Key Takeaways: Your Action Plan
- Verify First: Always check your specific Humana plan details using the number on your card before committing to a facility.
- Know Your Rights: Federal laws ensure your addiction care is covered comparably to medical care; you have the right to appeal denials.
- Prioritize In-Network: Choosing an in-network provider like Arista Recovery significantly lowers your out-of-pocket costs.
- Prepare for Pre-Auth: Higher levels of care (like residential rehab) usually require prior approval; have your documentation ready.
- Immediate Action: If you are in crisis, call a provider immediately—they can often handle the insurance verification for you.
Understanding Humana Coverage for Addiction
What ACA Mandates Mean for Your Benefits
Navigating the complexities of insurance can be stressful, especially when you or a loved one needs help immediately. The most important thing to know right now is that addiction treatment that accepts Humana in Ohio is available and protected by federal law. Under the Affordable Care Act (ACA), all health insurance plans—including Humana—must classify substance use disorder treatment as an “essential health benefit.”
This mandate ensures that your plan covers critical services such as medical detox, outpatient therapy, and residential care just as it would cover treatment for a physical illness like diabetes or heart disease3. You are not alone in this process, and the law is on your side to ensure you get the care you need.
The “Parity” Rule: Think of parity as a fairness guarantee. It prohibits insurance plans from placing stricter limits or higher costs on addiction treatment than they do on medical or surgical care. If your plan offers unlimited doctor visits for a physical condition, it generally cannot cap your therapy sessions for addiction2.
Skill Checkpoint: Before moving on, ensure you understand that your request for addiction treatment cannot be automatically denied simply because it is behavioral health care. You have specific protections that ensure access to these services.
Verifying Your Specific Plan Details
While the ACA provides a safety net, every Humana plan varies regarding deductibles, co-pays, and network restrictions. To avoid surprise bills, you need to verify your specific benefits. The most reliable source of truth is your Summary of Benefits and Coverage, a document available through your online Humana portal or by calling member services1.

If reading insurance documents feels overwhelming, you can call the number on the back of your card. Use the script below to get clear answers regarding your coverage in Ohio.
"Hello, I am calling to verify my behavioral health benefits.
1. Is [Facility Name, e.g., Arista Recovery] in-network with my plan?
2. What is my deductible, and how much of it have I met this year?
3. Do I need pre-authorization for residential treatment or detox?
4. What is my maximum out-of-pocket cost for the year?"Alternatively, many Ohio families find it easier to let the treatment center handle this. Providers like Arista Recovery are experienced with addiction treatment that accepts Humana in Ohio and can perform a complimentary verification of benefits for you, explaining your costs in plain English2.
Services Covered by Addiction Treatment That Accepts Humana in Ohio
Medical Detox and Residential Treatment
Recovery often happens in stages, and Humana plans generally cover the full continuum of care. The first step is often medical detox, where you safely withdraw from substances under the supervision of doctors and nurses. This is critical for safety and comfort. Following detox, residential treatment provides a structured environment to build the foundation for long-term sobriety1.
Understanding the difference between these two levels of care helps you plan your time and resources effectively:
| Feature | Medical Detox | Residential Treatment |
|---|---|---|
| Primary Goal | Physical stabilization and safe withdrawal management. | Emotional healing, skill-building, and behavioral change. |
| Duration | Typically 3–7 days. | Typically 30–90 days. |
| Environment | Medical setting with 24/7 nursing support. | Home-like setting with 24/7 therapeutic support. |
Humana considers these services essential health benefits. Centers like Arista Recovery in Ohio are equipped to guide you seamlessly from detox directly into a residential program, ensuring there are no gaps in your care2.
MAT, Therapy, and Aftercare Options
Effective treatment extends beyond just stopping substance use; it involves treating the whole person. Humana plans in Ohio typically cover a range of therapeutic interventions designed to support lasting recovery.
- Medication-Assisted Treatment (MAT): This combines FDA-approved medications (like buprenorphine) with counseling to reduce cravings and prevent relapse. It is highly effective for opioid and alcohol use disorders5.
- Evidence-Based Therapy: Therapies such as Cognitive Behavioral Therapy (CBT) and Dialectical Behavioral Therapy (DBT) help you identify triggers and develop coping mechanisms. These are standard at top-tier Ohio facilities like Arista2.
- Family Therapy: Addiction affects the whole family. Humana often covers family sessions to help repair relationships and build a supportive home environment10.
- Aftercare Planning: Recovery is a lifelong journey. Coverage usually extends to outpatient counseling and alumni groups to help you maintain sobriety after leaving the facility.
Practice This: When speaking with a provider, ask specifically if they offer “integrated MAT and therapy” and if these specific services are billed under your Humana plan.
Navigating Pre-Authorization Requirements
When You Need Prior Approval
Pre-authorization (or prior authorization) is a check-point where your insurance company confirms that a proposed treatment is medically necessary before they agree to pay for it. For addiction treatment that accepts Humana in Ohio, this is almost always required for higher levels of care.

You should expect to need pre-authorization for:
- Inpatient residential rehab.
- Partial Hospitalization Programs (PHP).
- Intensive Outpatient Programs (IOP).
- Extended hospital stays for detox.
Routine doctor visits or standard outpatient therapy sessions are less likely to require this step, but it is always safer to check. Proceeding without approval can result in a denial of the claim, leaving you responsible for the full bill3.
Streamlining the Authorization Process
While the term “pre-authorization” sounds bureaucratic, the process can be handled quickly if you are prepared. The goal is to prove medical necessity. Most reputable treatment centers in Ohio have utilization review teams that handle this entire process for you.
Checklist: Documents Needed for Authorization
- Insurance Card: Front and back copies.
- Clinical Assessment: A recent evaluation from a doctor or counselor detailing your substance use history.
- Medical History: Records of any co-occurring physical or mental health conditions.
- Previous Treatment: Information on any past rehab stays (to show why a specific level of care is needed now).
If you are working with Arista Recovery, our admissions staff will contact Humana directly to submit these documents. Clear documentation and prompt communication can significantly reduce wait times, getting you into treatment faster2, 3.
Maximizing Benefits and Minimizing Costs
Choosing In-Network Providers in Ohio
The single most effective way to lower your treatment costs is to choose a facility that is “in-network” with Humana. In-network providers have a contract with Humana to provide services at a pre-negotiated, lower rate. This protects you from “balance billing,” where a provider charges you the difference between what they want to be paid and what insurance pays.
Why it matters: Using an in-network facility like Arista Recovery means your insurance covers a larger percentage of the bill, and your out-of-pocket maximums are lower. Out-of-network care often requires you to pay significantly more upfront and may not count toward your annual deductible2.
Action Step: Search the Humana provider directory online or ask the facility directly: “Are you in-network with my specific Humana plan?”
Understanding Your Out-of-Pocket Expenses
Even with great coverage, you will likely have some financial responsibility. Understanding the terminology helps you budget for your recovery journey. Here are the three main costs you might encounter with Humana plans in Ohio:
- Deductible
- The amount you must pay out-of-pocket before your insurance begins to pay. If your deductible is $2,000, you pay the first $2,000 of treatment costs.
- Co-pay
- A fixed fee you pay for a specific service, such as $30 for a therapy session or $150 for an admission fee.
- Coinsurance
- A percentage of the cost you share with Humana after meeting your deductible. For example, if your coinsurance is 20%, Humana pays 80% of the bill, and you pay the remaining 20%1.
Once you reach your Out-of-Pocket Maximum for the year, Humana will typically cover 100% of all further covered services. Checking where you stand on your deductible for the current year is a smart first step.
Finding Addiction Treatment That Accepts Humana in Ohio with Arista
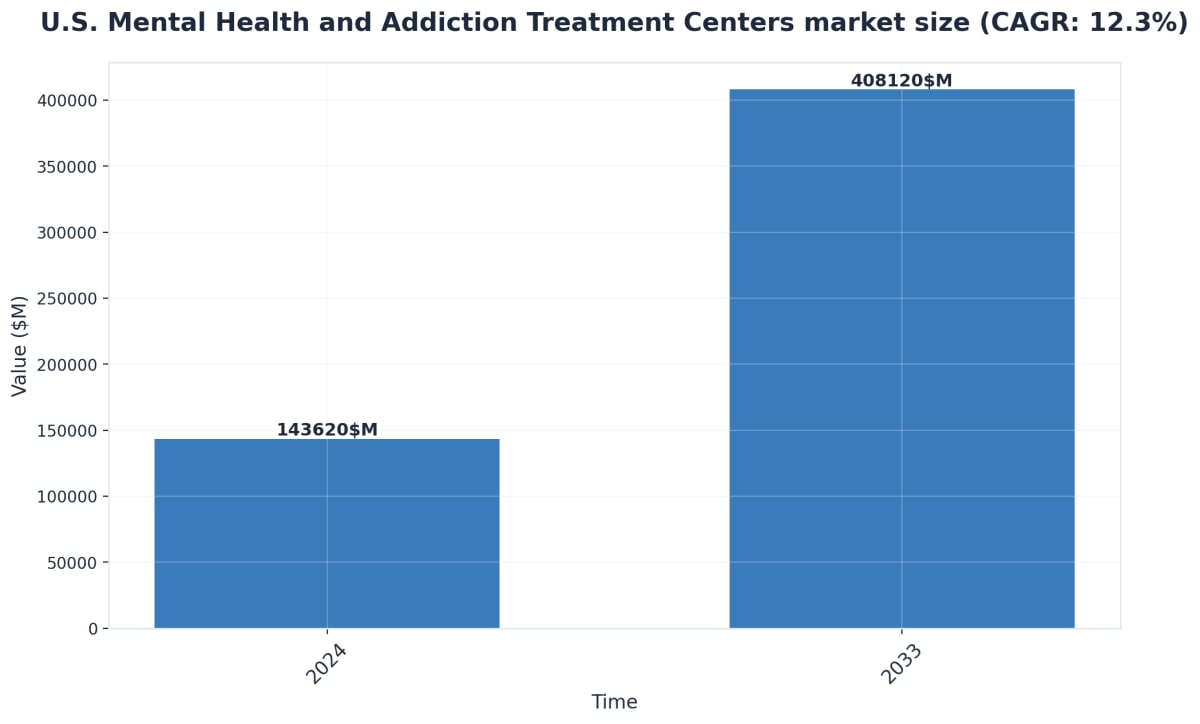
Finding effective addiction treatment in Ohio requires understanding what evidence-based care actually means and how to identify programs that deliver real results. Ohio has been significantly impacted by the addiction crisis—with over 5,000 overdose deaths annually in recent years—making access to quality treatment more critical than ever8. You need to know what questions to ask and what standards to expect when evaluating treatment options.
Evidence-based care refers to specific therapeutic approaches proven effective through clinical research. This includes Cognitive Behavioral Therapy (CBT), which helps you identify and change thought patterns that contribute to substance use; Medication-Assisted Treatment (MAT), combining FDA-approved medications with counseling for opioid or alcohol addiction; and Dialectical Behavior Therapy (DBT), which teaches coping skills for managing cravings and emotional triggers. Quality programs integrate these approaches rather than relying on a single method.
When evaluating treatment facilities in Ohio, look for specific credentials and offerings. Accreditation from organizations like The Joint Commission or CARF indicates adherence to quality standards. Programs should provide medical detox supervised by licensed physicians, individualized treatment plans based on comprehensive assessments, and multiple levels of care—from residential treatment to intensive outpatient programs that accommodate work or family obligations.
Decision Tree: Is this the right facility?
- Staff-to-Patient Ratio: Is it low enough to ensure personalized attention?
- Family Involvement: Do they offer structured family therapy sessions?
- Dual Diagnosis: Can they treat co-occurring anxiety or depression simultaneously?
- Aftercare: Is there a clear plan for what happens after discharge?
The right facility will explain exactly how they’ll address both the physical dependence and underlying factors contributing to addiction. When you’re ready to explore treatment options in Ohio, reach out to facilities that provide clear, specific answers about their methods and outcomes.
Frequently Asked Questions
What happens if my Humana plan denies coverage for a specific treatment level?
If your Humana plan denies coverage for a certain level of addiction treatment in Ohio, don’t lose hope. You can appeal the decision by asking for a review and providing extra medical information from your doctor or treatment team. The Affordable Care Act gives you the right to appeal any denial for essential health benefits, such as addiction treatment that accepts Humana in Ohio 3. Centers like Arista Recovery can help you gather paperwork and guide you through the appeal process, making it less overwhelming. Many families in Ohio find that appealing can lead to a different outcome and open the door to needed care.
Can family members participate in treatment even if they’re not Humana policyholders?
Yes, family members can take part in treatment even if they aren’t Humana policyholders. Many addiction treatment centers in Ohio, including Arista Recovery, strongly encourage family involvement because support from loved ones can help recovery last longer and reduce the risk of relapse. Family therapy is often covered as part of addiction treatment that accepts Humana in Ohio, and the focus is on healing relationships and building better communication, not just treating one person 10. Your family can join therapy sessions, support groups, and educational workshops alongside you—helping everyone move forward together.
How does Arista Recovery handle the transition from detox to residential care with Humana insurance?
Arista Recovery makes the move from detox to residential care smooth and supportive for those using Humana insurance in Ohio. After your detox—where medical staff help you safely manage withdrawal—Arista’s team works with both you and Humana to coordinate the next step. They handle the needed paperwork, confirm your benefits, and guide you through any pre-authorization so your care continues without gaps. This approach lets you focus on healing, not insurance details. Choosing addiction treatment that accepts Humana in Ohio at Arista means you get trusted, step-by-step support as you transition into a structured recovery environment 2.
Will my employer know if I use my Humana insurance for addiction treatment?
No, your employer will not know if you use your Humana insurance for addiction treatment in Ohio. All medical information, including treatment for substance use, is protected by privacy laws like HIPAA. When you use addiction treatment that accepts Humana in Ohio, your insurance claims are handled confidentially, and details about your care are not shared with your employer without your written permission. Only you and your healthcare providers can access this information. If you have questions about privacy or need extra reassurance, Arista Recovery can walk you through how your information stays protected 3.
What support does Arista Recovery offer after my Humana benefits are exhausted?
When your Humana benefits for addiction treatment run out, Arista Recovery doesn’t leave you on your own. The team will help you explore alternative support options, such as setting up payment plans, connecting you with local community programs, or linking you to sliding-scale services so you can keep moving forward in recovery. Arista’s staff can also guide you through applying for state-funded resources or other insurance plans if you qualify. Their focus is making sure that, even after your Humana coverage ends, you still have a clear path to ongoing care and support in Ohio 2.
Does Humana cover dual diagnosis treatment for co-occurring mental health conditions in Ohio?
Yes, Humana covers dual diagnosis treatment for people in Ohio who are facing both addiction and mental health concerns like depression or anxiety. This is required by the Affordable Care Act, which says insurance must include behavioral health care—including treatment for co-occurring disorders—as an essential benefit 3. If you or your loved one needs help for addiction and a mental health condition, you can find Ohio centers like Arista Recovery that offer integrated support using proven therapies such as CBT and DBT 7. With addiction treatment that accepts Humana in Ohio, you get a care plan tailored to both your mental health and substance use needs.
How quickly can I start treatment once Humana approves my pre-authorization?
Once Humana approves your pre-authorization for addiction treatment in Ohio, you can usually start care very soon—often within a few days, depending on the treatment center’s availability. At Arista Recovery, the team will contact you right away to schedule your admission and make sure everything is in place so you don’t have to wait longer than necessary. Many Ohio centers that offer addiction treatment that accepts Humana in Ohio work hard to minimize delays, knowing how important it is to begin recovery quickly. If you have questions or need support, Arista is ready to guide you through each next step 2.
Conclusion
Starting your recovery journey in Ohio means you have access to compassionate, evidence-based care designed to support lasting change. Understanding how insurance coverage works for addiction treatment helps you make informed decisions about your path forward without letting financial concerns become a barrier to getting help.
Recovery is possible, and navigating insurance doesn’t have to be complicated. Whether your plan is through an employer, the Healthcare Marketplace, Medicaid, or Medicare, coverage for substance use treatment is available. The key is knowing what questions to ask, what documentation to gather, and how to work with your treatment provider to maximize your benefits and minimize out-of-pocket costs.
Arista Recovery offers comprehensive treatment options throughout Ohio and works with most major insurance plans to make care accessible. Our team can verify your benefits, explain your coverage, and help you understand your financial responsibility before you begin treatment. We’re here to answer your questions about insurance, discuss your options, and guide you through the verification process. If you’re ready to explore treatment or simply want to understand what your insurance covers, contact us today for a free, confidential benefits check. Reaching out for help is a sign of strength, and recovery is possible with the right support behind you.
References
- Humana Insurance Coverage for Drug & Alcohol Rehab. https://rehabs.com/insurance-coverage/humana/
- Ohio Rehabs that Accept Humana. https://recovery.com/ohio/humana/
- Mental health & substance abuse coverage. https://www.healthcare.gov/coverage/mental-health-substance-abuse-coverage/
- Humana Health Insurance for Drug & Alcohol Rehab Treatment. https://rehabnet.com/insurance/humana/
- Medication-Assisted Treatment | Ohio Department of Mental Health and Addiction Services. https://dbh.ohio.gov/get-help/treatment-services/medication-assisted-treatment
- Medication-Assisted Treatment | ADAMHS Board of Cuyahoga County. https://www.adamhscc.org/resources/finding-help/by-service/medication-assisted-treatment
- Dual Diagnosis Treatment Centers in Ohio | Psychology Today. https://www.psychologytoday.com/us/treatment-rehab/ohio?category=dual-diagnosis
- Drug Overdose | Ohio Department of Health. https://odh.ohio.gov/know-our-programs/violence-injury-prevention-program/drug-overdose/
- Medications to Treat Opioid Use Disorder | National Institute on Drug Abuse. https://nida.nih.gov/research-topics/medications-opioid-use-disorder
- Family Therapy for Addiction Treatment. https://www.addictioncenter.com/treatment/family-therapy/

