Key Takeaways
- Integrated Care is Essential: Treating mental health and addiction simultaneously reduces relapse rates and improves long-term stability.
- Recognize the Signs: Look for patterns where substance use increases during emotional stress, or where mental health symptoms persist despite sobriety.
- Ohio-Specific Resources: Ohio offers robust integrated care options, including Arista Recovery, supported by mental health parity laws for insurance coverage.
- Actionable Timing: You do not need to wait for a crisis; progressive symptoms are a valid and recommended reason to seek help immediately.
Recognizing Co-Occurring Disorders
Psychological challenges rarely exist in isolation. If you are struggling with addiction, there is a strong likelihood that anxiety, depression, or other psychiatric conditions are also part of your experience. For many residents seeking dual diagnosis treatment Ohio, understanding this connection is the first step toward true recovery. These co-occurring disorders affect nearly half of all individuals seeking treatment for substance use disorders.
Perhaps you have noticed that you turn to substances when anxiety becomes overwhelming, or that depression seems to deepen during periods of active use. These patterns are not coincidences—they are signals that the brain is trying to manage multiple challenges simultaneously.
Common co-occurring disorders include depression, anxiety disorders, post-traumatic stress disorder (PTSD), bipolar disorder, and attention-deficit/hyperactivity disorder (ADHD). Each of these conditions can both contribute to chemical dependency and be exacerbated by it, creating a cycle that is difficult to break without professional support.
“Treating addiction alone while ignoring underlying psychological conditions often leads to relapse, while treating emotional disorders without addressing chemical dependency misses a critical piece of the puzzle.”
In Ohio, where access to integrated treatment has expanded significantly, addressing both conditions simultaneously has become the standard of care. The good news is that comprehensive treatment programs now routinely screen for co-occurring disorders. When both conditions receive attention, chances of sustained recovery improve dramatically.
What Dual Diagnosis Really Means
Dual diagnosis means having both a mental health condition and a substance use disorder at the same time. In Ohio, you might hear the terms “co-occurring disorders” or “dual disorders” used—they all describe the same challenge: mental illness and addiction happening together.
For example, someone could be living with depression and also struggling with opioid misuse. This combination is more common than you might think; about 21.2 million adults in the U.S. experience both at once1. Arista Recovery specializes in care for both, ensuring you or your loved one can move toward real, lasting recovery.
The Connection Between Mental Health and Addiction
Mental health conditions and addiction are closely linked. Sometimes, a person living with anxiety or depression might turn to alcohol or drugs for relief—this is called self-medicating. Other times, substance use can actually trigger or worsen mental health problems by changing brain chemistry2.
Research shows about half of people with a substance use disorder will experience a mental illness at some point in their lives1. This connection explains why dual diagnosis treatment Ohio is so important; by addressing both challenges at the same time, you increase the odds of real healing.
Common Co-Occurring Condition Combinations
Certain mental health and substance use combinations show up more often than others, especially here in Ohio. Recognizing these common pairings is key, as each combination may call for a slightly different treatment plan:
- Depression and Alcohol: Often go hand in hand as individuals try to numb emotional pain.
- Anxiety and Opioids/Stimulants: Anxiety disorders can appear alongside misuse of substances intended to calm or boost energy.
- PTSD and Substance Use: A frequent pairing that makes recovery complex due to trauma triggers1.
- Bipolar Disorder and Alcohol: Nearly half of people with bipolar disorder have an alcohol use disorder5.
Why These Conditions Occur Together
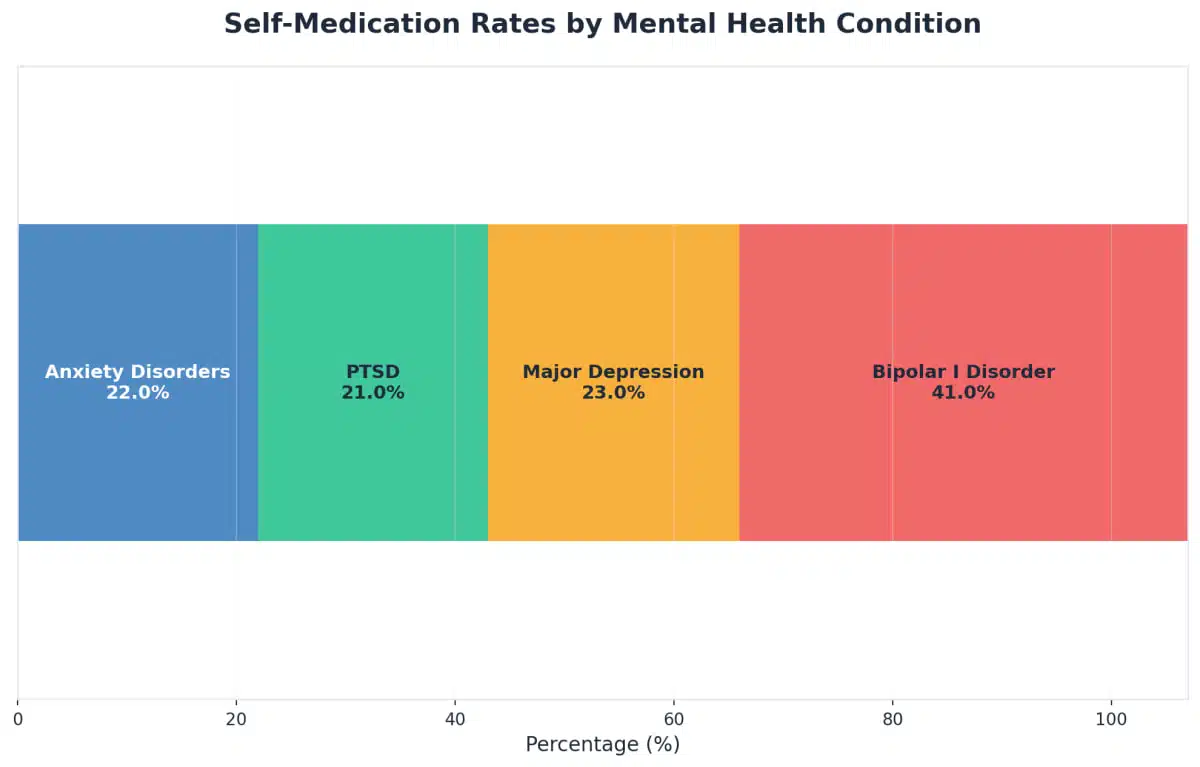
Why do mental health and substance use disorders often appear together? It is not just coincidence. Many people use drugs or alcohol to manage tough emotions or symptoms like anxiety, depression, or trauma. For instance, about 23% of people with major depression and over 21% with PTSD report using substances to cope with their feelings10.
In other cases, both conditions can develop because of shared risks like family history, ongoing stress, or changes in the brain2. Dual diagnosis treatment centers in Ohio—such as Arista—understand these connections and tailor care to your unique situation.
Self-Medication and Symptom Management
Self-medication means trying to manage tough mental health symptoms by using alcohol or drugs. In Ohio, this is a common path for many who want quick relief from emotional pain. Although turning to substances might seem to help at first, it often leads to more serious problems, including addiction and worsened mental health over time.
This cycle makes it much harder to break free without support. Dual diagnosis treatment centers in Ohio understand that true recovery means addressing both the mental health issue and the substance use together.
Shared Risk Factors and Brain Changes
Some people in Ohio face both mental health struggles and substance use because of shared risk factors—like family history, chronic stress, or early life trauma. These risks can affect how the brain develops and handles stress.
Substance use itself can also change brain chemistry, making mental health symptoms worse or harder to treat2. That is why dual diagnosis treatment centers in Ohio look at both the root causes and the brain changes when planning your care.
Self-Assessment for Dual Diagnosis Treatment Ohio
Taking an honest look at your current situation can be challenging, but recognizing when you need professional support is a powerful move toward recovery. If you are questioning whether it is time to seek help, your instinct is already pointing you in the right direction.
Consider whether drinking or drug use has begun affecting your daily responsibilities. Are you missing work, struggling to maintain relationships, or neglecting important commitments? When substances start interfering with the life you want to live, it is a clear signal that support could make a meaningful difference.
“Repeated unsuccessful attempts to control your use aren’t a personal failure; they’re an indication that you could benefit from structured treatment and professional guidance.”
For Ohio residents, access to quality care is closer than you might think. If you experience withdrawal symptoms during attempts to stop, if loved ones have expressed concern, or if you find yourself relying on substances to cope with difficult emotions, these are all valid reasons to reach out for help.
Warning Signs in Daily Life
Spotting the early signs that dual diagnosis treatment Ohio may be needed starts with tuning in to changes in everyday life. Use this quick checklist to evaluate your situation:
- Mood Instability: Have you noticed more frequent mood swings or trouble getting out of bed?
- Dependency for Function: Do you have a growing urge to use substances just to get through the day?
- Loss of Interest: Have you lost interest in activities you once enjoyed?
- Routine Disruption: Is it hard to keep up with school, work, or family routines?
If these warning signs sound familiar, you are not alone—over half of people living with both disorders do not receive help for either condition1. Seeking support from a trusted resource like Arista Recovery can help you regain balance.
Emotional and Behavioral Red Flags
Emotional and behavioral signs often signal it is time to consider dual diagnosis treatment. Are you noticing sudden irritability or feelings of emptiness that do not go away? Maybe you or your loved one have started isolating, feeling hopeless, or acting on risky impulses just to escape tough emotions.
These patterns are especially common when mental health struggles and substance use happen together. Research shows that untreated co-occurring disorders can raise suicide risk and make daily life much harder1. If these red flags are popping up, integrated dual diagnosis care can help you break the cycle.
Relationship and Work Disruptions
Relationship struggles and work problems often go hand in hand when someone is facing both mental health and substance use issues. Are you noticing more fights at home, missed family events, or friends drifting away? Maybe there has been trouble keeping a job, more absences, or a drop in performance.
These disruptions are common for people in Ohio dealing with co-occurring disorders. In fact, having both conditions increases the risk of job loss, social isolation, and family conflict compared to just one disorder alone7.
When Previous Treatment Hasn’t Worked
If you or your loved one has tried therapy, rehab, or medications in the past but things haven’t improved, it is time to look closely at dual diagnosis treatment Ohio. This approach is ideal when mental health and addiction keep feeding off each other.
Research shows that treating only one side of the problem leads to higher relapse rates and more severe symptoms than treating both together1. Integrated programs, like those at Arista Recovery, focus on the root of both challenges at the same time.
Repeated Relapse Patterns
If you have tried getting sober but keep falling into the same pattern of relapse, it might be a sign that dual diagnosis treatment is the missing piece. Many Ohio families notice this cycle: someone feels better for a while, but as soon as anxiety, depression, or trauma flares up, substance use returns.
Dual diagnosis programs are designed to break this loop by tackling both problems at once. If you are seeing repeated setbacks, it is worth considering this integrated support as your next step.
Worsening Symptoms Despite Sobriety
If you or your loved one has stayed sober but mental health symptoms like anxiety, depression, or mood swings seem to be getting worse, it may be time to consider dual diagnosis treatment Ohio. In Ohio, many find that untreated mental health issues can intensify during sobriety, making daily life difficult and increasing the risk of relapse.
Research shows that untreated co-occurring conditions can lead to more severe symptoms and greater impairment than facing just one disorder1. Integrated care helps you break the cycle and make real progress.
Decision Framework for Treatment Timing
Now that you have identified concerning signs, the natural next question is: when should you actually start treatment? The answer isn’t about waiting for the “perfect” moment—it is about recognizing when the cost of waiting outweighs the discomfort of change.
First, assess the trajectory. Are drinking or drug patterns stable, worsening, or improving? When patterns are escalating, earlier intervention typically leads to better outcomes. Research shows that individuals who enter treatment before experiencing severe consequences have significantly higher success rates.
Second, evaluate the capacity of your support system. Family members and friends who are currently willing to participate in the recovery process represent valuable resources. Their energy may diminish if the situation continues to deteriorate.
Third, consider life circumstances realistically. While there is rarely a “convenient” time for treatment, don’t let the search for ideal timing become a reason to postpone necessary care. Many Ohio residents find that addressing these challenges actually stabilizes other life areas more quickly than expected.
Evaluating Treatment Urgency
Determining how quickly to act can be difficult. Use the table below to distinguish between a situation requiring immediate emergency intervention and one that requires timely, structured admission to a program.
| Indicator Type | Signs & Symptoms | Recommended Action |
|---|---|---|
| Crisis Indicators | Thoughts of self-harm/suicide, aggressive outbursts, overdose, hallucinations, inability to care for self. | Immediate: Call 911 or go to the nearest ER. Contact Arista Recovery for crisis admission guidance. |
| Progressive Symptoms | Intensifying mood swings, increased tolerance, missing work/school, isolation, worsening anxiety/depression. | Urgent (24-48 hrs): Schedule an assessment with a dual diagnosis specialist to plan admission. |
Crisis Indicators Requiring Immediate Care
Certain crisis signs mean you shouldn’t wait. These include thoughts of self-harm, aggressive outbursts, or overdose. Research shows that untreated co-occurring disorders raise the risk for suicide and severe health complications1. If you see any of these crisis indicators, don’t hesitate—call 911 or reach out to a dual diagnosis center in Ohio like Arista Recovery immediately.
Progressive Symptoms Needing Intervention
Progressive symptoms are the slower-building warning signs that show dual diagnosis treatment in Ohio may be needed soon. Watch for patterns like mood swings that grow more intense or substance use that steadily increases. This approach works best when you are seeing things get gradually worse—missing more work or school, or drifting apart from loved ones.
Choosing Integrated Treatment Approaches
To choose the right integrated treatment approach for dual diagnosis treatment Ohio, ask yourself: does the program treat both mental health and substance use disorders at the same time? Prioritize integrated options, as research consistently shows they lead to better recovery and fewer relapses8.
Integrated treatment centers like Arista Recovery use evidence-based therapies—such as cognitive behavioral therapy (CBT) and dialectical behavior therapy (DBT)—that are proven to help with both substance use and mental health conditions2.
Why Simultaneous Treatment Works Better
Treating both mental health and substance use issues at the same time leads to better results. When care is integrated, symptoms on both sides improve faster. Research shows that integrated programs can reduce anxiety and depression symptoms by 18% to 27% more than programs that treat conditions separately8.
This approach works best when you want consistent teamwork: your mental health and addiction specialists communicate and share goals, so nothing falls through the cracks.
Evidence-Based Therapies for Dual Diagnosis
At Arista Recovery and other leading centers, evidence-based therapies are the gold standard. Two main types stand out:
- Cognitive Behavioral Therapy (CBT): Helps you spot and change unhelpful thoughts or actions linked to both substance use and mental health issues.
- Dialectical Behavior Therapy (DBT): Adds skills for managing tough emotions and building better relationships2.
Programs may also use trauma-informed care and motivational interviewing. Research shows these integrated approaches can reduce symptoms of depression and anxiety by up to 27% more than standard care8.
Starting Your Dual Diagnosis Treatment Ohio Journey
You have weighed your options and recognized that treatment is the right choice—now it is time to transform that decision into action. Taking your initial steps toward recovery doesn’t have to feel overwhelming when you have a clear, manageable path forward.

Within 24 hours: Schedule a confidential assessment with a qualified treatment provider. During this initial conversation—typically lasting 20-30 minutes—a trained counselor will ask about your substance use patterns and life circumstances. This assessment helps determine which level of care best fits your needs.
Within the first week: Gather the practical information you will need. Contact your insurance provider to understand your behavioral health benefits. Many Ohio treatment centers can verify your benefits and explain your financial responsibility before you commit.
Before treatment begins: Create a support system. Talk with trusted family members, friends, or your employer about your decision. Having people who understand your commitment makes the transition smoother.
Resource Planning and Preparation
Resource planning is a big part of preparing for dual diagnosis treatment Ohio. Start by making a checklist: gather your insurance cards, a current list of medications, and any mental health or substance use records you have. This info gives your Ohio care team a head start in building a plan that fits your journey.
Most dual diagnosis programs—like those at Arista Recovery—recommend organizing these documents before your first appointment. In Ohio, planning ahead also means checking transportation to your treatment center and setting aside time for initial assessments12.
Understanding Insurance Coverage in Ohio
Understanding insurance coverage is a key part of starting dual diagnosis treatment in Ohio. Begin by reviewing your insurance card or calling your provider to ask if mental health and substance use disorders are both covered—recent mental health parity laws mean most Ohio plans must offer similar coverage for both types of care9.
If you qualify for Medicaid or state-funded programs, these often include support for dual diagnosis services. Arista Recovery’s admissions team can help you verify coverage and explain what to expect, so you are not left guessing.
Preparing for Residential Treatment
Getting ready for residential dual diagnosis treatment in Ohio is all about making your first days more comfortable. Start by packing a small suitcase with comfortable clothes, personal toiletries, and any approved medications (in their original bottles).
Many Ohio centers, including Arista Recovery, recommend bringing a list of emergency contacts and key treatment records. Most dual diagnosis programs in Ohio ask families to plan for a stay of two to four weeks, though this may vary based on your needs12.
Your Next 30 Days Action Plan
Here is a practical 30-day action plan to help you start dual diagnosis treatment Ohio with confidence:
- Schedule Assessment: Most Ohio programs (like Arista Recovery) can arrange this within a week.
- Compile Resources: Gather insurance card, medication list, and treatment notes.
- Complete Screenings: Finish insurance verifications during weeks 1-2.
- Map the Plan: Meet with your care team to finalize your personalized roadmap.
- Engage Support: Keep close contact with family or trusted friends.
- Begin Therapy: By weeks 3-4, attend sessions focused on both mental health and substance use.
Week 1-2: Assessment and Verification
During weeks 1 and 2, you will go through a focused assessment and insurance verification process. Attend your first intake appointment—this usually includes a mental health and substance use screening, medical history review, and a chance to share your story.
Integrated treatment centers in Ohio use this period to tailor a plan that fits both your mental health and addiction needs, making sure nothing gets overlooked12.
Week 3-4: Starting Treatment and Support
In weeks 3 and 4, your journey shifts from planning to real action. Now you will start attending therapy sessions, group support, and skills classes. Most Ohio programs, including Arista Recovery, use evidence-based therapies like CBT and DBT to help you manage emotions and make healthier choices2.
Integrated care at centers like Arista can reduce anxiety and depression symptoms by up to 27% more than standard approaches8.
Finding Integrated Care in Ohio
Ohio has emerged as a leader in integrated behavioral health care, with over 50 designated Community Behavioral Health Centers across the state specifically equipped to address co-occurring disorders. These facilities represent a significant investment in comprehensive treatment infrastructure.
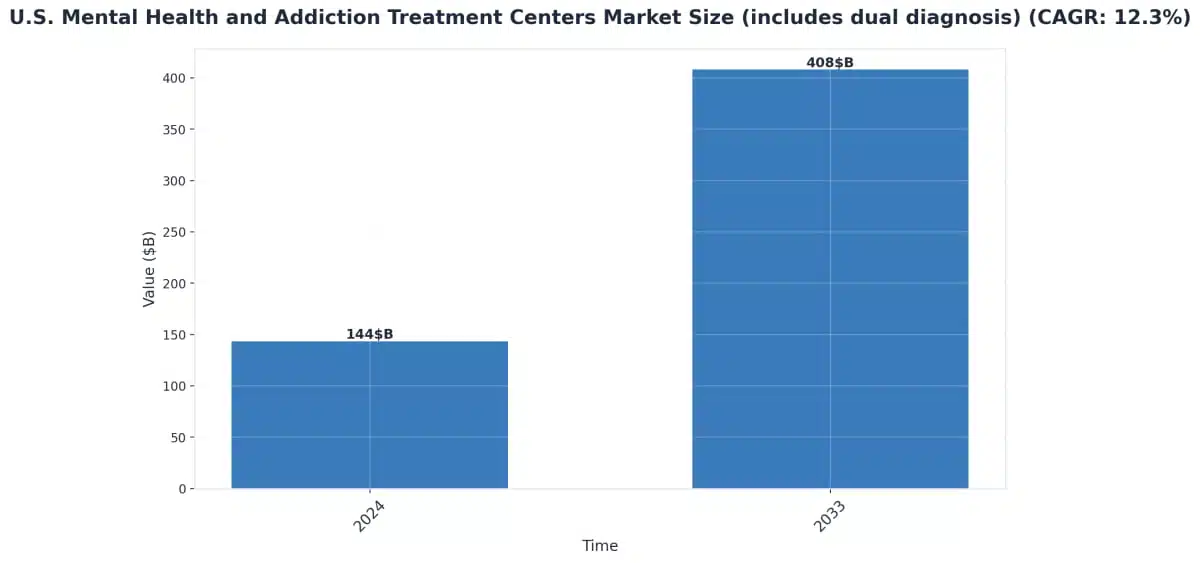
When evaluating integrated care programs in Ohio, look for specific indicators that the facility truly addresses co-occurring disorders. Effective integrated programs conduct unified assessments that examine both conditions together and assign coordinated care teams where providers actively collaborate.
During your evaluation of potential programs, ask how they handle co-occurring disorders specifically. Questions might include:
- “Do the same clinicians address both my mental health and substance use concerns?”
- “How do you coordinate medication management when treating both conditions?”
- “What does your assessment process look like for identifying co-occurring issues?”
You can identify Ohio’s integrated care facilities through the state’s Department of Mental Health and Addiction Services directory. Your primary care physician or current therapist can also provide referrals to reputable programs like Arista Recovery.
Frequently Asked Questions
You have learned how integrated care addresses both mental health and addiction together—but you probably still have specific questions about what this means for your situation. Let’s address the concerns that come up most often for people in Ohio considering this approach.
How do I know if my loved one needs dual diagnosis treatment versus standard addiction treatment?
The best way to know if your loved one needs dual diagnosis treatment instead of standard addiction care is to look for signs of both mental health struggles and substance use issues happening together. For example, if your loved one is dealing with anxiety, depression, mood swings, or trouble managing daily stress—and they’re also using alcohol or drugs to cope—dual diagnosis treatment Ohio is often the right choice. This approach works when symptoms like sadness, anger, or worry don’t improve with regular addiction treatment, or if there are cycles of relapse and emotional ups and downs1. In Ohio, it’s common to see conditions like PTSD, bipolar disorder, or severe anxiety paired with substance use. Integrated programs, like those at Arista Recovery, are designed for these situations, treating both sides at once so recovery is more successful.
What percentage of people with addiction actually have co-occurring mental health conditions?
About half of people living with addiction will experience a co-occurring mental health condition at some point in their lives. In fact, studies show that roughly 50% of those with a substance use disorder also deal with a serious mental illness, such as depression, anxiety, bipolar disorder, or PTSD1. This overlap is very common in Ohio, where families often see both challenges in the same loved one. The reverse is true, too—people with a mental health diagnosis are much more likely to develop addiction compared to the general population.
Will my insurance in Ohio cover dual diagnosis treatment?
Most insurance plans in Ohio now cover dual diagnosis treatment, thanks to improved mental health parity laws. This means your plan should provide similar coverage for both mental health and substance use care, whether you have employer insurance, Medicaid, or a private plan9. About 9.6% of Ohio adults with mental health needs had no insurance in 2024, so checking your coverage early is a smart step. Start by calling your insurance provider to ask if integrated treatment is included and if you need a referral or pre-approval. Arista Recovery’s admissions team can help you verify your benefits.
How long does dual diagnosis treatment typically take?
Dual diagnosis treatment in Ohio doesn’t look the same for everyone, but most people start with a two to four week assessment and early treatment period. After that, your journey might include outpatient therapy, group support, or ongoing medical care—which can last several months depending on your needs. Many Ohio programs, including Arista Recovery, recommend planning for at least 30-90 days of active treatment, followed by continued support to help you stay on track.
What happens if we only treat the addiction and not the mental health condition?
If you only treat addiction and skip addressing the mental health side, the chances of long-term recovery drop sharply. Many people in Ohio find that untreated depression, anxiety, or trauma can trigger a return to substance use, even after good progress in a rehab program. Research shows that when only one part of a co-occurring disorder is treated, relapse rates are much higher, and mental health symptoms can actually get worse—not better1. That’s why dual diagnosis treatment Ohio focuses on both issues at the same time.
Can someone start dual diagnosis treatment if they’re still using substances?
Yes, someone can begin dual diagnosis treatment in Ohio even if they’re still using substances. In fact, integrated care is designed to help people wherever they are on their recovery journey—including those who haven’t yet stopped using. Many Ohio programs, like Arista Recovery, expect that withdrawal and cravings are part of the early process, so they provide medical and emotional support from day one. Research shows that addressing both conditions together—right from the start—leads to better outcomes and lowers relapse risk compared to treating them separately2.
How do I choose between different dual diagnosis programs in Ohio?
To choose between dual diagnosis programs in Ohio, make a practical comparison checklist. Start by asking if the center offers integrated care—this means they treat mental health and substance use issues together, not separately. Research shows that integrated programs help lower anxiety and depression symptoms by up to 27% more than separate treatments8. Also, look for evidence-based therapies like CBT or DBT, and ask if the program encourages family involvement or offers aftercare support.
What if my family member refuses to admit they have a mental health problem?
It’s common for someone in Ohio to hesitate or even refuse to admit they have a mental health condition—especially when substance use is also present. Try to approach conversations with understanding and patience. Instead of pushing, focus on sharing your concerns gently: talk about specific changes you’ve noticed, like mood swings or trouble at work. If your family member won’t discuss mental health, you can still reach out for guidance from trusted resources like Arista Recovery.
Are medications used in dual diagnosis treatment, and are they safe?
Yes—medications are often part of dual diagnosis treatment in Ohio, and when prescribed and monitored by trained professionals, they are considered safe. Common examples include antidepressants for depression or anxiety, mood stabilizers for bipolar disorder, and medications that help reduce cravings or withdrawal symptoms for substance use disorders. The care team at places like Arista Recovery uses careful screening and regular check-ins to make sure each medicine matches your needs.
What’s the difference between integrated and non-integrated dual diagnosis treatment?
Integrated dual diagnosis treatment means you receive care for both mental health and substance use issues at the same time, with one team working together to support your whole recovery. In Ohio, centers like Arista Recovery use this model, so your therapists, doctors, and counselors all share information and build one plan just for you. Non-integrated treatment separates care—maybe you see a mental health provider in one place and a substance use counselor somewhere else, with little coordination.
How much does dual diagnosis treatment cost without insurance?
The cost of dual diagnosis treatment in Ohio without insurance varies widely. Outpatient services may range from several hundred to a few thousand dollars per month, while residential or inpatient dual diagnosis programs can be much more expensive—sometimes several thousand dollars per week. Many Ohio centers, including Arista Recovery, offer payment plans or sliding-scale fees. For those without insurance, the SAMHSA National Helpline (1-800-662-4357) can connect you to state-funded programs4.
Can dual diagnosis treatment help if previous rehab attempts have failed?
Yes—dual diagnosis treatment can absolutely help when past rehab attempts haven’t worked. Many Ohio families find that repeated relapses or stubborn symptoms are signs that both mental health and substance use need to be treated together, not separately. Research shows that integrated care for dual diagnosis leads to better recovery outcomes and up to 27% greater reduction in anxiety and depression symptoms compared to standard, non-integrated rehab programs8.
What role does family play in dual diagnosis treatment and recovery?
Family plays a big part in dual diagnosis treatment and recovery here in Ohio. When families get involved—by joining therapy sessions, learning about co-occurring disorders, or simply offering steady encouragement—recovery outcomes improve. Research shows that integrated dual diagnosis treatment, especially when it includes family support, helps lower relapse rates and strengthens long-term stability28.
Is telehealth an option for dual diagnosis treatment in Ohio?
Yes—telehealth is now a widely available option for dual diagnosis treatment in Ohio. Many treatment centers, including Arista Recovery, offer virtual therapy sessions, medication management, and support groups, so you can start or continue your recovery journey from home. This method works well for Ohioans who have busy schedules, live far from a treatment center, or face transportation barriers.
What happens after residential dual diagnosis treatment ends?
After you finish residential dual diagnosis treatment in Ohio, your journey isn’t over—it’s just moving to a new phase. Most people step down to outpatient care, which means you’ll still get therapy and support, but you’ll return home each day. You might join group sessions, meet with a counselor weekly, or check in with your care team at Arista Recovery to keep building healthy habits. Research shows that continuing care after residential treatment greatly improves long-term recovery8.
Conclusion
Finding the right support for addiction recovery—especially when co-occurring mental health disorders are part of the picture—is one of the most important decisions you and your loved ones will make. Throughout this guide, we have explored how integrated treatment addresses both addiction and psychological conditions simultaneously, offering the comprehensive care that leads to lasting recovery.
As you move forward with your decision, remember the key framework we discussed: start by assessing whether co-occurring disorders are present, then prioritize programs offering integrated dual diagnosis treatment with evidence-based therapies like CBT and DBT.
For those in Ohio, you have access to a range of quality treatment programs designed to address various addiction disorders and co-occurring psychological conditions. Resources like the Ohio Department of Mental Health and Addiction Services and facilities offering integrated care—including options like Arista Recovery—provide pathways to the comprehensive support you need.
You have now equipped yourself with the knowledge to make an informed decision about treatment. The next concrete step is to contact 2-3 programs that meet your criteria, ask your prepared questions, and if possible, schedule facility tours. Recovery is possible, you do not have to navigate this journey alone, and taking that first step toward integrated, evidence-based care is an act of courage that can transform your future.
References
- Co-Occurring Disorders and Other Health Conditions | SAMHSA. https://www.samhsa.gov/substance-use/treatment/co-occurring-disorders
- Finding Help for Co-Occurring Substance Use and Mental Disorders | NIMH. https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health
- Dual Diagnosis – MedlinePlus. https://medlineplus.gov/dualdiagnosis.html
- National Helpline for Mental Health, Drug, Alcohol Issues – SAMHSA. https://www.samhsa.gov/find-help/helplines/national-helpline
- Bipolar Disorder and Alcoholism: Are They Related? – Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/bipolar-disorder/expert-answers/bipolar-disorder/faq-20057890
- Interplay Between Alcohol Use, Mood, and Functioning in Bipolar Disorder. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2819705
- Posttraumatic Stress Disorder and Co-Occurring Substance Use Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC3811127/
- Integrated vs Non-Integrated Treatment Outcomes in Dual Diagnosis. https://pmc.ncbi.nlm.nih.gov/articles/PMC10157410/
- Mental Health By the Numbers – NAMI. https://www.nami.org/mental-health-by-the-numbers/
- Self-Medication with Alcohol or Drugs for Mood and Anxiety Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC6175215/”

