025
Ohio’s fight against opioid addiction looks different in 2025 than it did just a few years ago. The rise of fentanyl—a highly potent synthetic opioid—now plays a part in 78% of overdose deaths statewide, making detox even more complex2. Thankfully, overdose deaths dropped by 9% from 2022 to 2023, and nonfatal overdose ER visits are down, showing that expanded access to care and harm reduction tools like naloxone are working4.
The number of opioid detox providers in Ohio has jumped from 35 in 2019 to 125 in 2023, giving you more choices for safe, regulated care. This approach works best when you have a trusted resource—like Arista—by your side to help navigate these options.
Fentanyl’s Impact on Withdrawal Timelines
Fentanyl changes how withdrawal feels and how long it lasts in opioid detox Ohio. Because fentanyl is a much stronger opioid than older prescription painkillers or heroin, it stays in your body longer and can make withdrawal symptoms start later and last several days instead of just two or three.
Many Ohio detox programs now see people needing medical supervision for five to seven days or more, especially when fentanyl is involved. This method works when you want to avoid the risk of sudden cravings or dangerous withdrawal at home. Experts in Ohio have found that standard detox timelines don’t always fit fentanyl, so staff may adjust medication or observation plans to keep you safe2.
Recent Progress in Overdose Prevention
Ohio has made notable strides in overdose prevention, helping to make opioid detox Ohio safer and more hopeful for families. Since 2014, Project DAWN has distributed nearly 90,000 naloxone kits and reported about 11,000 overdose reversals—saving thousands of lives3.
By October 2024, the network grew to over 221 naloxone programs, now reaching about 83 of Ohio’s 88 counties. This expansion means that more people across the state can access life-saving medications and overdose education. As a result, nonfatal overdose ER visits dropped from 62.7 per month in August 2023 to 41.1 in August 2025, showing how community support and harm reduction tools are making a real impact4.
Self-Assessment: Is Medical Detox Right for You?
Deciding whether you need medical detox is one of the most important choices you’ll make on this healing journey. While every situation is unique, certain factors clearly indicate when medical supervision becomes essential for safety and success.

Medical detox is typically recommended when opioids have been used regularly for several weeks or longer. The duration and intensity of use directly impact withdrawal severity. For those who’ve attempted to quit independently before and experienced severe symptoms—or relapsed quickly because the discomfort became unbearable—that’s a strong signal that medical support could make the difference this time.
Physical health also plays a crucial role in this decision. When underlying medical conditions like heart disease, diabetes, or respiratory issues are present, withdrawal can create additional complications that require professional monitoring. Similarly, when multiple substances are being used alongside opioids, the detox process becomes more complex and potentially dangerous without medical oversight.
Consider the living environment as well. Is there a stable, supportive home where rest and healing can occur? Are there triggers or access to substances that might derail these efforts? When the home environment isn’t conducive to healing, a medical detox facility in your area provides the protected space needed to focus entirely on getting well.
Mental health concerns deserve equal attention. When depression, anxiety, or thoughts of self-harm are present, detoxing alone can intensify these feelings during an already vulnerable time. Medical detox programs offer psychiatric support alongside physical care, addressing the whole person rather than just the withdrawal symptoms.
Evaluating Your Withdrawal Risk Level
Start your evaluation with this simple tool: rate your withdrawal risk level as low, moderate, or high. Ask yourself:
- Have you had severe withdrawal before?
- Do you have health issues like heart or lung problems?
- Is there a history of seizures or mental health struggles?
In Ohio, programs for opioid detox use these questions to match you with the safest care, because withdrawal can be unpredictable—especially with fentanyl now in so many street drugs2. This approach is ideal for anyone who isn’t sure how their body will react or who may have had trouble with withdrawal at home. Evidence shows that medically supervised detox greatly lowers the risk of complications and keeps you safer during tough symptoms1.
Medical Complications That Require Supervision
Some health issues make medical supervision during opioid detox Ohio not just helpful, but necessary. If you have heart problems, lung disease, or a past history of seizures, withdrawal can be especially risky. For example, opioid withdrawal can trigger changes in blood pressure or heart rate that are dangerous for people with cardiac conditions.
Liver or kidney problems may also affect how your body handles withdrawal medications, so close monitoring is needed1. In Ohio, programs for opioid detox look for these complications to make sure you get the safest care. Choosing a facility like Arista Recovery means you’ll have access to medical support for any complications, ensuring your comfort and safety throughout the detox process.
Social and Psychiatric Stability Factors
When thinking about opioid detox Ohio, social and psychiatric stability play a major role in keeping you safe. If your living situation isn’t steady—like not having a safe place to stay, or living with people who use drugs—it becomes much harder to stick to a detox plan. Unstable housing or lack of family support often means you’ll need a higher level of supervision.
Psychiatric factors are just as important: anyone with depression, anxiety, or a history of mental health crises is at greater risk for complications during withdrawal. Ohio’s guidelines state that ambulatory (outpatient) detox is only safe if you have enough social, medical, and psychiatric stability to manage your care and medications at home1. If you or your loved one faces challenges in these areas, Arista Recovery’s team can help you find the right structure for lasting success.
Determining Your Appropriate Care Setting
Choosing the safest setting for opioid detox Ohio starts with a quick decision guide: Do you have steady housing, strong family support, and mild withdrawal symptoms? If so, outpatient (ambulatory) detox may be a fit. If you’re facing severe symptoms, health complications, or unstable living conditions, a residential (inpatient) setting is safer.
Ohio’s guidelines require that outpatient detox is only offered if your social and medical situation is stable enough to manage care at home1. This solution fits people who can reliably attend clinic visits and handle their medications safely. For those with unpredictable health or support at home, inpatient care offers round-the-clock monitoring and immediate help if anything changes.
Ambulatory vs. Residential Detox Options
Let’s break down the main differences between ambulatory (outpatient) and residential (inpatient) opioid detox in Ohio:
| Feature | Ambulatory (Outpatient) | Residential (Inpatient) |
|---|---|---|
| Setting | Visit clinic for meds/check-ins, sleep at home. | Stay at facility 24/7 with round-the-clock care. |
| Best For | Mild symptoms, steady housing, strong support. | Severe symptoms, unstable housing, medical needs. |
| Disruption | Less disruptive to daily life/work. | Requires taking time off for full focus on recovery. |
Both options use the same evidence-based withdrawal management and medications for opioid detox Ohio. Programs like Arista Recovery help you weigh these choices, matching your needs with the safest setting and the right support team.
ASAM Criteria for Placement Decisions
The ASAM criteria (American Society of Addiction Medicine) is a tool used by Ohio treatment providers—including Arista Recovery—to help place you in the safest and most effective level of care for opioid detox Ohio. It looks at six areas: how severe your withdrawal symptoms are, your medical health, emotional or mental health, risk of relapse, living situation, and willingness to change.
Using these criteria, your care team can tell if outpatient detox is safe, or if you’d be better supported in a 24/7 inpatient setting10. For instance, this method works when someone has mild symptoms and a stable home—they may do well with ambulatory detox. But if you have severe withdrawal, health complications, or unstable housing, inpatient care is the safer choice.
Decision Framework: Choosing Safe Opioid Detox Ohio
Making the choice to pursue detox is deeply personal, but you don’t have to navigate it alone. A structured decision framework can guide your evaluation of available options and identify the safest path forward.
Start by assessing the severity of your withdrawal risk. When you’ve been using substances daily for months or years, or when you’ve experienced severe withdrawal symptoms in the past, medical supervision isn’t just recommended—it’s essential for your safety. Multiple levels of detox care exist throughout Ohio, from hospital-based programs to residential facilities, each designed to match different clinical needs.
Next, consider your support system and living environment. Will you have someone available 24/7 during withdrawal? Is your home environment conducive to healing, or does it contain triggers that might jeopardize your progress? For many people, stepping away from familiar surroundings provides the reset needed to break patterns and focus entirely on getting well.
Evaluate practical factors like insurance coverage and geographic accessibility. Most detox programs across Ohio accept major insurance plans, and verification specialists can clarify your benefits before admission. Location matters too—some people prefer facilities close to family, while others benefit from distance that creates healthy boundaries during the initial stages of treatment.
Finally, trust your instincts about timing. While “the perfect moment” rarely exists, recognizing that you need support is itself a powerful indicator that now is the time to act. Withdrawal symptoms won’t improve on their own, and delaying treatment often means prolonged suffering.
Essential Safety Standards to Verify
Use this quick verification checklist when choosing an opioid detox Ohio provider:
- Licensure: Confirm the facility is licensed by the State of Ohio with oversight for withdrawal management1.
- Medication: Make sure they offer FDA-approved medications such as buprenorphine, methadone, or naltrexone for opioid withdrawal6.
- Monitoring: Ask if 24/7 medical monitoring is available, especially for those with health risks or severe symptoms.
These safety standards matter because they lower the risk of complications and help keep your detox process on track. In Ohio, licensed programs must follow state guidelines for assessment, medication dosing, and ongoing care, so you know you’re not alone in this process1.
Ohio Regulatory Compliance Requirements
Ohio has clear regulatory compliance requirements for any opioid detox provider, and these rules are your best tool for spotting a trustworthy program. All licensed opioid detox Ohio centers must follow the Ohio Administrative Code Rule 4723-9-14, which sets strict standards for withdrawal management1. This means programs need state-approved assessment procedures, safe medication practices, and proper documentation.
Facilities also have to use validated tools—like the Clinical Opiate Withdrawal Scale (COWS)—to check symptoms and risks. If you’re searching for a safe detox, ask to see proof of state licensure and make sure staff can explain how they follow these rules. This solution fits anyone who wants peace of mind that their care is both legal and up to date with Ohio’s current guidelines.
Medication-Assisted Treatment Availability
When exploring opioid detox Ohio options, check that the facility offers medication-assisted treatment (MAT) with FDA-approved medications—namely buprenorphine, methadone, or naltrexone. MAT is proven to make detox safer and greatly reduce your risk of overdose death: using buprenorphine or methadone cuts that risk by about 50% compared to going without medication5, 6.
These medications help manage cravings and make withdrawal symptoms less severe, so you’re more comfortable and less likely to relapse. This approach works best when you want both medical safety and a real shot at long-term recovery. In Ohio, legitimate detox programs like Arista Recovery ensure you have access to MAT and a team that can explain the pros and cons of each option.
24/7 Medical Monitoring Capabilities
24/7 medical monitoring is a must-have for any reputable opioid detox Ohio program. This means there are medical professionals—like nurses or doctors—on-site all day and night, ready to handle withdrawal symptoms, check vital signs, and respond if a problem comes up. Since fentanyl is involved in most overdoses in Ohio, withdrawal can be unpredictable and even risky without this level of support2.
For example, if someone’s blood pressure spikes or they feel severe anxiety, trained staff can step in right away. Most Ohio guidelines require 24/7 monitoring for anyone with severe symptoms or health risks during opioid detox1. Arista Recovery’s round-the-clock care ensures you’re never alone, making your path to recovery safer and more comfortable.
Evaluating Treatment Continuity Plans
A strong opioid detox Ohio program always includes a clear plan for what happens after withdrawal. Here’s a quick tool: ask each provider if they help you transition to residential or outpatient care, offer counseling, and support both mental health and trauma needs.
Continuity matters—studies show only about 20% of people who complete hospital detox get additional substance abuse treatment, which puts them at higher risk for relapse7. Programs that make it easy to step into ongoing treatment, like those at Arista Recovery, help you stay on track with your recovery goals. This strategy suits people who want more than just a few days of support—it’s for families and individuals seeking real, lasting change.
Connection to Residential or Outpatient Care
When you’re looking into opioid detox Ohio, a crucial question to ask is: does the provider help you move smoothly into your next phase of care? A strong program should actively connect you to either residential treatment (where you stay onsite for more support) or outpatient care (where you visit the clinic but live at home).
This approach works best for people who want a real shot at long-term recovery—not just a few days of withdrawal support. In Ohio, only about 20% of people who finish hospital detox get follow-up substance abuse treatment, which leaves many at risk for relapse7. That’s why Arista Recovery and other trusted centers build seamless bridges from detox into ongoing care, whether you need the structure of inpatient rehab or the flexibility of outpatient therapy.
Dual Diagnosis and Trauma-Informed Services
When comparing opioid detox Ohio programs, make sure to ask about dual diagnosis and trauma-informed services. Dual diagnosis means the provider can treat both substance use and mental health conditions—like depression or anxiety—at the same time. Trauma-informed care ensures that staff understand how past trauma might affect withdrawal and recovery, and adjust their approach so you feel safe and respected.
This solution fits people who have experienced mental health struggles or trauma, which is very common among those seeking opioid detox. Ohio’s best programs, including Arista Recovery, offer counseling and support for these overlapping needs, following state guidelines that highlight the importance of integrated treatment1, 10.
Implementation Pathways for Different Situations
Once you’ve evaluated your situation using the decision framework above, the next step is identifying which implementation pathway aligns with your specific needs and circumstances. Throughout Ohio, several pathways lead to appropriate care, each designed to meet different needs and situations.
If you’re experiencing severe withdrawal symptoms or have a history of complicated detox, immediate medical attention is essential. Hospital-based detox programs across Ohio provide 24/7 monitoring and intervention. These settings are equipped to handle medical emergencies and offer the highest level of clinical support. You might access this care through your local emergency department or by calling ahead to facilities that specialize in addiction medicine.
For those with moderate risk factors, residential detox programs offer a structured environment with round-the-clock medical supervision in a more treatment-focused setting. These programs typically last 3-7 days and seamlessly transition into ongoing treatment. Facilities throughout Ohio provide this level of care with personalized medical protocols and therapeutic support from day one.
If your situation involves lower medical risk but you still need professional guidance, outpatient detox with daily check-ins might be appropriate. This pathway allows you to remain at home while receiving regular medical monitoring, medication management, and counseling support. However, this option requires a stable, substance-free living environment and strong family or community support.
For Individuals in Acute Crisis
Click to view the Crisis Action Tool
If you’re in acute crisis and need opioid detox Ohio right away, follow these steps:
- Call Immediately: Contact a licensed detox provider—such as Arista Recovery—for immediate help.
- Medical Stabilization: Ohio’s regulated centers are prepared to admit you quickly, especially if you’re experiencing severe withdrawal or fentanyl use complications1, 2.
- Intake Process: Programs will guide you through intake, check your medical/mental health, and start FDA-approved medications like buprenorphine or methadone to keep you safe6.
This route works well if you need rapid support—Ohio’s system is built for urgent intervention, and recovery begins the moment you reach out. As you move forward, it’s important to know how to access medical stabilization and handle insurance steps efficiently.
Immediate Access to Medical Stabilization
When you reach out for opioid detox Ohio during a crisis, immediate medical stabilization is the first priority. Licensed centers like Arista Recovery follow Ohio’s strict standards to admit you quickly, starting with a thorough check of your health and withdrawal symptoms. Medical staff use proven tools—like the Clinical Opiate Withdrawal Scale—to guide safe care and respond if complications come up1.
For people facing fentanyl-related withdrawal, this step can be life-saving, since fentanyl is now involved in 78% of overdose deaths in Ohio2. FDA-approved medications such as buprenorphine or methadone are started right away to ease symptoms and reduce overdose risk, cutting the chance of death by about 50% compared to going without treatment5.
Navigating Insurance Verification Quickly
When you’re seeking opioid detox Ohio during a crisis, handling insurance verification fast can make a big difference. Start by having your insurance card and ID ready—most licensed treatment centers, including Arista Recovery, have staff who can check your coverage within minutes. They’ll verify your benefits, help you understand what detox services are covered, and explain any steps or paperwork needed for approval1.
In Ohio, many insurers are required to cover medically necessary detox with FDA-approved medications, but exact benefits can vary. This method works when you want to avoid delays and focus on getting help quickly. Programs like Arista guide you through these details, so you don’t have to navigate insurance alone.
For Family Members Seeking Help
If you’re a family member seeking help for a loved one who needs opioid detox Ohio, you play a vital role—sometimes, just knowing where to start can make all the difference. Begin with this supportive action checklist:
- Learn the basics of withdrawal and treatment options in Ohio.
- Reach out to licensed providers like Arista Recovery for guidance on safe, evidence-based care.
- Prepare for an open, nonjudgmental conversation with your loved one.
Ohio’s network of regulated detox programs means you don’t have to guess about quality or safety—trusted centers follow strict standards to protect both patients and families1. This approach is ideal for families who want to be part of the solution and ensure their loved one gets real support, not just a quick fix.
How to Approach Your Loved One
Approaching a loved one about opioid detox Ohio can feel intimidating, but having a plan makes it easier. Start with this step-by-step approach tool:
- Pick a calm time to talk, away from stress or distractions.
- Use “I” statements—like, “I’m worried about your health”—to show care without blame.
- Listen as much as you speak; your loved one may have fears or questions about opioid withdrawal and detox.
- Share that Ohio has safe, regulated programs and that help is available from trusted providers like Arista Recovery1.
- Offer to help with the first steps, such as making a call or going to an appointment together.
This method works when you want to show support without judgment and create space for real conversation. In Ohio, families are often the bridge to life-saving care, especially with the rise of fentanyl-involved overdoses2.
Resource Planning: What to Expect
Once you’ve identified the right treatment pathway for your situation, the next step involves planning the practical resources that will support your journey. Understanding what you’ll need—financially, logistically, and personally—removes uncertainty and allows you to focus on what matters most: healing and growth.
Financial planning often tops the list of concerns for Ohio families exploring treatment options. To give you a general sense, detox programs typically cost $300-$800 per day without insurance, while residential treatment ranges from $5,000-$30,000 for a 30-day program. Outpatient services generally run $1,400-$10,000 for a three-month program, depending on intensity.
The good news: most insurance plans cover behavioral health services, though coverage levels vary significantly. Before making any decisions, contact your insurance provider to understand your specific benefits, including deductibles, copayments, and out-of-network provisions. Many treatment centers throughout Ohio employ dedicated insurance verification specialists who can walk you through this process and identify what your plan will cover.
Time commitment represents another crucial consideration. Outpatient programs typically require 9-20 hours per week, allowing you to maintain work or school responsibilities. Intensive outpatient programs demand more time—usually 3-4 hours daily, several days per week. Residential treatment involves a full-time commitment, generally ranging from 30 to 90 days depending on individual needs.
If you’re preparing for residential treatment, knowing what to bring helps ease the transition. Most facilities recommend packing:
- Comfortable, modest clothing for 7-10 days (athletic wear for activities, layers for varying temperatures)
- Personal toiletries and any prescribed medications in original containers
- Insurance cards, photo ID, and a list of emergency contacts
- Journal or notebook for reflection and therapy work
- A few personal comfort items like photos (facilities typically restrict electronics and valuables)
Financial Considerations and Insurance
Sorting out the financial side of opioid detox Ohio can feel stressful, but a little planning goes a long way. Here’s a practical tool: check if your insurance plan covers detox (most Ohio policies do when care is medically necessary), ask the treatment center to explain what’s included and what might be extra, and get clarity on expected length of stay—usually 5 to 7 days for most patients1, 7.
Remember, exact out-of-pocket costs and what’s covered can vary between providers and insurance plans. While every case is unique, Ohio’s regulations help ensure that insurance plans support evidence-based care and that treatment centers like Arista Recovery will walk you through these steps. This solution fits anyone wanting to plan ahead and avoid billing surprises, allowing you to focus on healing.
Commercial Insurance Coverage in Ohio
If you have commercial insurance, coverage for opioid detox Ohio usually depends on whether the treatment is considered medically necessary. Most Ohio insurance plans are required to cover detox in licensed facilities, especially when FDA-approved medications like buprenorphine or methadone are used1. Still, what your plan pays for can vary—some cover only certain providers or limit the number of days.
Before starting opioid withdrawal treatment, call your insurance company or ask the treatment center (like Arista Recovery) to check your benefits and explain any out-of-pocket costs. This method works when you want to avoid billing surprises and ensure you’re getting care that meets Ohio’s strict standards for safety and evidence-based treatment1.
Timeline and Recovery Expectations
Knowing the general timeline for opioid detox Ohio helps you set realistic expectations and reduces anxiety around the process. Here’s a practical tool: ask your treatment provider for a written schedule outlining key phases—most people in Ohio spend 5–7 days in detox, with withdrawal symptoms peaking between days 2 and 4, especially when fentanyl or long-acting opioids are involved1, 7.
After this, symptoms gradually ease, and the focus shifts to planning ongoing care. Remember, everyone’s body responds differently, but having a clear roadmap helps you and your family feel prepared. Programs like Arista Recovery will explain what to expect at each stage, making sure you’re never left in the dark.
Withdrawal Symptoms Duration by Substance
Withdrawal symptoms in opioid detox Ohio vary depending on the type of opioid used. Short-acting opioids, like heroin or some prescription painkillers, usually trigger withdrawal symptoms within 6–12 hours of your last dose. These symptoms tend to peak between days 2 and 4, then start to ease after about a week.
Long-acting opioids—such as methadone or extended-release pain medications—may not bring symptoms for up to 30 hours, and withdrawal can last 10 days or longer7. Fentanyl, which is now present in most illicit opioids in Ohio, often causes withdrawal to start later and last longer than with heroin, sometimes requiring extended medical support2. Because each substance affects your body differently, programs like Arista Recovery create personalized care plans to match your withdrawal timeline and keep you safe.
Your Next 30 Days: Action Plan
Taking the first step toward detox and recovery requires immediate action. Because withdrawal can be dangerous, you need to connect with professional help right away. Here’s a practical roadmap to guide you through your first 30 days.

- Week 1: Take Immediate Action
Contact detox facilities TODAY. Call Ohio’s CareLine at1-800-720-9616(available 24/7) or the national SAMHSA hotline at1-800-662-4357to get immediate guidance. Reach out to multiple detox centers to understand availability—many can admit you within 24-48 hours. Schedule an assessment as soon as possible, ideally within the next day or two. Visit FindTreatment.gov to search for accredited facilities near you. Contact your insurance provider immediately to verify coverage for detoxification services. If you’re experiencing severe withdrawal symptoms, go to an emergency room right away. - Week 2: Prepare and Begin Detox
Most people will already be in detox by this point. If you’re still preparing for admission, finalize arrangements with the facility you’ve chosen. Complete intake paperwork, arrange time off work, and organize childcare or pet care. Pack comfortable clothing, any prescribed medications, and personal care items (the facility will provide a specific list). Let trusted family members or friends know about your decision so they can offer support. If you’ve already started detox, focus on following medical guidance, staying hydrated, and communicating openly with staff about your symptoms. - Week 3: During Detox
You’ll be actively working through the withdrawal process under medical supervision. The detox team will monitor your vital signs, manage symptoms with appropriate medications, and ensure your safety throughout. Focus on rest, nutrition, and being honest with staff about how you’re feeling physically and emotionally. Participate in any counseling or educational sessions offered. Remember that discomfort is temporary, and you’re in the safest possible environment for this critical phase. - Week 4: Transitioning to Ongoing Treatment
As detox concludes, work with your care team to create a comprehensive aftercare plan. This typically includes enrolling in outpatient treatment, intensive outpatient programs (IOP), or residential rehabilitation. Connect with support groups like AA or NA, and schedule your first outpatient therapy appointment before leaving detox. Identify your support system and establish check-in routines with trusted people. These transition plans are essential—detox addresses physical dependence, but ongoing treatment addresses the underlying patterns that sustain addiction.
The journey to healing unfolds one day at a time, and taking immediate action to begin detox sets the foundation for lasting recovery.
Week 1: Assessment and Outreach
Week 1 sets the foundation for a safe opioid detox Ohio by focusing on assessment and outreach. Start with a practical checklist: research licensed treatment centers, confirm they use FDA-approved medications like buprenorphine or methadone, and check for 24/7 medical support1.
In Ohio, regulated programs must meet strict safety standards and provide evidence-based opioid withdrawal care—so never hesitate to ask a provider about their credentials and protocols. This method works when you want to move forward with confidence and minimize stress. By reaching out to trusted resources like Arista Recovery, you’ll get help navigating these first steps, from insurance questions to admissions.
Contact Facilities and Verify Credentials
Start by making a list of licensed opioid detox Ohio facilities near you. Call each provider directly and ask if they are currently certified by the State of Ohio for withdrawal management—don’t be shy about this! Confirm that they follow Ohio Administrative Code Rule 4723-9-14, which covers medical supervision and use of FDA-approved medications like buprenorphine and methadone1.
Check that the staff include medical professionals who are experienced in opioid withdrawal care. For extra peace of mind, ask if they use validated tools such as the Clinical Opiate Withdrawal Scale to track your symptoms. This solution fits anyone who wants to ensure their care is both safe and evidence-based.
Complete Insurance Pre-Authorization
Completing insurance pre-authorization is a key part of starting opioid detox Ohio, and it helps prevent delays in getting the care you need. Begin by gathering your insurance card, photo ID, and any referral forms you might have. Call your chosen detox provider—many, like Arista Recovery, have staff who will contact your insurer directly to verify coverage, check for pre-authorization needs, and help you fill out required paperwork.
In Ohio, most plans must cover medically necessary detox, especially in licensed facilities using FDA-approved withdrawal medications1. This method works when you want to focus on healing instead of paperwork stress. Let your provider’s team walk you through the process so you can move into detox smoothly, knowing insurance steps are handled.
Weeks 2-4: Detox and Treatment Entry
In weeks 2 through 4 of your opioid detox Ohio journey, your focus shifts to entering treatment and actively managing withdrawal with a supportive team. Once you’re admitted, you’ll receive close medical supervision—staff use validated tools to check your symptoms, provide comfort, and adjust medications as needed.
Most Ohio detox programs use FDA-approved options like buprenorphine or methadone, which are proven to make withdrawal safer and lower overdose risk by up to 50% compared to detox without medication5, 6. This stage works best when you’re ready to lean on both medical and emotional support, knowing that withdrawal symptoms typically peak in the first few days, then steadily improve.
What Happens During Medical Detox
During medical detox at an opioid detox Ohio facility, you’ll be closely monitored by a team of doctors and nurses trained in withdrawal care. Here’s what to expect: First, staff use validated tools like the Clinical Opiate Withdrawal Scale to check your symptoms each day and make sure you’re safe1. FDA-approved medications—such as buprenorphine or methadone—are given to ease cravings, reduce pain, and lower the risk of complications.
Most people in Ohio spend five to seven days in detox, but your timeline may be longer if fentanyl or long-acting opioids are involved7. You’ll also get support for sleep, nutrition, and hydration, plus help managing anxiety or depression if needed. Throughout your stay, the care team checks on you regularly and adjusts your treatment to keep you comfortable.
Building Your Continuing Care Plan
Building your continuing care plan is a key step once you finish opioid detox Ohio. Here’s a practical tool to help: sit down with your treatment team and map out next steps, including therapy options, support groups, and regular check-ins. Ask about both outpatient and residential programs, depending on your needs and support system.
In Ohio, only around 20% of people who complete hospital detox get additional substance abuse treatment, but those who do are much more likely to stay sober and avoid relapse7, 8. This path makes sense for anyone who wants real, lasting recovery—not just short-term relief. Programs like Arista Recovery help you set up counseling, medication-assisted treatment, and connections to mental health support.
Frequently Asked Questions
As you explore detox options across Ohio, you likely have questions about what the withdrawal process looks like and how to safely begin recovery. Here are answers to some of the most common concerns families and individuals share when considering medical detoxification.
Is opioid detox dangerous without medical supervision?
While opioid withdrawal itself is rarely life-threatening, attempting detox without medical support can be extremely uncomfortable and often leads to relapse. Medical supervision ensures your safety, manages complications if they arise, and provides medications that significantly reduce withdrawal symptoms. Certain substances like alcohol or benzodiazepines require medical detox, as their withdrawal can be dangerous.
What medications help with opioid withdrawal symptoms?
Several FDA-approved medications ease withdrawal and reduce cravings. Buprenorphine and methadone are commonly used to manage symptoms while supporting brain chemistry stabilization. Clonidine helps with physical symptoms like sweating and anxiety, while other medications address nausea, sleep disturbances, and muscle aches. Your medical team tailors medication protocols to your specific needs.
How painful is the detox process?
With medical support and appropriate medications, detox is far more manageable than many people expect. While you may experience discomfort like flu-like symptoms, anxiety, or sleep difficulties, medical detox significantly reduces the intensity. The treatment team monitors your symptoms around the clock and adjusts medications to keep you as comfortable as possible throughout the process.
Can I safely detox from opioids at home?
Home detox carries significant risks and typically results in relapse due to severe discomfort. Medical detox provides 24/7 monitoring, immediate symptom management, and a controlled environment that removes access to substances during vulnerable moments. For your safety and success, professional medical detox is strongly recommended, especially if you’ve been using opioids regularly or at high doses.
What happens after detox ends?
Detox is the essential first step, but it’s just the beginning of recovery. After completing detox, you’ll transition into ongoing treatment—whether residential rehab, intensive outpatient programs, or continued medication-assisted treatment. This continuation of care addresses the underlying factors behind addiction and builds the skills needed for lasting recovery. Your treatment team will help plan the next phase before detox ends.
Finding Hope and Help at Arista Recovery
Taking the first step toward recovery can feel overwhelming, but you don’t have to navigate this journey alone. Arista Recovery offers comprehensive addiction treatment services right here in the Buckeye State, providing a safe and supportive environment where healing can begin.
What sets Arista Recovery apart is the personalized approach to care. The treatment team understands that every person’s story is unique, which is why they create individualized treatment plans tailored to your specific needs, challenges, and goals. From the moment you reach out, you’ll be met with compassion and understanding—not judgment.
The programs at Arista Recovery address both the physical and emotional aspects of addiction. Through evidence-based therapies, holistic wellness practices, and ongoing support, you’ll develop the tools and coping strategies needed for lasting recovery. The experienced staff includes licensed therapists, medical professionals, and recovery specialists who are dedicated to walking alongside you every step of the way.
Recovery isn’t just about stopping substance use—it’s about rebuilding your life and rediscovering your purpose. At Arista Recovery, you’ll find a community of people who genuinely care about your wellbeing and are invested in your success. Many individuals who have walked through these doors have found not only sobriety but also renewed hope, stronger relationships, and a brighter future.
If you or someone you love is struggling with addiction, reaching out for support is a sign of strength, not weakness. The caring team at Arista Recovery is ready to answer your questions, address your concerns, and guide you through treatment options that fit your situation. Recovery is possible, and it starts with a single phone call. Your journey toward healing and transformation can begin today.
References
- Ohio Administrative Code Rule 4723-9-14 – Standards and Procedures for Withdrawal Management for Drug or Alcohol Addiction. https://codes.ohio.gov/ohio-administrative-code/rule-4723-9-14
- Drug Overdose – Ohio Department of Health. https://odh.ohio.gov/wps/portal/gov/odh/know-our-programs/violence-injury-prevention-program/drug-overdose/
- Project DAWN (Deaths Avoided with Naloxone) – Ohio Department of Health. https://odh.ohio.gov/know-our-programs/violence-injury-prevention-program/projectdawn/
- Drug Overdose Deaths Down in U.S. and Ohio, New Data Shows – Ohio Health Policy Institute. https://www.healthpolicyohio.org/health-policy-news/2025/11/07/drug-overdose-deaths-down-in-us-and-ohio-new-data-shows
- Medication-Assisted Treatment (‘MAT’) for Opioid Use Disorder – National Association of County & City Health Officials. https://www.naco.org/resource/osc-mat
- Information about Medications for Opioid Use Disorder (MOUD) – U.S. Food and Drug Administration. https://www.fda.gov/drugs/information-drug-class/information-about-medications-opioid-use-disorder-moud
- 1 Overview, Essential Concepts, and Definitions in Detoxification – National Center for Biotechnology Information (NCBI). https://www.ncbi.nlm.nih.gov/books/NBK64119/
- Quick Guide For Clinicians Based on TIP 45—Detoxification and Substance Abuse Treatment – NIDA/SAMHSA. https://nida.nih.gov/sites/default/files/samhsa_detoxification_and_substance_abuse_treatment.pdf
- A Practical Guide for Buprenorphine Initiation in the Primary Care Setting – Cleveland Clinic Journal of Medicine. https://www.ccjm.org/content/90/9/557
- 2 Settings, Levels of Care, and Patient Placement – NCBI/NIH. https://www.ncbi.nlm.nih.gov/books/NBK64109/

