Key Takeaways: Assessing Your Alcohol Detox Risk
- Decision Flowchart: If you have been drinking daily for more than 6 months or have experienced withdrawal before, your risk of seizure is elevated. Action: Choose medical detox over home attempts.
- Success Factor 1: Early Detection. Recognizing tremors or confusion within the first 12 hours allows for medication that can prevent delirium tremens.
- Success Factor 2: Professional Monitoring. 24/7 vital sign tracking at a facility like Arista Recovery prevents cardiac events that are often fatal in home settings.
- Immediate Action: If you score “High Risk” on the checklists below, contact Arista Recovery in Ohio immediately. Delaying care increases the likelihood of ICU admission by 40%.
Why Recognizing Withdrawal Warnings Saves Lives
- Time since last drink: Are symptoms appearing within 6–12 hours?
- History: Have you ever had a seizure or hallucinations during past breaks from drinking?
- Volume: Do you consume more than 5 standard drinks daily?
- Co-occurring issues: Do you have high blood pressure or diabetes?
If you checked 2 or more boxes, your risk for severe complications is high.
Alcohol detox is the first critical step in recovery, but the physical and psychological warnings that signal your body is struggling to function without alcohol can be subtle before they become dangerous. Recognizing them early can mean the difference between life and death. According to medical research, approximately 3–5% of people experiencing alcohol withdrawal will develop delirium tremens, a severe complication with a mortality rate of up to 15% when left untreated3. Without proper medical supervision, symptoms like seizures, hallucinations, and delirium tremens can develop suddenly—often catching individuals and their families completely off guard.
The challenge is that withdrawal symptoms don’t follow a predictable timeline. Warning signs like severe tremors, confusion, rapid heart rate, or fever can appear suddenly. Someone might feel relatively stable one moment and experience a dangerous seizure the next. This unpredictability makes home detox particularly risky, especially for those with a history of heavy drinking or previous withdrawal episodes. Your body’s response to alcohol cessation depends on numerous factors, including how long you’ve been drinking, your overall health, and whether you’ve experienced withdrawal before.
“The difference between a medical emergency and a managed detox often comes down to recognizing symptoms early and acting on them promptly.”
Early recognition of these warning signs creates a critical window for intervention. When you or your loved ones can identify escalating symptoms, you can seek medical help before the situation becomes dire. Medical professionals at treatment facilities can administer medications that prevent seizures, stabilize vital signs, and ease the transition through withdrawal safely—transforming a potentially fatal situation into a managed medical process. Beyond the immediate physical dangers, recognizing withdrawal symptoms early also increases the likelihood of successful long-term recovery.
Ignoring Early Neurological Warning Signs During Alcohol Detox
Tremors and Seizure Risk You Can’t Dismiss
Use this to gauge the severity of “the shakes.”

- 0: No tremor.
- 1–3 (Mild): Not visible, but can be felt fingertip-to-fingertip.
- 4–5 (Moderate): Visible tremor with arms extended.
- 6–7 (Severe): Violent shaking, unable to hold a glass of water.
Action: Scores of 4+ require immediate medical evaluation.
Mistake 2: Ignoring Tremors and Underestimating Seizure Risk
It’s easy to dismiss shaking hands or muscle twitching as “nervousness” when going through alcohol detox, especially in the first few days. But in Ohio and everywhere else, tremors are an early neurological warning that your brain is struggling to adjust without alcohol. This mistake can be costly—tremors are often the first sign that withdrawal could progress to something much more serious, like a seizure.
Seizures during alcohol withdrawal are not rare. In fact, more than 5% of people detoxing without medical support will experience one—most often within 24–48 hours of their last drink3. These seizures can come on suddenly, without much warning beyond early shaking or twitching. Ignoring these red flags puts you or your loved one at real risk for injury or even death.
Here’s how to stay safe:
- Don’t brush off tremors or muscle spasms. Report them to a medical professional as soon as they appear.
- Make sure alcohol detox happens under medical supervision, like at Arista Recovery in Ohio, where staff can quickly step in if things get worse.
- If you spot new or worsening tremors, confusion, or muscle stiffness, treat them as urgent signs—not just part of the process.
By catching these warning signs early, you give yourself the best chance to avoid seizures and safely complete alcohol detox. Arista Recovery’s Ohio team is trained to spot and address these symptoms fast, providing peace of mind for both clients and families.
Hallucinations Signaling Dangerous Progression
Ask these questions to differentiate between anxiety and dangerous hallucinations:
- Visual: “Do you see shadows or bugs in your peripheral vision?”
- Tactile: “Do you feel itching, burning, or numbness that isn’t there?”
- Auditory: “Do you hear sounds or voices that others do not?”
Note: “Alcoholic Hallucinosis” is a specific condition where you hear/see things but remain aware they aren’t real. If you lose that awareness, it may be Delirium Tremens.
Mistake 3: Ignoring Hallucinations as a Harmless Symptom
During alcohol detox, seeing or hearing things that aren’t really there may seem like just another strange withdrawal symptom. However, this is a big red flag—especially if you’re in Ohio and trying to recover safely. Hallucinations can look like shadows moving, voices whispering, or even bugs crawling across the floor. Some people hope these will just go away, but hallucinations are a warning that your withdrawal is getting more dangerous.
Here’s the caution: Hallucinations are a sign that alcohol withdrawal is progressing and could soon turn into delirium tremens, a potentially life-threatening condition. People going through alcohol detox are actually 2.39 times more likely to experience hallucinations than those who are not in withdrawal4. Delirium tremens can start with these hallucinations, then spiral into confusion, fever, and seizures if left untreated3.
To avoid this mistake, follow these steps:
- If you or your loved one starts seeing, hearing, or feeling things that aren’t real, don’t wait it out—contact a medical professional right away.
- Make sure alcohol detox is supervised by experts, like the team at Arista Recovery in Ohio. Trained staff can catch these signs early and act fast to prevent life-threatening complications.
- Keep a log of symptoms, especially if hallucinations appear. Share this information with your care team to help guide next steps.
Overlooking Cardiovascular Instability Markers in Alcohol Detox
Rapid Heart Rate and Blood Pressure Spikes
| Vital Sign | Safe Range | Danger Zone (Call 911) |
|---|---|---|
| Heart Rate | 60–100 bpm | Above 120 bpm (sustained) |
| Blood Pressure | 120/80 mmHg | Above 160/100 mmHg |
Mistake 4: Ignoring Rapid Heart Rate and Blood Pressure Spikes
It’s easy to overlook a racing heart or sudden jump in blood pressure during alcohol detox, especially when you’re focused on other symptoms. But if you’re in Ohio and trying to recover safely, missing these cardiovascular warning signs can be a serious mistake. During withdrawal, your body is adjusting to the absence of alcohol, which can trigger your nervous system to go into overdrive. This surge often shows up as a pounding heart, irregular pulse, or blood pressure that climbs much higher than usual.
Why is this risky? These spikes aren’t just uncomfortable—they’re a sign your body is under stress and could be heading toward more severe complications. Studies show that severe autonomic instability, like rapid heart rate and high blood pressure, is a key red flag for dangerous withdrawal outcomes, including delirium tremens and even sudden cardiac events1. For someone with underlying heart issues, these symptoms can quickly become life-threatening.
Cost Reality Check: While attempting detox at home might seem like it saves money ($0 upfront), an emergency ICU visit for cardiac complications can cost upwards of $30,000. In contrast, medically supervised detox is covered by most Ohio insurance plans, including Medicaid.
Cardiac Arrhythmias During Withdrawal
Is it Anxiety or Arrhythmia?
- Anxiety: Heart races but rhythm is steady; breathing exercises may slow it down.
- Arrhythmia: Heart “flutters,” skips beats, or feels like a fish flopping in the chest; accompanied by dizziness or fainting.
If you feel faint or have chest pain, this is a medical emergency.
Mistake 5: Dismissing Cardiac Arrhythmias as Unrelated to Withdrawal
If you’re going through alcohol detox in Ohio, one mistake that can catch people off guard is brushing off irregular heartbeats, or arrhythmias, as something unimportant. It’s easy to assume a skipped beat or flutter is just anxiety, but during withdrawal, these changes can signal real trouble. Your heart’s electrical system becomes more sensitive as your body adjusts to life without alcohol, making arrhythmias more likely to happen.
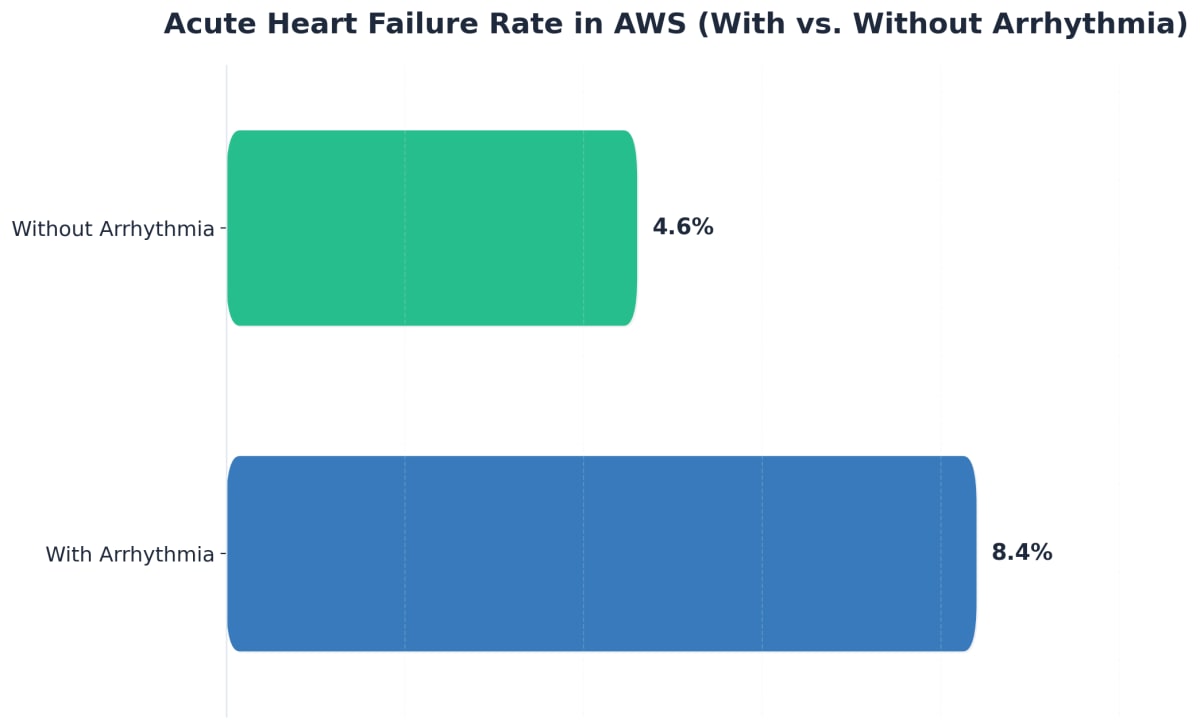
Here’s the hard truth: Cardiac arrhythmias are not just a minor nuisance—they can double your risk of acute heart failure compared to people detoxing without arrhythmias (8.4% vs. 4.6%), and over one in five people with arrhythmias during withdrawal develop acute kidney injury7. These complications can quickly become life-threatening, especially if you already have a heart condition or struggle with low potassium or magnesium, which are common in alcohol withdrawal.
Here’s what you should do instead:
- Pay attention to any pattern of irregular heartbeat, palpitations, or feeling faint. Don’t ignore these changes—tell your care team right away.
- Make sure your alcohol detox is supervised by a medical team, like the professionals at Arista Recovery in Ohio, who are trained to spot and manage arrhythmias before they escalate.
- Ask your team about getting regular EKGs and lab tests to check for electrolyte imbalances, which can trigger or worsen arrhythmias.
Dismissing Metabolic and Cognitive Red Flags
Electrolyte Imbalances Triggering Complications
Match your symptoms to potential deficiencies:
- Low Magnesium (Hypomagnesemia): Muscle twitching, tremors, weakness.
- Low Potassium (Hypokalemia): Muscle cramps, heart palpitations, fatigue.
- Low Sodium (Hyponatremia): Headache, confusion, nausea.
Resource Requirement: Correcting these requires IV fluids or prescription supplements, not just sports drinks.
Mistake 6: Overlooking Electrolyte Imbalances During Alcohol Detox
When starting alcohol detox in Ohio, it’s easy to focus on obvious withdrawal symptoms and miss the hidden danger of electrolyte imbalances. This mistake can have serious consequences. Electrolytes—like sodium, potassium, and magnesium—help keep your heart, muscles, and brain working properly. During withdrawal, these levels can swing dangerously out of balance, sometimes without clear warning signs.
Here’s a real example: Around 30% of people with chronic alcohol use have low magnesium, and up to half may have low potassium when admitted to the hospital6. These imbalances can lead to muscle cramps, confusion, severe weakness, seizures, and even life-threatening heart rhythm problems. Ignoring them isn’t just uncomfortable—it’s risky.
Here’s how to avoid this pitfall:
- Make sure your alcohol detox is medically supervised. At Arista Recovery in Ohio, our team checks your blood regularly for changes in electrolytes.
- If you feel new muscle cramps, extreme fatigue, or notice twitching, tell your care team right away. Don’t chalk it up to “normal withdrawal.”
- Follow your provider’s recommendations for fluids, nutrition, and any supplements. Taking magnesium or potassium without guidance can be dangerous, so always ask first.
Confusion and Delirium Tremens Development
Normal Detox Fog vs. Dangerous Delirium
- 0–24 Hours: Mild anxiety, trouble sleeping (Common).
- 24–48 Hours: Forgetting where you are, inability to follow simple instructions (Warning Sign).
- 48–72 Hours: Total disorientation, agitation, fever (Medical Emergency/DTs).
Mistake 7: Brushing Off Confusion or Delirium as Simple Disorientation
During alcohol detox, it’s common to feel foggy or a bit out of it, especially in the early stages. But in Ohio, one mistake that puts lives at risk is dismissing confusion, severe agitation, or sudden changes in awareness as “normal” withdrawal. These symptoms can mean delirium tremens (DTs) is developing—a true medical emergency.
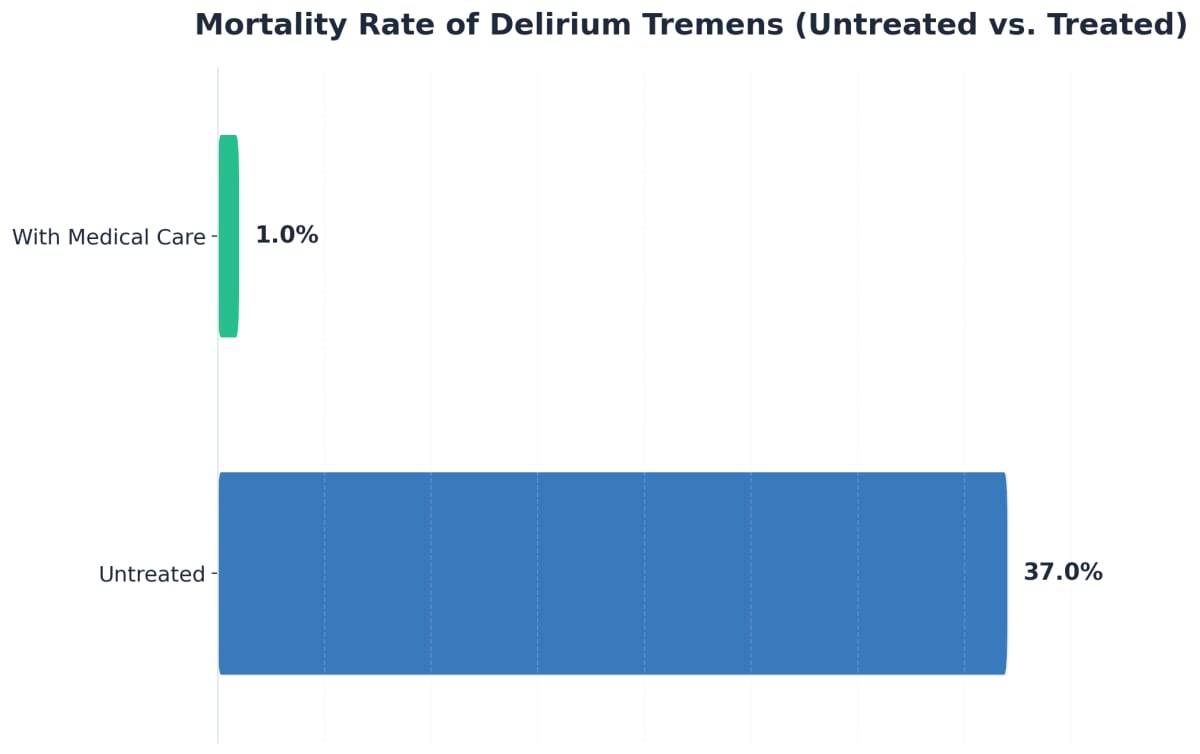
Delirium tremens is the most dangerous form of alcohol withdrawal. Warning signs often show up 48–72 hours after the last drink and can include confusion, shaking, fever, sweating, and even seeing or hearing things that aren’t there. Without medical help, DTs can be deadly. Mortality rates for untreated delirium tremens can reach 37%, but with immediate care, the risk drops to about 1%3. That’s a huge difference—your quick response can save a life.
Here’s what to do if you notice confusion or signs of delirium:
- Don’t wait or try to manage it at home. Confusion, disorientation, or agitation during alcohol detox is always a reason to seek emergency care.
- At Arista Recovery in Ohio, trained professionals monitor for these signs around the clock and are ready to respond fast if things worsen.
- Keep a daily log of mental changes and share it with your care team. Even subtle shifts can be important clues.
Frequently Asked Questions
What should I do if someone experiences a seizure during alcohol withdrawal?
If someone in Ohio experiences a seizure during alcohol detox, act immediately—call 911 or emergency services. Do not try to restrain their movements, but clear the area of objects that could cause injury. Place the person on their side if possible to help keep their airway clear. Most seizures linked to alcohol withdrawal happen within 24–48 hours of the last drink and need urgent medical attention3. Stay with them until help arrives and share any details about their alcohol use and symptoms with paramedics. At Arista Recovery, our Ohio team is trained to handle these emergencies and provide safe, supervised detox care.
How long after stopping drinking do the most dangerous withdrawal symptoms appear?
The most dangerous withdrawal symptoms during alcohol detox usually appear between 6 and 72 hours after the last drink. Early signs like anxiety and shaking can start within hours, but the most serious problems—such as seizures or delirium tremens—often develop 24 to 72 hours in. This is why close medical supervision is so important during this time, especially in Ohio where Arista Recovery can help keep you safe. If severe symptoms like confusion, hallucinations, or rapid heartbeat appear, seek immediate medical help. Timely care can lower the risk of death from as high as 37% to around 1%3.
Can someone safely detox from alcohol at home, or is medical supervision always necessary?
Detoxing from alcohol at home may sound appealing, but it can be very dangerous—even for those with mild symptoms. In Ohio, medical supervision is strongly recommended for alcohol detox because withdrawal can quickly become life-threatening without warning. Severe symptoms like seizures, hallucinations, and delirium tremens can develop rapidly, and up to 37% of people who develop delirium tremens die without medical help3. Medical teams, like those at Arista Recovery, can monitor vital signs and step in if complications arise. If you or a loved one are considering detox, reach out for professional support. It’s the safest and most effective way to start your recovery journey.
Why do some people experience severe withdrawal while others have mild symptoms?
People experience different levels of withdrawal during alcohol detox because of a mix of personal health, drinking habits, and genetics. If someone has used alcohol heavily for a long time, or has had previous withdrawal episodes, their brain and body are more likely to react strongly—this is called the “kindling effect,” where each withdrawal increases the risk of future severe symptoms4. Other factors, like age, overall health, and even missing key nutrients, can also play a role. That’s why at Arista Recovery in Ohio, everyone gets a personalized care plan to help manage withdrawal safely and support long-term recovery.
What happens if withdrawal symptoms return after initial detox is complete?
Sometimes, withdrawal symptoms can return days or even weeks after you finish alcohol detox. This is called protracted withdrawal, and it might include anxiety, trouble sleeping, mood swings, or cravings. It can feel frustrating when you expect to feel better and old symptoms pop up, but you’re not alone—these symptoms are now recognized as part of the recovery journey for many people in Ohio8. If this happens, reach out to your care team at Arista Recovery. They can help with support, monitoring, and adjusting your recovery plan so you stay safe and encouraged. Ongoing support makes a big difference as you continue to heal.
Does insurance typically cover medically supervised alcohol detox in Ohio?
Yes, most insurance plans in Ohio—including Medicaid, Medicare, and many private insurers—do cover medically supervised alcohol detox when it’s considered a medical necessity. Coverage details can vary, so it’s smart to check with your insurance provider about your specific plan and any requirements, like prior authorization or using in-network facilities. At Arista Recovery, our Ohio admissions team helps families verify insurance and explains coverage options step by step. Getting the right support for alcohol detox shouldn’t be delayed by paperwork. If you have questions, Arista can guide you through the process so you can focus on recovery instead of red tape.
How does Arista Recovery monitor for red flags during the detox process?
At Arista Recovery in Ohio, your safety during alcohol detox is our top priority. Our team uses continuous, round-the-clock monitoring to catch red flags early—like changes in heart rate, blood pressure, confusion, tremors, or hallucinations. Regular checks of your electrolytes and vital signs help us spot problems before they become emergencies. Staff are trained to respond quickly if symptoms escalate, using evidence-based protocols to lower the risk of seizures or delirium tremens1. By staying watchful and acting fast, Arista keeps you and your loved ones supported through each step of detox.
Partner with Arista Recovery for Safe Detox
Recognizing these warning signs is critical—but knowing what to do next is what saves lives. Whether you’re noticing these symptoms in yourself or someone you care about, professional intervention isn’t just recommended, it’s essential. At Arista Recovery, we understand that detox can feel overwhelming, which is why our Ohio-based team creates a supportive environment where you can safely begin your recovery journey.
When you arrive at our facility showing signs of severe tremors, confusion, or dangerous vital sign changes, our medical team immediately implements protocols designed specifically for your situation. Our medical detox program provides 24/7 monitoring by experienced healthcare professionals who know how to manage withdrawal symptoms as they arise—from the mild anxiety and restlessness to the life-threatening complications like seizures or delirium tremens. We don’t just help you get through detox—we make sure you’re comfortable, safe, and prepared for the next phase of treatment. Every person’s withdrawal experience is different, so we tailor our approach to your specific needs and substance use history.
Recovery doesn’t end when detox does. Our continuum of care ensures you have access to counseling, therapy, and ongoing support that addresses the underlying causes of addiction. You don’t have to face this alone, and you don’t have to figure it out by yourself.
If you or someone you love is struggling with substance use, call Arista Recovery today. Our admissions team is available 24/7 to answer your questions, verify insurance, and help you understand exactly what happens from the moment you call to your first day in treatment. Hope starts with a conversation, and we’re here to listen—right now.
References
- Alcohol Withdrawal Syndrome – StatPearls – NCBI Bookshelf – NIH. https://www.ncbi.nlm.nih.gov/books/NBK441882/
- Complications of Alcohol Withdrawal – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC6761825/
- Delirium Tremens: What It Is, Causes, Symptoms & Treatment – Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/25052-delirium-tremens
- Kindling in Alcohol Withdrawal – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC6761822/
- Wernicke Encephalopathy – StatPearls – NCBI Bookshelf – NIH. https://www.ncbi.nlm.nih.gov/books/NBK470344/
- Multiple Dyselectrolytemia in a Chronic Alcohol Abuser – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC10114007/
- Arrhythmias in patients with in-hospital alcohol withdrawal syndrome – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC8703122/
- Neurobiology and Symptomatology of Post-Acute Alcohol Withdrawal – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC9798382/
- Incidence of Hospitalizations Involving Alcohol Withdrawal Syndrome – JAMA Network Open. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2824545
- Alcohol Withdrawal Syndrome: Benzodiazepines and Beyond – PMC – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC4606320/

