Key Takeaways: Your Decision Guide
- Assess Your Risk: If you have a history of seizures, heart issues, or heavy daily drinking, medical supervision is not optional—it is a safety requirement.
- The Protocol Advantage: An evidence-based alcohol detox protocol uses symptom-triggered medication to keep you comfortable and prevent life-threatening complications.
- Immediate Action: If you are experiencing tremors or confusion, contact a medical professional or Arista Recovery immediately to begin a safe assessment.
Why an Alcohol Detox Protocol Makes Detox Safer
Understanding Alcohol Withdrawal Severity
Grasping how severe alcohol withdrawal can become is key to understanding why medical supervision is often needed. Not everyone will experience withdrawal the same way, but the risks are real. About half of people in Ohio who stop or sharply cut back on drinking after regular, heavy use will notice withdrawal symptoms. These can range from mild shakes and anxiety to dangerous complications like seizures or delirium tremens (DTs), which is a medical emergency.4
To help you spot your personal risk level, review this quick assessment checklist:
- Have you ever needed a drink in the morning to steady yourself?
- Have you had withdrawal symptoms before?
- Are you over 40, or do you have other health problems?
- Have you had seizures or hallucinations in the past when stopping alcohol?
If you answer “yes” to any of these, your risk of severe withdrawal is higher. Symptoms usually start within 6–24 hours of the last drink and can get worse quickly. Without a proper alcohol detox protocol, these symptoms can become life-threatening.
“Medical care is crucial—a treated episode of severe withdrawal has a 95% survival rate, but without treatment, the risk of dying from DTs climbs to 15%.”5
Arista Recovery understands how overwhelming this process can feel. With the right help, you don’t have to face these risks alone. Next, let’s break down when professional detox becomes essential and what signs to watch for.
When Professional Detox Becomes Essential
Knowing when to seek a professional alcohol detox protocol can save lives, especially in Ohio where access to specialized care is vital. Here’s a simple decision guide to help you recognize when medical detox is the safest choice.
Checklist: Is Professional Detox Needed?
- You’ve experienced seizures, hallucinations, or delirium tremens (DTs) before.
- You have serious health conditions (like heart, liver, or kidney problems).
- You’re pregnant or over age 60.
- You’ve tried to quit before and withdrawal symptoms were severe or unmanageable.
- There’s no trustworthy adult to monitor your symptoms at home.
This approach is ideal if you or your loved one answer yes to any of these items. In these situations, at-home detox is not just risky—it can quickly become life-threatening. Opting for a professional alcohol detox protocol includes round-the-clock monitoring, rapid medication adjustments, and immediate intervention if complications arise.4
For Ohio families, Arista Recovery offers safe, welcoming support—so you don’t have to face this alone. Our team is trained to spot early warning signs and act fast, giving you the best chance for a safe recovery. Next up, let’s explore which treatments and tools are used in evidence-based detox care.
Core Components of an Evidence-Based Alcohol Detox Protocol
Benzodiazepine Therapy as First-Line Treatment
Benzodiazepine therapy is the foundation of a safe alcohol detox protocol, especially for people facing moderate to severe withdrawal. Here’s a simple decision guide you can use with your care team in Ohio:
Quick Guide: Is Benzodiazepine Therapy Needed?
- Are you experiencing tremors, anxiety, or high blood pressure after stopping alcohol?
- Have you had seizures or delirium tremens (DTs) before?
- Do you have a history of heavy or long-term drinking?
This solution fits most individuals with symptoms or risk factors for serious withdrawal. Benzodiazepines—like diazepam, chlordiazepoxide, or lorazepam—work by calming the nervous system, lowering the risk of seizures and dangerous complications. In fact, they’re proven to be the most effective medicines for reducing withdrawal severity and preventing life-threatening problems like DTs.1, 2, 3
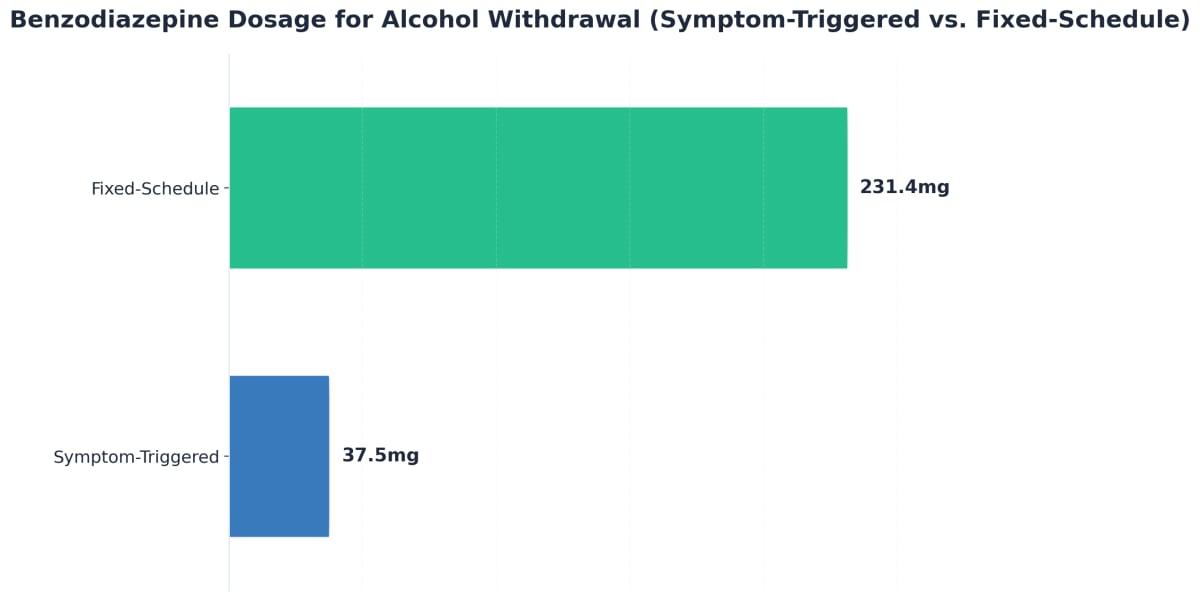
Protocols typically use a short course (3–7 days), with medication amounts adjusted based on your symptoms. Symptom-triggered dosing, where medication is only given when withdrawal signs appear, can cut down on the total medicine needed without sacrificing safety.10 This approach works best when you’re in a setting with trained staff who check your symptoms regularly—like Arista Recovery or other licensed Ohio detox centers.
Benzodiazepine therapy does require careful monitoring. Some patients—especially those with liver problems—may need a different medication or a slower taper. Your care team will choose the right plan based on your health needs. Arista Recovery’s Ohio-based team is well-trained in these evidence-based protocols, so you or your loved one can feel safe and supported through detox.
Symptom Monitoring and Assessment Tools
Effective symptom monitoring is the backbone of a safe alcohol detox protocol. In Ohio, most treatment centers—including Arista Recovery—use tools like the CIWA-Ar (Clinical Institute Withdrawal Assessment for Alcohol, Revised) to keep a close eye on withdrawal symptoms. This checklist asks about things you or your loved one may feel (such as nausea, anxiety, or sweats) and includes what nurses and doctors can see, like shaking or changes in blood pressure.
Here’s a practical tool to help you understand how monitoring works:
- Nausea or vomiting
- Tremors (shaking hands)
- Sweating
- Anxiety or agitation
- Confusion or trouble thinking clearly
- Hallucinations (seeing or hearing things that aren’t there)
- Seizures
Each item is scored, and the total guides how much medication you might need. This approach allows Ohio care teams to adjust treatment quickly and safely. Symptom-triggered monitoring—rather than a fixed schedule—can cut down on the amount of medication you need and shorten your stay, all without making you less safe.10
It’s important to know that some people, like those who are confused or have trouble communicating, may need different tools. Objective assessment scales—where nurses rely more on observation—are sometimes a better fit.6 Arista Recovery’s staff in Ohio are trained to use these tools and respond fast if symptoms change, which helps prevent dangerous complications.
Essential Supportive Care During Withdrawal
Thiamine and Nutritional Supplementation
Making sure your body gets enough vitamins—especially thiamine (vitamin B1)—is a vital part of any safe alcohol detox protocol. Thiamine helps your brain and nerves work properly, but heavy drinking can block your body from absorbing it. In Ohio, up to 80% of people struggling with alcohol addiction develop thiamine deficiency, putting them at risk for serious conditions like Wernicke’s encephalopathy and Korsakoff’s syndrome, which can cause memory loss and confusion.7
A practical tool used by detox centers, including Arista Recovery, is a nutrition assessment checklist. This helps your care team quickly spot signs of poor nutrition or vitamin shortages, such as weight loss, confusion, or trouble walking. If these are present, medical teams act fast to give thiamine—often by injection or IV, since pills may not work as well for people in withdrawal. Early thiamine treatment can prevent life-changing complications.
This route is best for anyone entering an alcohol detox protocol, no matter their age or health history. Alongside thiamine, Ohio detox teams also monitor for other shortages, like folate and vitamin B12, and address them as needed. Arista Recovery’s commitment to evidence-based care means you or your loved one gets the right nutritional support from day one.
Fluid Management and Electrolyte Balance
Keeping your body hydrated and your minerals balanced is a core part of any safe alcohol detox protocol. When you stop drinking, your body can lose fluids quickly through sweating, vomiting, or diarrhea—especially during withdrawal. These losses can lead to dehydration and disturb levels of electrolytes like sodium, potassium, and magnesium.
If these minerals drop too low or rise too high, you may face muscle cramps, irregular heartbeats, or even seizures. In Ohio detox centers, including Arista Recovery, trained staff check your fluid and electrolyte status often.
Here’s a simple checklist used in medical settings:
- Watch for signs of dehydration: dry mouth, rapid heartbeat, dizziness
- Monitor urine color and amount
- Test blood for sodium, potassium, and magnesium levels
- Replace fluids by mouth or IV as needed
- Correct any abnormal electrolyte levels promptly
This approach works best when managed by medical professionals—fluid overload or rapid correction can be risky if not done carefully.8 Proper management can prevent complications that make withdrawal much harder to handle. Arista Recovery’s Ohio team uses up-to-date protocols to keep you safe, comfortable, and on track toward recovery.
Preventing Life-Threatening Complications
Given the serious health risks we’ve discussed, understanding how professional detox prevents life-threatening complications becomes essential to your decision-making process. If you’re considering detox for yourself or helping a family member through this journey, you need to know exactly how medical supervision protects against the most dangerous outcomes.
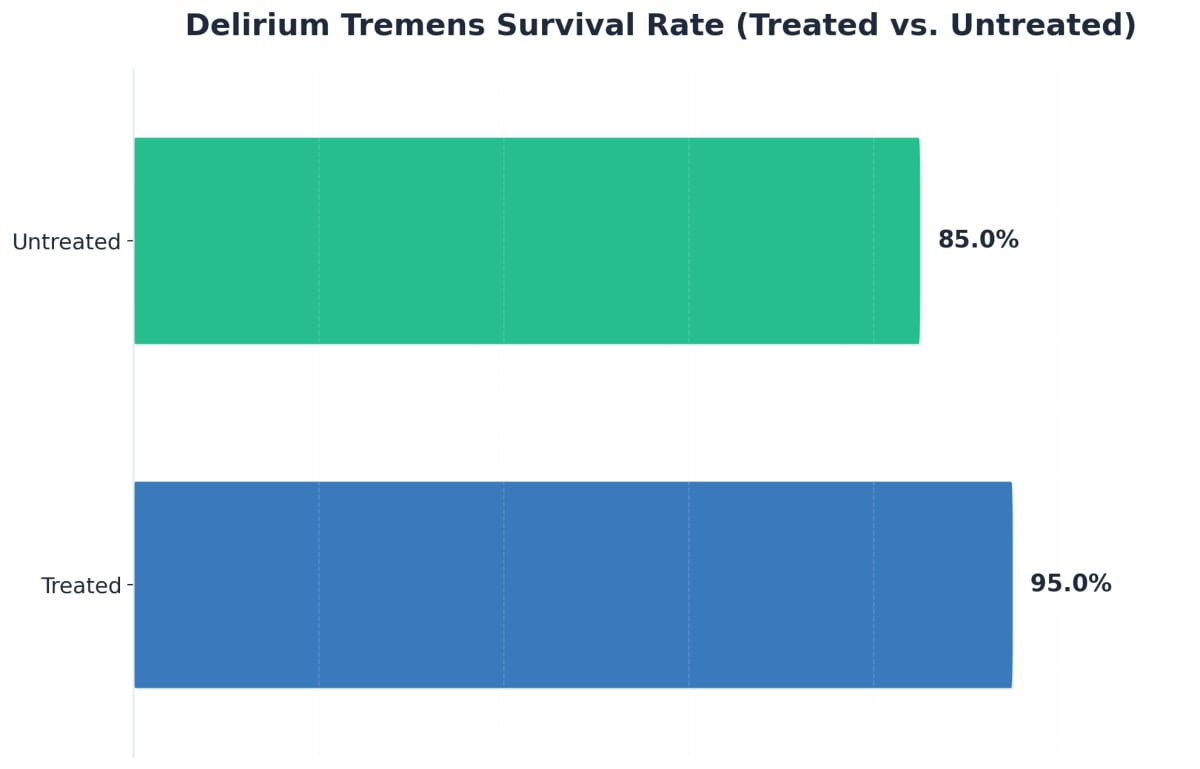
Withdrawal from certain substances can be deadly without proper medical intervention. Alcohol and benzodiazepine withdrawal, in particular, can cause seizures, cardiac complications, and delirium tremens—a severe condition that can be fatal in up to 15% of untreated cases. In a medical detox setting, healthcare professionals monitor your vital signs around the clock and can intervene immediately if dangerous symptoms develop. This level of care simply isn’t possible at home, no matter how dedicated your family members may be.
Overdose risk actually increases during certain stages of recovery. When you attempt to detox on your own and relapse, your tolerance has often decreased significantly. Using the same amount you once could handle may now be lethal. Medical detox programs provide a safe, controlled environment where this risk is eliminated during your critical early days of recovery. Staff members are trained in overdose prevention and reversal, and facilities maintain emergency protocols that can save your life within seconds.
Beyond the immediate risks of withdrawal and overdose, untreated addiction leads to cascading health problems that worsen over time. Liver disease, heart damage, infectious diseases, and malnutrition are common complications that develop alongside substance use disorders. During medical detox, healthcare providers can identify your underlying conditions early and begin addressing them. This comprehensive approach treats you as a whole person, not just your addiction symptoms.
Mental health crises often accompany detox, and these psychological emergencies can be just as dangerous as physical ones. Severe depression, anxiety, and suicidal thoughts frequently surface when substances are removed. Having mental health professionals available 24/7 means your crises receive immediate attention. Medication management, therapeutic support, and crisis intervention all work together to keep you safe during your most vulnerable moments.
The combination of medical monitoring, emergency preparedness, and comprehensive health assessment creates a safety net that dramatically reduces your risk of life-threatening complications. Accredited detox facilities follow evidence-based protocols designed specifically to prevent the worst outcomes. This isn’t about creating fear—it’s about acknowledging reality and choosing the path that offers you the greatest protection. Professional detox transforms what could be a dangerous medical emergency into a managed, supported process where your healing can truly begin.
Frequently Asked Questions
How much does medical detox cost in Ohio, and will my insurance cover it?
Medical detox costs in Ohio can vary based on your insurance plan and the specific alcohol detox protocol you need. Many private insurance plans, Medicaid, and Medicare often cover part or all of the cost of detox if it’s medically necessary. Coverage usually includes the assessment, medications, and 24/7 care provided by trained staff. However, exact out-of-pocket costs depend on your deductible, copays, and whether the detox center is in-network. It’s a good idea to contact your insurance company or speak with Arista Recovery’s Ohio team—they can help you check your benefits and explain what’s covered before you start treatment 4.
Can I safely detox from alcohol at home, or do I need to go to a facility?
Detoxing from alcohol at home can be risky, especially if you have a history of seizures, hallucinations, heart problems, or have experienced severe withdrawal before. Even if symptoms seem mild at first, they can become life-threatening quickly—about 15% of people with untreated delirium tremens do not survive, but medical care raises survival to 95% 5. An alcohol detox protocol in a medical facility includes round-the-clock care and fast response if complications arise. For most people in Ohio, professional detox at a place like Arista Recovery is the safest path to recovery and gives families peace of mind.
How long does alcohol detox typically take from start to finish?
The length of alcohol detox depends on your health, drinking history, and which alcohol detox protocol is used. Most people in Ohio will complete the main part of withdrawal in 3 to 7 days, with symptoms often starting within 6–24 hours after the last drink. Mild symptoms may fade after a few days, but some people notice fatigue or sleep changes for a bit longer. Medical teams, like those at Arista Recovery, check your progress each day and adjust care as needed, so your experience is as safe and comfortable as possible 4.
What happens after detox is complete—do I need additional treatment?
After you complete detox, your recovery journey isn’t over—detox is just the first step. Most people in Ohio benefit from ongoing support, like counseling, group therapy, or medication to help prevent relapse. These treatments help you build healthy routines and address any underlying issues connected to alcohol use. According to medical guidelines, starting ongoing treatment right after finishing an alcohol detox protocol lowers the risk of returning to drinking and boosts your chances of long-term success 4. Arista Recovery can help you create a plan for the next stage, keeping you and your family involved and supported.
Will I be comfortable during detox, or will withdrawal symptoms be unbearable?
Most people are surprised to learn that a well-designed alcohol detox protocol actually aims to keep you as comfortable as possible. Medical teams in Ohio, like those at Arista Recovery, use symptom-triggered medication and supportive care to ease symptoms such as anxiety, shakes, trouble sleeping, or nausea. With 24/7 monitoring and quick response, severe discomfort is much less common than you might expect 10. While some symptoms can’t be avoided entirely, the right protocol makes withdrawal safer and more manageable. You’ll have caring staff by your side, helping you through each step so you don’t have to face it alone.
How do I choose between different detox facilities in Ohio?
When choosing between detox facilities in Ohio, start by checking if the center uses an evidence-based alcohol detox protocol with medical supervision and symptom tracking tools like CIWA-Ar or other objective assessment scales 46. Ask about 24/7 medical staffing, access to emergency care, and whether thiamine and nutrition support are part of their routine. This path makes sense for those wanting the safest, most reliable care. Also, look for programs like Arista Recovery that welcome family involvement and offer personalized aftercare planning. Touring the facility or calling their team can help you get a feel for their approach and build trust.
Can my family visit me or stay involved during the detox process?
Yes, family involvement is encouraged during an alcohol detox protocol at most Ohio treatment centers, including Arista Recovery. While visitation rules can vary, most facilities welcome family visits during set hours and often offer support groups or family counseling sessions. Staying connected helps you feel supported and allows loved ones to ask questions, learn about the process, and plan for the next steps together. This approach works well for people who benefit from encouragement and want to strengthen family bonds during recovery. Arista Recovery believes including families leads to better outcomes and a more hopeful transition after detox 4.
Building Your Path to Lasting Recovery
Once you’re safely through the acute dangers of detox, the real work of recovery begins. While medical supervision addresses the immediate physical crisis, building lasting sobriety requires addressing why you turned to substances in the first place and developing concrete skills to navigate life without them. This transition from crisis management to long-term healing marks a critical turning point in your recovery.

In Ohio, comprehensive recovery programs typically include individual therapy to explore personal triggers and patterns, group counseling to connect with others facing similar challenges, and family therapy to rebuild relationships damaged by addiction. Evidence-based approaches like cognitive behavioral therapy help you develop healthier coping mechanisms, while holistic treatments address your overall well-being.
| Timeline | Key Focus | Typical Setting |
|---|---|---|
| First 30 Days | Identify high-risk situations, develop emergency response plans, process underlying issues. | Residential / Inpatient |
| By 60 Days | Practice new skills in challenging situations, transition planning. | Residential to Outpatient |
| At 90 Days | Building confidence, solidifying neural pathways for healthy choices. | Outpatient / Sober Living |
The transition from detox to ongoing treatment determines long-term success. Residential programs provide 24/7 structure and intensive support during those vulnerable early weeks, while outpatient care allows you to practice new skills in real-world situations. Support groups, sober living environments, and continued counseling create multiple safety nets during moments when cravings hit hardest—because they will hit, and having a plan makes all the difference.
Recovery isn’t about perfection—it’s about building momentum through small, consistent choices. With professional guidance, peer support, and your own commitment to healing, you can create a life where sobriety isn’t just about what you’ve given up, but what you’ve gained.
References
- Alcohol Withdrawal in Hospitalized Patients – NCBI Bookshelf – NIH. https://www.ncbi.nlm.nih.gov/books/NBK604324/
- Clinical management of alcohol withdrawal: A systematic review. https://pmc.ncbi.nlm.nih.gov/articles/PMC4085800/
- Management of alcohol withdrawal – WHO Guidelines. https://www.who.int/teams/mental-health-and-substance-use/treatment-care/mental-health-gap-action-programme/evidence-centre/alcohol-use-disorders/management-of-alcohol-withdrawal
- Alcohol Withdrawal Syndrome: Outpatient Management. https://www.aafp.org/pubs/afp/issues/2021/0900/p253.html
- Delirium Tremens: What It Is, Causes, Symptoms & Treatment. https://my.clevelandclinic.org/health/diseases/25052-delirium-tremens
- Clinical Institute Withdrawal Assessment for Alcohol–Revised might not be applicable in all patients. https://pmc.ncbi.nlm.nih.gov/articles/PMC5597013/
- Alcohol related thiamine deficiency. https://adf.org.au/insights/alcohol-related-thiamine-deficiency/
- Alcohol withdrawal syndrome in medical patients. https://www.ccjm.org/content/83/1/67
- Alcohol Withdrawal Syndrome: Benzodiazepines and Beyond. https://pmc.ncbi.nlm.nih.gov/articles/PMC4606320/
- Symptom-Triggered vs Fixed-Schedule Doses of Benzodiazepine for Alcohol Withdrawal: A Randomized Trial. https://jamanetwork.com/journals/jamainternalmedicine/fullarticle/211434

