Key Takeaways
- Suboxone is a medication combining buprenorphine and naloxone designed to reduce opioid cravings and withdrawal symptoms safely.
- The treatment significantly lowers overdose risk, offers a “ceiling effect” for safety, and can be prescribed in outpatient settings.
- Suboxone treatment in Hilliard, OH, is most relevant for individuals and families in the region seeking a flexible, evidence-based path to recovery.
What Is Suboxone Treatment in Hilliard, OH?
The Science Behind Buprenorphine
Buprenorphine is the primary active ingredient in Suboxone treatment in Hilliard, OH. To understand how it works, think of it like a key that fits perfectly into a lock—except this key only opens the door halfway. Buprenorphine attaches to the same receptors in your brain that opioids do, but it does not produce the same intense “high.” Instead, it effectively quiets cravings and manages withdrawal symptoms, allowing you to feel normal and function in your daily life.
A critical safety feature of buprenorphine is the “ceiling effect.” Imagine filling a cup with water; once the cup is full, adding more water simply causes it to spill over without increasing the volume inside. Similarly, taking more buprenorphine beyond a certain point does not increase its effect. This mechanism makes it significantly harder to misuse or overdose on compared to traditional opioids, a vital consideration given the high rates of opioid challenges in Ohio.4
Doctors in Ohio value buprenorphine because it can be prescribed in standard medical offices. This accessibility allows families to seek care in a familiar, comfortable environment. At Arista, we believe that understanding the mechanics of your medication can demystify the process, making the first steps toward recovery feel less daunting.
Why Naloxone Is Added to the Formula
You might wonder why Suboxone is a combination of two medicines: buprenorphine and naloxone. Naloxone acts as a safeguard or a “safety switch” for your brain. If you were to use a lock that only opens for a specific key, naloxone is the alarm system that triggers if someone tries to force the lock open incorrectly.
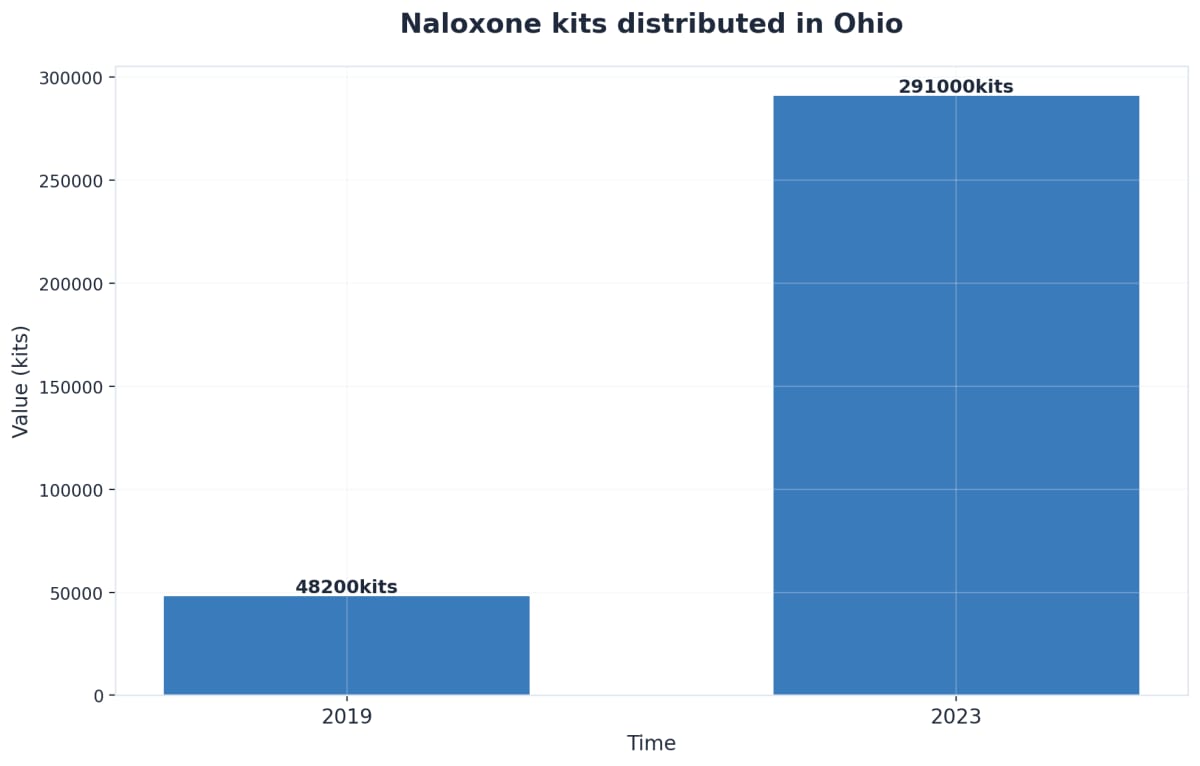
When Suboxone is taken as prescribed—dissolved under the tongue—the naloxone remains dormant and has little to no effect. However, if the medication is misused via injection, the naloxone activates immediately to block opioid effects and precipitate withdrawal. This deterrent helps prevent abuse and protects individuals from accidental overdose.9
With fentanyl present in a significant percentage of overdose deaths in the state, the addition of naloxone makes treatment safer for everyone involved.3
At Arista, we want you to feel confident that this formula is engineered with your safety as the priority, allowing you to focus on healing without unnecessary worry.
Proven Benefits of Medication-Assisted Treatment
Overdose Risk Reduction Statistics
One of the most compelling reasons to consider Suboxone is its ability to drastically reduce the risk of overdose. If recovery were a walk on an icy sidewalk, Suboxone would be the boots providing traction and stability. Clinical studies highlight the effectiveness of this approach:
| Treatment Duration | Reduction in Overdose Risk |
|---|---|
| First 3 Months | 76% lower risk compared to no medication1 |
| 12 Months | 59% lower risk compared to no medication1 |
These statistics are particularly relevant in Ohio, where overdose rates have historically been high. In 2020, fentanyl was identified in 94% of opioid overdose deaths in the state.3 Utilizing proven treatments like Suboxone provides families with a tangible tool to protect their loved ones.
Why Medication Outperforms Abstinence-Only
Attempting to recover through abstinence-only methods can be compared to climbing a steep hill without any gear. While the intention is good, the lack of support increases the risk of slipping. Suboxone provides the necessary tools to make the climb manageable and safe.
Research indicates that abstinence-only treatment can inadvertently increase danger. When a person stops using opioids completely, their body loses its tolerance. If a relapse occurs, even a small dose can be fatal. Non-medication treatments have been associated with a risk of fatal overdose that is over 77% higher, whereas Suboxone and similar medications reduce that risk by approximately one-third.2
Medication-assisted treatment (MAT) is not “trading one addiction for another.” It is a medical intervention that stabilizes brain chemistry, controls cravings, and allows individuals to engage fully in therapy and life rebuilding. At Arista, we emphasize that choosing MAT is a decision for safety and long-term success.
The Three Phases of Suboxone Treatment
Induction: Starting Treatment Safely
The induction phase is the initial step of your recovery journey. Think of this as learning to ride a bike with training wheels; it requires care and guidance to start safely. During induction, the Arista care team helps you transition from opioids to Suboxone. Crucially, you must be in a state of mild withdrawal before taking the first dose to avoid precipitating worse symptoms.

Your provider will monitor you closely during this phase:
- Assessment: Checking your withdrawal levels and vital signs.
- Dosing: Administering the first dose and observing the effects.
- Adjustment: Tuning the dosage like a guitar string until it perfectly alleviates symptoms without causing sedation.9
This process is typically outpatient, allowing you to return to the comfort of your home and family support system each day. In Ohio, starting treatment this way ensures safety while maintaining your daily connections.4
Stabilization and Long-Term Maintenance
Following induction, treatment moves into stabilization. This phase is about finding your balance. Your care team at Arista will work with you to fine-tune your medication until you feel “normal”—free from cravings and withdrawal symptoms. This period usually lasts a few weeks and involves regular check-ins to ensure the dosage remains effective.
Once you are stable, you enter the maintenance phase. This is akin to riding on a smooth, open path where you can focus on rebuilding your life, returning to work, and reconnecting with loved ones. Research supports staying on medication for at least six months to improve long-term health outcomes.1 Many Ohio residents opt for extended maintenance to provide a robust shield against relapse in an environment where overdose risks persist.3
Accessing Suboxone Treatment in Hilliard, OH
Ohio’s Expanding Treatment Infrastructure
Ohio has made significant progress in expanding the network of care available to residents. The state’s treatment system has grown like a network of bridges, connecting people from isolation to support. Between 2019 and 2024, the number of opioid treatment providers in Ohio increased from 35 to 125—a 250% jump.10
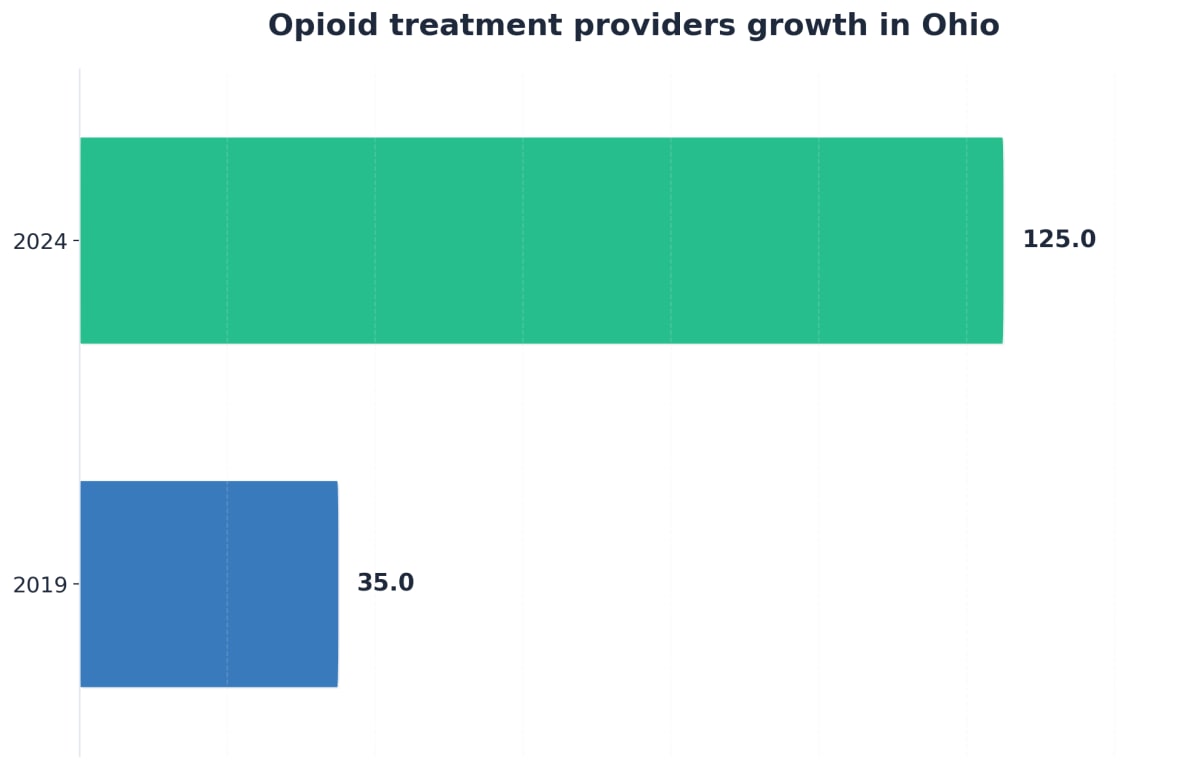
This expansion means shorter wait times and more clinics closer to home. Additionally, the adoption of telemedicine has revolutionized access, allowing prescriptions and counseling to occur online. This is particularly beneficial for those with tight work schedules or transportation challenges.6 Arista is proud to be part of this growing infrastructure, offering trusted local support to ensure no one has to navigate recovery alone.
Insurance Coverage and Cost Considerations
Navigating insurance can be complex, but understanding your coverage is a vital part of the process. In Ohio, Medicaid and most private insurance plans are mandated to cover addiction treatment, including Suboxone. However, the specifics—such as copays and deductibles—vary by plan.
Financial barriers can impact recovery success. Research shows that even a $1 increase in daily out-of-pocket costs can reduce treatment retention by 14%.5
It is essential to verify your benefits before beginning treatment. Programs like Arista are equipped to help you review your insurance policy, explain your costs clearly, and explore any available financial assistance options. Ensuring treatment is affordable is key to maintaining long-term recovery.
Frequently Asked Questions
Can I receive Suboxone treatment through telemedicine in Ohio?
Yes, you can receive Suboxone treatment through telemedicine in Ohio! Since recent changes in federal rules, doctors can prescribe buprenorphine (the main medicine in Suboxone) after a virtual visit—even if you haven’t met in person first 6. This makes it much easier for people in Hilliard and across Ohio to start recovery, especially if getting to a clinic is hard due to work, transportation, or living far away. Telemedicine also helps protect privacy and can speed up getting help when you need it most. At Arista, you can connect with caring providers through secure video calls, so support is just a click away.
How long will I need to stay on Suboxone?
How long you’ll need to stay on Suboxone during Suboxone treatment in Hilliard, OH depends on your unique recovery journey. Some people may feel ready to taper off after several months, while others stay on Suboxone for a year or more. Research shows that being on medication for at least six months leads to fewer overdoses and better long-term health outcomes 1. There’s no one-size-fits-all timeline—your Arista care team will work with you to make a plan that fits your needs and keeps you safe. The most important thing is to move at your own pace and focus on your health and goals.
Is Suboxone safe if I’m pregnant or breastfeeding?
Yes, Suboxone can be used safely during pregnancy and breastfeeding, especially when prescribed and monitored by a healthcare provider. For someone in Hilliard or anywhere in Ohio, staying in treatment is often much safer than stopping suddenly. Research shows that buprenorphine (the main medicine in Suboxone) is linked to better outcomes for both moms and babies compared to methadone, with lower chances of premature birth and less risk of withdrawal symptoms in newborns 8. If you’re breastfeeding, studies suggest that very little buprenorphine passes into breast milk, making it generally safe. The care team at Arista will work closely with you and your OB/GYN to make sure you and your baby stay healthy throughout recovery.
Will my insurance cover Suboxone treatment in Hilliard?
Most insurance plans in Ohio—including Medicaid and private insurance—are required to cover Suboxone treatment in Hilliard, OH. This means your plan will likely help pay for your care, but the details can vary. Some plans pay the full cost, while others may have you pay a copay or part of the cost. Research shows that even a small increase in daily out-of-pocket costs can make it harder to stay in treatment, so understanding your coverage is important for your recovery journey 5. The team at Arista is here to help you review your insurance and find ways to make treatment as affordable as possible.
What’s the difference between Suboxone and methadone treatment?
Suboxone and methadone are both medicines used to help people recover from opioid addiction, but they work in different ways. Suboxone (used in Suboxone treatment in Hilliard, OH) contains buprenorphine and naloxone. It can be prescribed by regular doctors and taken at home, making it more flexible for most people. Methadone is usually given out at special clinics and requires daily visits. Suboxone has a built-in safety feature called the “ceiling effect,” which lowers the risk of overdose compared to methadone 4. Both medicines lower overdose risk by about a third, but Suboxone is often easier to access for Ohio families 2. Arista can help you find the right fit for your needs.
Can I work or drive while taking Suboxone?
Yes, most people can work and drive safely while taking Suboxone as part of Suboxone treatment in Hilliard, OH. Once your dose is stable and you’re used to the medication, it usually doesn’t make you feel drowsy or “out of it.” In fact, Suboxone is designed to help you feel normal so you can get back to your daily activities. However, just like with any new medicine, you shouldn’t drive or operate heavy machinery until you know how it affects your body. If you ever feel sleepy or dizzy, talk to your Arista care team—they’ll help you adjust your treatment for safety 4.
What happens if I relapse while on Suboxone treatment?
If you relapse while taking Suboxone as part of Suboxone treatment in Hilliard, OH, it doesn’t mean you’ve failed or that treatment isn’t working. Relapse is common and can be part of the recovery process. Think of it like slipping while learning to ride a bike—you might fall, but you can always get back up. The most important thing is to let your Arista care team know right away. They’ll help you adjust your plan and look at what triggered the slip, so you can avoid it next time. Studies show that staying connected to medication and support reduces the risk of overdose, even if you have a setback 1. Recovery is a journey, and you’re never alone.
Conclusion
Understanding the treatment landscape in Ohio reveals a wide range of evidence-based approaches, from outpatient counseling to medication-assisted treatment. The data is encouraging: individuals who complete structured programs show significantly higher long-term recovery rates than those who attempt to quit without professional support. Combining therapeutic interventions with medical oversight creates the strongest foundation for lasting change.
Recovery is a deeply personal journey, but you do not have to navigate it alone. Organizations throughout Ohio, including Arista Recovery, offer comprehensive resources designed specifically for residents seeking evidence-based care. By integrating medical support, therapeutic counseling, and wellness strategies, we create coordinated care plans tailored to your unique needs. Whether you are exploring options for yourself or a loved one, compassionate professionals are ready to answer your questions and help you find the path that works best for you. Hope is not just possible—it is within reach.
References
- Comparative Effectiveness of Different Treatment Pathways for Opioid Use Disorder – JAMA Network. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2760032
- Treating Opioid Disorder Without Meds More Harmful Than No Treatment – Yale News. https://news.yale.edu/2023/12/19/treating-opioid-disorder-without-meds-more-harmful-no-treatment-all
- During the COVID-19 Pandemic, Opioid Overdose Deaths Revert to Previous Record Levels in Ohio – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8919935/
- What is Buprenorphine? Side Effects, Treatment & Use – SAMHSA. https://www.samhsa.gov/substance-use/treatment/options/buprenorphine
- Do Out-of-Pocket Costs Influence Retention and Adherence to Buprenorphine Treatment? – PMC. https://pmc.ncbi.nlm.nih.gov/articles/PMC8314254/
- NIDA HEAL Opioid Use Disorder and Overdose Strategic Plan FY 2025 – NIDA. https://nida.nih.gov/publications/2022-2026-nida-strategic-plan/heal-opioid-use-disorder-overdose-strategic-plan/nida-heal-opioid-use-disorder-overdose-strategic-plan-fy-2025
- Understanding the Opioid Overdose Epidemic – CDC. https://www.cdc.gov/overdose-prevention/about/understanding-the-opioid-overdose-epidemic.html
- Buprenorphine Versus Methadone for Opioid Use Disorder in Pregnancy – New England Journal of Medicine. https://pubmed.ncbi.nlm.nih.gov/36449419/
- Medication Assisted Treatment Program Overview – ASAM. https://www.asam.org/docs/default-source/education-docs/mat-program-overview_2-12-2019239e2b9472bc604ca5b7ff000030b21a.pdf
- Barriers to Broader Use of Medications to Treat Opioid Use Disorder – NIH. https://www.ncbi.nlm.nih.gov/books/NBK541389/


