Recovery Decision Guide & Key Takeaways
Is Integrated Care Right for You?- Assessment Score: If you answer “Yes” to 2+ of the following, integrated care is recommended:
- Do you use substances to cope with anxiety, depression, or trauma?
- Have you tried treating just one issue (addiction or mental health) without lasting success?
- Do symptoms of one condition get worse when the other flares up?
- Top 3 Success Factors:
- Simultaneous Treatment: Addressing both conditions at once reduces relapse risk by 40-60%.
- Duration of Care: Programs lasting 90+ days show significantly higher long-term sobriety rates.
- Active Aftercare: Continued engagement in alumni groups or therapy is crucial for chronic management.
- Immediate Next Action: Call 988 for immediate crisis support or contact an Ohio provider today to verify your insurance benefits.
Understanding Co-Occurring Disorders in Mental Health and Addiction Treatment Ohio
- Do you feel anxious or depressed when you are not using substances?
- Has a doctor ever diagnosed you with a mental health condition alongside substance use?
- Do you feel that your substance use is a way to “quiet” your mind?
When you are navigating the complex landscape of mental health and addiction treatment Ohio offers, it is crucial to understand that these challenges rarely exist in isolation. Co-occurring disorders—often called dual diagnosis—describe the simultaneous presence of a substance use disorder alongside one or more mental health conditions. This combination affects millions of Americans, and understanding this connection is the first step toward meaningful recovery.
Research shows that approximately half of individuals experiencing psychiatric conditions will also face chemical dependency at some point in their lives, according to the National Institute on Drug Abuse. The relationship works both ways: conditions like depression, anxiety, PTSD, or bipolar disorder can increase vulnerability to addiction, while drugs or alcohol can trigger or worsen psychological symptoms. This creates a challenging cycle where each condition reinforces the other.
You might notice this pattern in different ways. Perhaps you’ve been using alcohol to manage anxiety symptoms, only to find your anxiety intensifying between drinking episodes. Or maybe you’ve turned to prescription medications to cope with depression, leading to dependency that deepens your emotional struggles. These scenarios aren’t signs of weakness—they’re indicators of co-occurring disorders that require specialized attention.
Traditional treatment approaches that address only addiction or only emotional well-being often fall short because they’re treating just part of the problem. When you leave one condition untreated, it typically undermines progress on the other. That’s why recognizing the interconnected nature of these conditions is so critical to your recovery journey.
The good news is that integrated treatment—addressing both conditions simultaneously—has proven remarkably effective. By understanding how your psychological well-being and chemical dependency interact, you can work with treatment professionals to develop a comprehensive recovery plan. This approach doesn’t just support your journey to sobriety; it strengthens your overall emotional wellness, giving you the tools to build a healthier, more stable future. The key is finding treatment options that recognize and address this dual challenge.
Why Mental Health and Addiction Connect
Mental health struggles and substance use often operate like a cycle: stress, depression, or anxiety can make someone more likely to use drugs or alcohol as a way to cope. Over time, substance use can change brain chemistry, making symptoms of depression, anxiety, or trauma even stronger. Studies show that about half of people with a substance use disorder will also have a mental health condition at some point in their lives, and the reverse is true too2. This strong connection is why experts in mental health and addiction treatment Ohio recommend treating both at the same time for the best chance at lasting recovery.
The 50% Rule: Half Face Both Challenges
The “50% rule” is a simple way to remember just how common it is for people to face both mental health and substance use challenges at the same time. In Ohio and across the U.S., about half of those who struggle with addiction will also have a mental health condition at some point, and the reverse is true as well2. This means if you or someone you care about is dealing with one, it’s very likely the other is involved, too.

“This overlap is why local experts recommend integrated care for lasting results, not just focusing on one piece of the puzzle.”
At Arista, we understand how this connection shapes real people’s recovery journeys, offering support that addresses both mental health needs and substance use. When you recognize just how common co-occurring disorders are, it can feel less isolating—and more hopeful—knowing help is available through mental health and addiction treatment Ohio centers like ours.
How Trauma Creates Dual Vulnerabilities
Trauma can act like a storm that shakes up how the brain and emotions work. When someone experiences trauma—like childhood abuse, neglect, or a major loss—it often leaves them feeling anxious, on edge, or hopeless. To cope, many turn to drugs or alcohol, hoping for relief. But over time, this can lead to addiction, while the original pain of trauma still lingers. That’s why trauma and substance use so often show up together, making recovery harder without support for both6.
In Ohio, mental health and addiction treatment programs now focus on trauma-informed care—this means addressing the root causes, not just the symptoms, and creating a safe space for healing. Action Step: If you suspect trauma is a root cause, ask potential providers specifically about their “trauma-informed” protocols during your initial call.
Common Mental Health and Addiction Pairs
Certain mental health conditions and substance use disorders frequently appear together, acting like teammates that work against your recovery. When depression and substance use combine, each makes the other harder to manage. For example, it’s common for someone struggling with anxiety to start using substances to feel calmer, only for those substances to make anxiety worse over time. In Ohio, providers see these combinations daily, which is why mental health and addiction treatment Ohio centers focus on supporting both at once2.
Depression, Anxiety, and Substance Use
Depression can feel like a heavy fog, while anxiety acts as a constant alarm. People sometimes use drugs or alcohol to cut through that fog or quiet the alarm, but the relief is usually short-lived. Over time, substance use can deepen the fog or make the alarm ring louder, leading to a tougher cycle to break. In Ohio, it’s common for treatment programs to see these challenges together, which is why mental health and addiction treatment centers like Arista focus on treating both at once for real progress2.
PTSD and Opioid Dependence Patterns
PTSD is often described as a wound that hasn’t fully healed. When someone experiences flashbacks or intense anxiety, opioids may seem to offer a quick escape. But over time, using these drugs can deepen both the emotional pain and the risk of physical addiction. In Ohio, nearly 76% of drug overdose deaths involved opioids in 2023, showing how serious this pattern is3. Mental health and addiction treatment providers in Ohio, including Arista, use trauma-informed therapy to help people break this cycle and build trust again—with themselves and with others.
Integrated Mental Health and Addiction Treatment Ohio Approaches
| Treatment Model | Focus | Outcome |
|---|---|---|
| Sequential | Treats one condition first, then the other. | High relapse risk; untreated issues trigger setbacks. |
| Parallel | Treats both at the same time but with different teams. | Conflicting advice; lack of coordination. |
| Integrated (Recommended) | One team treats both conditions simultaneously. | 40-60% better long-term recovery rates. |
When you’re dealing with both a substance use disorder and a mental health condition, getting help for just one won’t give you the lasting recovery you deserve. That’s why integrated treatment—where both conditions are addressed simultaneously by a coordinated team—has become the gold standard in dual diagnosis care.
Integrated approaches work because they recognize that your psychological well-being and addiction are interconnected. For example, if you’re using alcohol to cope with anxiety, treating only the drinking problem leaves the underlying anxiety untreated, making relapse much more likely. Similarly, addressing depression without acknowledging patterns of dependency means missing a critical piece of the puzzle. Research consistently demonstrates this approach’s effectiveness: studies show that integrated treatment improves long-term recovery outcomes by 40-60% compared to treating conditions separately.
Effective integrated treatment typically includes several key components working together. Medication-assisted treatment may help stabilize withdrawal symptoms and psychiatric conditions, while evidence-based therapies like Cognitive Behavioral Therapy (CBT) and Dialectical Behavior Therapy (DBT) teach you practical skills for managing both conditions. Many programs also incorporate group therapy, where you’ll connect with others facing similar challenges, and family therapy to rebuild relationships and create a supportive home environment.
What makes these approaches successful is the coordination. Your treatment team—which might include psychiatrists, therapists, counselors, and peer support specialists—communicates regularly to ensure everyone’s working toward the same goals. In practice, this might look like your psychiatrist adjusting your anxiety medication based on direct feedback from your therapist about specific triggers identified during your CBT sessions, or your counselor sharing insights about stress patterns with your group facilitator to provide more targeted support. This prevents the frustrating experience of receiving conflicting advice or having one provider unaware of what another recommended.
You’ll find integrated treatment programs that tailor these evidence-based approaches to your specific needs. Whether you’re dealing with depression and opioid use, bipolar disorder and alcohol dependence, or PTSD and stimulant use, the right program will create a personalized plan that addresses your unique situation. Recovery is possible when both conditions receive the comprehensive, coordinated attention they require.
Why Treating Both Conditions Simultaneously Matters
Think of recovery as trying to patch holes in a boat: if you only fix one leak, the other keeps letting water in. Research shows that integrated treatment, where both mental health and substance use are addressed together, leads to better outcomes and fewer relapses than treating each issue on its own5. That’s why mental health and addiction treatment Ohio providers, like Arista, coordinate care so you’re not left struggling with half the help you need. Integrated care brings together therapy, medications, and support for your whole situation—not just one part.
Evidence Behind Integrated Care Models
Imagine trying to fix a puzzle with missing pieces—if you only treat one issue, the picture stays incomplete. Research shows that integrated treatment for co-occurring disorders is consistently more effective than separate treatment plans, helping people achieve stronger recovery and fewer relapses5. Programs that bring together mental health and substance use care—like many at Arista—support people as whole individuals, not just as a set of symptoms. This approach is now the best practice in mental health and addiction treatment Ohio, and it’s backed by national and local experts for a reason: it works.
Medication-Assisted Treatment Options
Medication-assisted treatment (MAT) acts as a bridge: it helps steady someone during tough times, while therapy builds the tools for long-term healing. FDA-approved medicines, like buprenorphine, methadone, or naltrexone, work alongside counseling to support recovery—not just replace one problem with another. Studies show MAT leads to better recovery outcomes than therapy alone and can even lower the risk of overdose4. Sadly, only about 23% of public programs in Ohio offer MAT, so finding a center like Arista that provides these options is a real advantage for those seeking mental health and addiction treatment Ohio.
Therapy Modalities for Dual Diagnosis
Therapy functions as a set of tools: CBT helps you spot and change unhelpful thoughts and habits, while trauma-focused care helps you safely process painful experiences from your past. When these approaches are combined, people are more likely to stay in treatment, feel better, and avoid relapse7,6. At Arista, we use these evidence-based therapies to support individuals and families, meeting you where you are on your recovery journey.
Cognitive-Behavioral Therapy Foundations
Picture your thoughts, feelings, and behaviors like gears in a machine—if one gets stuck, the whole process can break down. CBT teaches you to spot patterns (like negative self-talk or urges to use substances), challenge those patterns, and practice new, healthier responses. Research shows CBT is especially helpful for people with dual diagnosis, leading to better progress and fewer relapses compared to doing nothing at all7. Many Ohio recovery centers, including Arista, use CBT as a core part of their treatment plans because it’s practical, flexible, and gives you skills to use every day.
Trauma-Focused Treatment Protocols
Imagine trauma as a wound that keeps getting poked. Trauma-focused protocols gently help you process those memories in a safe, guided way, so they lose their power to cause daily pain or trigger substance use. Studies show that these approaches lead to better outcomes than coping-focused methods alone, especially for people dealing with both PTSD and addiction6,8. Arista offers trauma-informed care as part of mental health and addiction treatment Ohio, creating safe spaces where healing can truly begin for you or your loved one.
Finding Treatment in Ohio: Access Guide
- Is the facility accredited by The Joint Commission or CARF?
- Do they offer integrated treatment for both mental health and addiction?
- Is medical detox available on-site?
- Do they accept your specific insurance plan?
Now that you understand what effective integrated treatment looks like, let’s explore how to access these services in Ohio. Finding the right treatment program can feel overwhelming, but Ohio offers numerous pathways to recovery support. Whether you’re seeking care for yourself or a loved one, understanding your options is the first step toward healing.
Start by reaching out to your primary care physician, who can provide referrals to specialized treatment centers and coordinate care. Many Ohio residents also find support through the Ohio Department of Mental Health and Addiction Services (OhioMHAS), which maintains a comprehensive directory of licensed treatment providers across the state.
Insurance coverage varies, so contact your provider to understand what behavioral health services your plan includes. Most major insurance plans now cover psychiatric and addiction treatment at similar levels to medical care, thanks to parity laws. If you’re uninsured or underinsured, Ohio offers several assistance programs and sliding-scale payment options through community wellness centers.
When evaluating treatment programs, consider factors like location, treatment philosophy, staff credentials, and the specific services offered. Look for facilities that provide evidence-based therapies and have experience treating co-occurring disorders. Accreditation from organizations like The Joint Commission or CARF International indicates quality standards are being met. Green flags include programs that offer individualized treatment plans and involve family in the recovery process, while red flags include facilities that promise quick fixes or use a one-size-fits-all approach without personalized assessment.
Don’t hesitate to ask questions during initial consultations. Inquire about staff-to-client ratios, family involvement opportunities, aftercare planning, and success metrics. A reputable program will be transparent about their approach and outcomes. Arista Recovery, for example, is one Ohio provider specializing in integrated treatment for co-occurring disorders, offering comprehensive assessment and evidence-based care coordination.
For immediate assistance, Ohio’s crisis hotline (988) connects you with trained counselors 24/7. They can provide immediate support and guide you toward local resources. Remember, seeking care is a sign of strength, not weakness. Recovery is possible, and taking that first step toward treatment opens the door to a healthier, more fulfilling life. The right support system is waiting to assist you in beginning your journey.
Overcoming Barriers to Care in Ohio
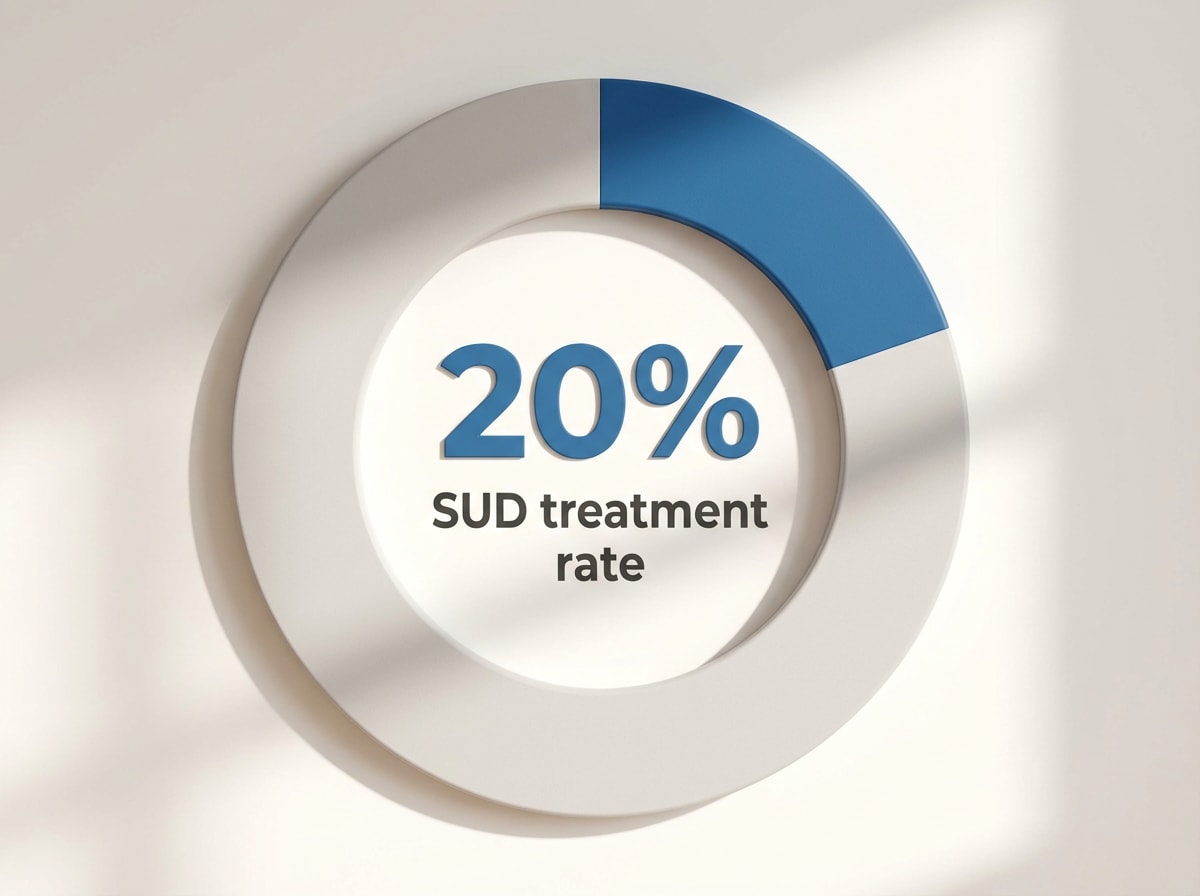
The biggest hurdles for many people are confusion about insurance, worries about confidentiality, and fear of being judged. In Ohio, only about 20% of people with substance use disorders actually get the help they need, often because of these barriers1,9. The good news? Resources like Arista can help you verify insurance coverage, explain your rights to privacy, and connect you with nonjudgmental, local care. Telehealth and community-based programs have made access easier, and you’re never alone in facing these challenges.
Insurance Coverage and Verification Steps
First, grab your insurance card and call the number on the back. Ask if your plan covers both mental health and substance use treatment, and whether places like Arista are in-network. Next, ask about deductibles, co-pays, and any limits on visits or medications. If talking to the insurer feels confusing, many Ohio treatment centers, including Arista, can help you verify coverage and explain your options. People without insurance are 50% less likely to get treatment, so checking coverage early can really open doors9.
Addressing Stigma and Confidentiality
Stigma—the fear of being judged—can keep people from seeking help, even when they need it most. In Ohio, this barrier is common, making it vital to find providers who offer nonjudgmental support. Confidentiality means your treatment details stay private. By law, centers like Arista must protect your information, so you can focus on healing without worry. Studies show that when people feel their privacy is protected and support is welcoming, they’re far more likely to begin treatment and stick with it1,9.
Specialized Programs for Your Situation
Specialized treatment matters because everyone’s story is different. Some Ohio clinics have gender-specific groups, others focus on trauma-informed care for those with tough pasts, and many now offer support designed for LGBTQ+ clients or veterans. These targeted programs improve engagement and results, helping people feel truly seen and understood6. Arista is dedicated to connecting you with the right resources—because mental health and addiction treatment Ohio can and should fit your unique situation.
Gender-Specific and LGBTQ+ Programs
Think of these programs like a custom-fit jersey—tailored to your life, not just the average person’s. In Ohio, some centers offer women’s or men’s groups that focus on issues like parenting, trauma, or healthy relationships. LGBTQ+ programs provide care that respects identity and addresses the risks of stigma and isolation. Studies show that specialized programs help people engage more in treatment and see better results6. At Arista, we connect you with gender-specific and LGBTQ+ mental health and addiction treatment Ohio options designed for your real life.

Veterans and Trauma-Informed Services
Imagine carrying invisible scars from service or life events that make daily life and recovery harder. Veterans often face PTSD, anxiety, or substance use challenges at higher rates than the general public. Ohio recovery centers, including Arista, now provide trauma-informed care—meaning your story is met with respect and tailored support. Evidence shows that integrated, trauma-focused interventions lead to the best results for veterans with both PTSD and addiction, much more than standard coping-focused methods6. Mental health and addiction treatment Ohio programs for veterans might include therapies like EMDR or cognitive processing therapy, plus peer groups with others who “get it.”
Building Your Long-Term Recovery Plan
- Days 1-7: Medical Detox & Stabilization
- Days 8-45: Residential Treatment & Intensive Therapy
- Days 46-90: Transition to Outpatient & Skill Building
- Day 91+: Aftercare, Alumni Support & Maintenance
Recovery doesn’t end when treatment does—it’s an ongoing journey that requires planning, commitment, and support. Creating a comprehensive long-term recovery plan while you’re still in treatment gives you a roadmap for maintaining sobriety and building the life you want after leaving a structured program.
Your recovery plan should address several key areas of your life. Start with your living situation: will you return home, move to a sober living facility, or find new housing that supports your recovery? Consider your daily routine, including work or school, exercise, healthy meals, and sufficient sleep. These foundational elements create stability during a vulnerable transition period.
Building a strong support network is essential. Identify people who encourage your sobriety—whether that’s family members, friends from support groups, a sponsor, or your treatment team. Throughout the state, you’ll find numerous recovery communities through organizations like the Ohio Recovery Housing Association and local chapters of mutual support groups. Regular attendance at these meetings provides accountability and connection with others who understand your journey.
Your plan should also include strategies for managing triggers and high-risk situations. Work with your treatment team to identify your personal triggers—whether they’re people, places, emotions, or circumstances—and develop specific coping strategies for each one. This might include calling your sponsor, attending a meeting, practicing specific techniques like 5-minute box breathing exercises or progressive muscle relaxation, or engaging in physical activity like a brisk walk or workout session.
Finally, establish a crisis plan. Know exactly who to call and where to go if you’re struggling or experiencing thoughts of relapse. Your crisis plan should include at least three emergency contacts (such as your therapist, sponsor, and a supportive family member), the address and phone number of your nearest crisis center, and a written list of warning signs that indicate you need immediate support. Keep these emergency contacts readily available in your phone and written down in a place you can easily access. Remember that asking for help is a sign of strength, not weakness. With a solid plan in place and ongoing support from your recovery network, you’re setting yourself up for lasting recovery success.
From Detox to Residential Treatment
Think of detox as clearing a stormy sky: a safe, supervised process helps your body adjust and prepares you for what comes next. Residential treatment is like building a solid shelter—offering structure, therapy, and round-the-clock support so you can focus on healing both mind and body. Research shows that starting with a stable detox and then moving into residential care leads to better outcomes, with fewer relapses and stronger progress for people with co-occurring disorders5. At Arista, we guide you through each phase, using trauma-informed, integrated care proven to work for Ohio families seeking recovery.
Medical Detox Safety and Stabilization
Picture detox as a safe harbor in a storm. During medical detox, trained professionals watch over you as substances leave your system, managing withdrawal symptoms and any health risks. In Ohio, this care is essential for people with both mental health and addiction challenges—because withdrawal can sometimes trigger anxiety, depression, or even medical emergencies. Research shows that starting recovery with medically supervised detox leads to fewer relapses and better long-term outcomes5. At Arista, we use trauma-informed practices to help you feel supported and respected, building trust from day one. This first step is the foundation for all future treatment, ensuring your mind and body are ready for residential care.
Transitioning to Intensive Programming
Think of this transition as moving from an emergency room to a supportive classroom. After medical detox, your body is clearer, but your mind and emotions need focused help. Intensive programming offers daily therapy, group support, skill-building, and time to work through both mental health and substance use patterns. This step is especially important for people with co-occurring disorders, because it creates a safe, structured space to start new habits and prepare for life after treatment. Research shows that moving from detox into integrated, trauma-informed residential care—like the programs at Arista—leads to better long-term outcomes and fewer setbacks5.
Aftercare and Relapse Prevention Strategies
Think of aftercare as your safety net—a set of tools and connections that catch you if things get tough. In Ohio, mental health and addiction treatment centers like Arista help you design a plan that might include alumni groups, therapy check-ins, and community supports. Research shows ongoing support and structured relapse prevention cut the risk of setbacks and are key for treating addiction as a long-term condition, not just a short-term crisis5.
Ongoing Support and Alumni Resources
Think of alumni programs as your recovery family cheering you on. At Arista and other Ohio mental health and addiction treatment centers, these groups offer regular meetups, peer mentoring, and special events. Connecting with others who’ve walked a similar path makes it easier to handle triggers and celebrate milestones. Research shows that people who stay involved in aftercare and alumni networks have better long-term outcomes and are less likely to face setbacks5.
Managing Recovery as a Chronic Condition
Just like with other long-term conditions, staying well means keeping up with regular check-ins, using healthy coping skills, and having a plan for tough days. In Ohio, mental health and addiction treatment centers like Arista encourage ongoing self-care, relapse prevention plans, and open conversations with your support team. Research shows that treating addiction and mental health as chronic conditions—using a mix of aftercare, therapy, and community support—leads to better results and fewer setbacks5.
Frequently Asked Questions
As you consider these recovery planning steps, you likely have practical questions about the treatment process itself. Here are answers to some of the most common concerns families and individuals share when exploring treatment options.
Will my insurance cover dual diagnosis treatment in Ohio?
Most insurance plans in Ohio do cover dual diagnosis treatment—including care for both mental health and substance use challenges—thanks to state and federal rules that require equal coverage for these services. Your plan may pay for therapy, medication-assisted treatment, or residential care, but what’s covered and how much you’ll owe out-of-pocket can vary. It’s a smart idea to call the number on your insurance card and ask if mental health and addiction treatment Ohio providers like Arista are in-network. Centers such as Arista can also help you check your benefits and explain your options. Remember, people without insurance are 50% less likely to get treatment, so verifying your coverage early helps you access the support you deserve9.
How do I know if I need integrated treatment for mental health and addiction?
You might need integrated treatment if you’re struggling with both mental health symptoms—like depression, anxiety, or trauma—and issues related to alcohol or drug use. Some signs that integrated care could help include finding it hard to manage daily life, feeling that substance use makes your mental health worse (or vice versa), or noticing that past treatments for one problem didn’t fully help. In Ohio, almost half of people with a substance use disorder also face mental health challenges, which is why mental health and addiction treatment Ohio programs like Arista’s focus on treating both together for the best results2,5. If you see yourself in these patterns, reaching out for an assessment can be the first step toward recovery.
What happens if I’ve tried treatment before and it didn’t work?
If you’ve tried mental health and addiction treatment in Ohio before and didn’t get the results you hoped for, you’re not alone. Recovery is a journey, not a straight line—many people need more than one attempt to find the right fit or approach. Research shows that integrated, trauma-informed care is more effective than treating mental health or substance use separately, so trying a new program that addresses both can make a real difference5. At Arista, we know every person’s story is unique and offer flexible, supportive options tailored to your needs. Even if past treatment didn’t work, there’s always hope; each step forward gives you new tools and a better chance at lasting recovery.
Can I receive treatment while maintaining my job?
Yes, you can receive mental health and addiction treatment in Ohio while keeping your job. Many centers, including Arista, offer flexible outpatient programs, evening therapy sessions, and telehealth options so you can fit treatment around your work schedule. In fact, telehealth has made it much easier for Ohioans to access care without missing work, with studies showing a 143% increase in engagement for rural residents1. Outpatient and virtual mental health and substance use services let you stay at home and continue working, all while building a strong recovery foundation. If you’re worried about privacy or asking for time off, treatment providers can help you understand your rights and create a plan that supports both your health and your career.
Is medication-assisted treatment the same as replacing one addiction with another?
No, medication-assisted treatment (MAT) isn’t just swapping one addiction for another. MAT uses FDA-approved medications like buprenorphine, methadone, or naltrexone to help manage cravings and withdrawal while you work on recovery with counseling and support. These medicines don’t create a high when taken as prescribed; instead, they help stabilize your body and mind, making it easier to focus on healing. Studies show MAT leads to better recovery outcomes and lowers the risk of overdose compared to therapy alone4. In Ohio, mental health and addiction treatment programs like Arista combine MAT with therapy and peer support for a full-circle approach to lasting recovery.
How long does treatment typically last for co-occurring disorders?
Treatment length for co-occurring mental health and substance use disorders in Ohio can vary, but most people spend several months working on recovery—not just a few weeks. Many Ohio mental health and addiction treatment programs recommend at least 90 days of combined therapy, medical support, and aftercare to build lasting change. Some folks need more time, especially if symptoms are severe or if life’s stressors make progress slow. Experts say that treating addiction and mental health as ongoing (like managing diabetes) leads to better results and fewer setbacks, so staying connected to support even after formal treatment is key5. At Arista, your plan is personalized, with flexible options for outpatient or residential care, so you get the right amount of help for lasting wellness.
What if my loved one refuses to get help?
If your loved one refuses mental health and addiction treatment in Ohio, it can feel heartbreaking and frustrating. Many people hesitate to get help due to fear, stigma, or feeling they should handle things alone—over 75% of those not in treatment say they weren’t ready or didn’t think they needed help1. You can make a difference by staying supportive, listening without judgment, and gently sharing your concerns. Sometimes, connecting your loved one with a caring provider like Arista for an informational chat (not a commitment) can lower their defenses. Family support and patience often play a big role in encouraging someone to eventually reach out. If you need guidance, resources for families are available through Ohio recovery centers so you don’t have to navigate this alone.
Are there treatment options specifically for veterans in Ohio?
Yes, Ohio offers specialized mental health and addiction treatment programs just for veterans. These programs are designed to respect your military experience and help with challenges like PTSD, depression, or substance use that can come after service. Many Ohio treatment centers—including Arista—offer trauma-informed care, which means they use therapies proven to help veterans heal from both trauma and addiction. Options might include EMDR, cognitive processing therapy, and peer groups with other veterans who understand your journey. Studies show that integrated, trauma-focused treatment leads to the best outcomes for veterans facing both PTSD and substance use issues6. If you or a loved one is a veteran, reaching out to a provider like Arista can connect you with care that truly honors and supports your service.
How do I verify a treatment program’s credentials and success rates?
To verify a treatment program’s credentials and success rates in Ohio, start by checking for state licensure and national accreditation, such as from The Joint Commission or CARF. These certifications show a program meets high standards for mental health and addiction treatment. Next, ask the provider about their staff’s training and any specialties in dual diagnosis or trauma-informed care. For success rates, look for outcomes based on evidence (like how many clients complete the program and stay in recovery) and ask if these are tracked independently. Research shows that programs using integrated, evidence-based approaches—like those at Arista—deliver the best results for co-occurring disorders5. Don’t hesitate to request references or reviews from former clients. This helps you feel confident you’re choosing a trusted path to recovery.
What’s the difference between outpatient and residential treatment?
Outpatient and residential treatment are two main paths for mental health and addiction care in Ohio, each with its own strengths. Outpatient treatment lets you live at home and attend therapy sessions or groups during the day or evening—great if you have work, school, or family responsibilities. Residential treatment means staying at a treatment center full-time, with round-the-clock support, therapy, and a structured routine, which is especially helpful for people with severe symptoms or those needing a safe, substance-free setting. Research shows that both options are effective, and the best choice depends on your needs, safety, and support at home5. At Arista, we’ll help you decide which approach fits your recovery goals and life. Mental health and addiction treatment Ohio centers like ours offer both tracks, giving you the flexibility and care you need to heal.
Will my treatment information remain confidential?
Yes—your treatment information will remain confidential. In Ohio, all mental health and addiction treatment centers, including Arista, are required by law to protect your privacy. This means your records, conversations, and any details about your care can only be shared with your written permission or in special legal situations. Confidentiality helps you feel safe to open up and get the support you need. Research shows that when people know their information stays private, they’re more likely to seek and continue treatment for mental health and addiction issues1,9. If you have questions about how your information is protected, don’t hesitate to ask your provider. You deserve to feel secure as you take steps toward recovery.
What support is available for families during treatment?
Families in Ohio don’t have to go through recovery alone—there’s a wide range of support available during mental health and addiction treatment. Most centers, including Arista, offer family therapy sessions, education workshops, and support groups to help loved ones understand co-occurring disorders and learn healthy ways to communicate. These programs teach families how recovery works, how to set boundaries, and how to care for themselves while supporting someone they love. Research shows that family involvement leads to better outcomes and a higher chance of lasting recovery for everyone involved5. Many Ohio providers also connect families with local or online support groups, so no one has to feel isolated. If you’re looking for a team that includes your family in the process, Arista is here to guide you every step of the way.
How do I handle a relapse after completing treatment?
Relapse can feel discouraging, but it’s a common part of recovery from mental health and addiction—especially with co-occurring challenges. If you experience a setback after treatment in Ohio, remember: you haven’t failed. Experts see relapse as a sign that your recovery plan might need adjusting, not as the end of your journey. The best step is to reconnect quickly with your support system—this could mean reaching out to your counselor, joining a local or online group, or contacting your treatment team at Arista. Updating your relapse prevention plan, exploring new coping skills, and reviewing what triggered the return of symptoms can all help you regain stability. Research shows that treating addiction and mental health as ongoing, chronic conditions—with regular check-ins and aftercare—leads to stronger, longer-lasting recovery5. Mental health and addiction treatment Ohio providers like Arista are here to help you get back on track, no matter where you are in your journey.
Can telehealth be effective for addiction and mental health treatment?
Yes, telehealth can be highly effective for mental health and addiction treatment in Ohio. Virtual care lets you connect with therapists or recovery specialists from home, making it easier to start and stick with treatment—especially if you live in a rural area or have a busy schedule. Studies show that telehealth increases treatment engagement by 143% among rural residents, and people are 9.2% more likely to follow through with medication-assisted treatment plans when care is offered virtually1,7. At Arista, both telehealth and in-person options are available so you can choose what works best for you. Many Ohioans find that video appointments, online therapy groups, and virtual check-ins help them feel supported and make recovery more accessible. Telehealth is a strong option whether you’re seeking counseling, medication management, or ongoing support through mental health and addiction treatment programs.
Start Your Recovery Journey in Ohio Today
Taking the first step toward recovery is one of the most courageous decisions you’ll ever make. If you or someone you care about is struggling with addiction—especially when mental health challenges are part of the picture—you don’t have to face this alone. Throughout Ohio, compassionate care and evidence-based treatment programs are available to guide you toward a healthier, more fulfilling life.
Recovery looks different for everyone. Some people benefit most from residential treatment, where they can focus entirely on healing in a supportive environment. Others find success with outpatient programs that allow them to maintain work and family commitments while receiving professional care. The right path depends on your unique circumstances, the severity of your addiction, any co-occurring mental health conditions, and the support systems you have in place.
Whether you’re dealing with depression and addiction, anxiety and substance use, PTSD and dependency, or any combination of mental health and addiction challenges, treatment centers across Ohio understand what you’re facing. They’ve helped thousands of people navigate the journey from dual diagnosis to lasting recovery, and they’re ready to support you too.
Many people worry about the unknowns: Will treatment work for me? What will my life look like afterward? How do I even begin? These concerns are completely normal. Treatment professionals are trained to address your questions, ease your fears, and create a personalized recovery plan that addresses both your addiction and mental health needs.
Recovery isn’t just about stopping drug or alcohol use—it’s about rediscovering who you are and building the life you deserve. It’s about healing relationships, developing healthy coping strategies, managing your mental health, and finding purpose again. The integrated support you need is available right here in your community.
Ready to take the next step? Start by calling your insurance provider to verify your behavioral health benefits and ask specifically about dual diagnosis coverage. Then contact two or three accredited programs that treat co-occurring disorders to schedule consultations—most offer free assessments. Ask about their approach to integrated treatment, staff credentials, and success rates. You deserve a program that treats the whole you, not just one piece of the puzzle. That first call isn’t just about getting information—it’s about reclaiming your future.
References
- National Survey on Drug Use and Health (NSDUH) 2024 Report. https://www.samhsa.gov/data/nsduh
- Screening and Treatment of Co-Occurring Disorders – SAMHSA. https://www.samhsa.gov/mental-health/serious-mental-illness/co-occurring-disorders
- Understanding the Opioid Overdose Epidemic – CDC. https://www.cdc.gov/overdose-prevention/about/understanding-the-opioid-overdose-epidemic.html
- Medication-Assisted Treatment Improves Outcomes for Patients With Opioid Use Disorder – Pew Charitable Trusts. https://www.pew.org/en/research-and-analysis/fact-sheets/2016/11/medication-assisted-treatment-improves-outcomes-for-patients-with-opioid-use-disorder
- Integrated Treatment of Substance Use and Psychiatric Disorders – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC3753025/
- Treatment of Co-Occurring PTSD and Substance Use Disorder in VA – VA/DoD. https://www.ptsd.va.gov/professional/treat/cooccurring/tx_sud_va.asp
- An Evaluation of Cognitive Behavioral Therapy for Substance Use Disorder – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC10572095/
- Post-Traumatic Stress Disorder (PTSD): Diagnosis and Treatment – Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/post-traumatic-stress-disorder/diagnosis-treatment/drc-20355973
- Healthcare Coverage and Service Access for Low-Income Adults with Substance Use Disorders – NIH. https://pmc.ncbi.nlm.nih.gov/articles/PMC9086121/
- PTSD and Trauma: New APA Guidelines Highlight Evidence-Based Approaches – American Psychological Association. https://www.apa.org/monitor/2025/07-08/guidelines-treating-ptsd-trauma


