Key Takeaways
- State Regulations: Ohio medical detox facilities must be licensed by OhioMHAS and adhere to strict ASAM guidelines for safety, staffing, and emergency preparedness.
- Major Metros Served: Comprehensive detox services are accessible across Ohio, with major hubs in Columbus, Cleveland, Cincinnati, and Dayton.
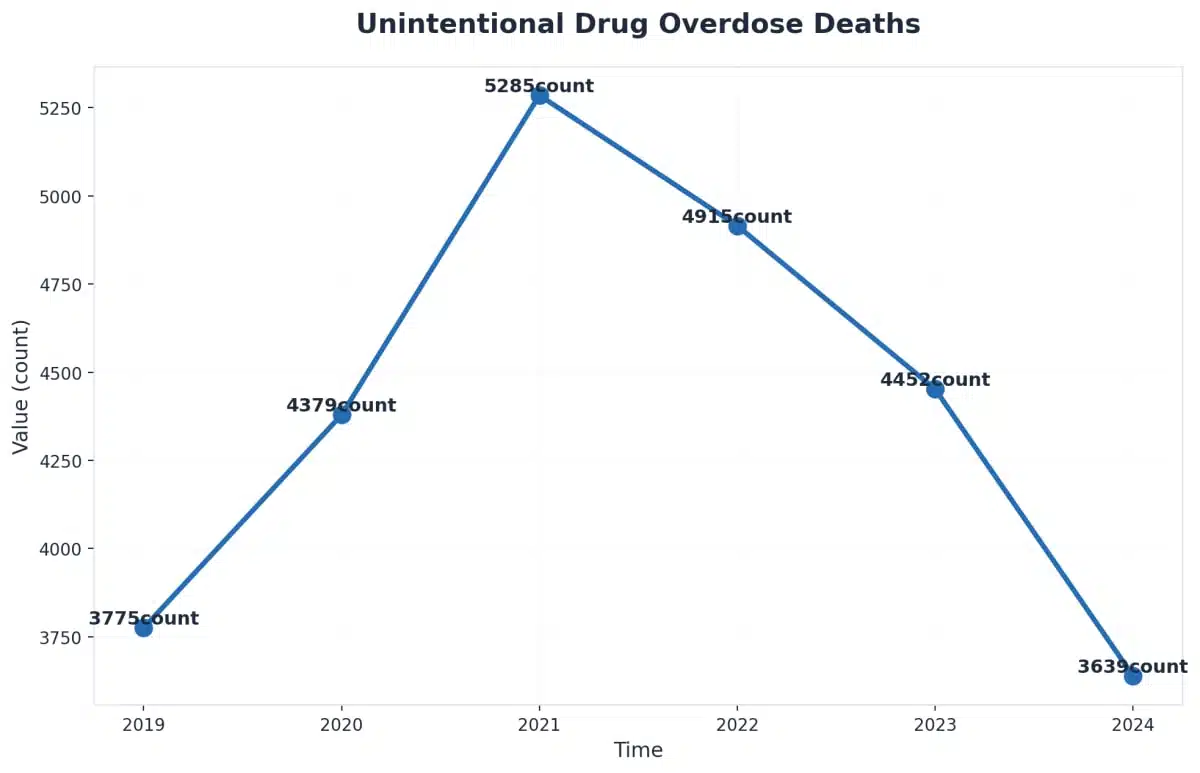
- State Statistic: Recent statewide data shows a 23% drop in unintentional drug overdose deaths, highlighting the effectiveness of expanded treatment access and integrated care.
- State Resource: The Ohio Department of Mental Health and Addiction Services (OhioMHAS) provides essential oversight, resources, and support for recovery programs statewide.
Understanding Medical Detox in Ohio
What Medical Detox Actually Means
When you or a loved one are ready to take the first step toward recovery, medical detox is often the most crucial foundation. In Ohio, this process involves receiving around-the-clock medical supervision while the body safely clears drugs or alcohol. It isn’t just about quitting a substance—it’s about managing withdrawal symptoms in a secure, controlled environment, significantly reducing the risk of seizures, cardiac events, or severe psychological distress.
Medical detox protocols in Ohio follow strict, evidence-based guidelines. Licensed medical teams at trusted facilities like Arista Recovery tailor care based on each person’s unique history, substance use patterns, and co-occurring health needs1. Whether you are seeking help for yourself or guiding a loved one, you know how unpredictable withdrawal can be, especially with fentanyl or polysubstance use on the rise in the Columbus area and throughout Ohio4.
That’s why the focus is on more than just physical stabilization—it’s also about beginning a comprehensive mental health assessment and coordinating the next steps for ongoing treatment. For many, this is the first time feeling safe enough to ask for help, and every moment of compassionate support truly matters. Medical detox is only step one, but it’s a foundational one that sets the stage for lasting healing.
Why Medical Supervision Is Critical
Medical supervision during detox in Ohio isn’t just a best practice—it’s a life-saving necessity shaped by the state’s unique substance use patterns and high rates of opioid-involved emergencies. With fentanyl and methamphetamine frequently detected in overdose cases, withdrawal can rapidly escalate from uncomfortable to medically dangerous. This is particularly true in the Columbus, Cleveland, and Cincinnati regions, where overdose rates have historically remained among the highest in the state4.
“Withdrawal can trigger seizures, delirium, and cardiac events—risks that increase exponentially with polysubstance use and co-occurring health conditions. Continuous monitoring is essential to prevent life-threatening complications.”
The ASAM guidelines adopted by most Ohio facilities require continuous monitoring and tailored interventions to support safe stabilization1. It’s not just about managing symptoms; it’s about catching the subtle warning signs that only trained medical staff can spot before a crisis unfolds. When withdrawal is medically supervised, the odds of transitioning to further treatment rise dramatically.
Medication-assisted withdrawal protocols boost engagement by up to 60% compared to abstinence-only detox, reducing early drop-out and giving patients a real shot at sustained recovery2. Every hour of professional support provided is another step away from relapse and another win for recovery in Ohio.
Ohio’s Medical Detox Landscape and Regulations
State Licensing and Accreditation
State licensing and accreditation form the backbone of safe, effective medical detox in Ohio. Every detox facility must be licensed by the Ohio Department of Mental Health and Addiction Services (OhioMHAS), which sets strict requirements for staffing, safety protocols, and emergency preparedness11. In addition, reputable programs like Arista Recovery seek accreditation from national bodies like the Commission on Accreditation of Rehabilitation Facilities (CARF) or The Joint Commission, ensuring adherence to evidence-based standards and continual quality improvement1.
These layers of oversight are vital—especially when serving diverse communities from Cleveland to the Appalachian counties. Licensing isn’t just a bureaucratic checkbox; it protects patient safety, mandates credentialed medical staff, and requires regular inspections. Accreditation pushes programs to stay current with evolving detox guidelines, including the latest ASAM recommendations for polysubstance withdrawal and integrated care1.
Recent updates in Ohio have expanded requirements for medication management and mental health assessment during detox, reflecting the state’s commitment to holistic care and better outcomes11. When every step of the process is held to these high standards, it ensures that even the most at-risk individuals can begin recovery with dignity and safety.
Ohio’s Response to the Opioid Crisis
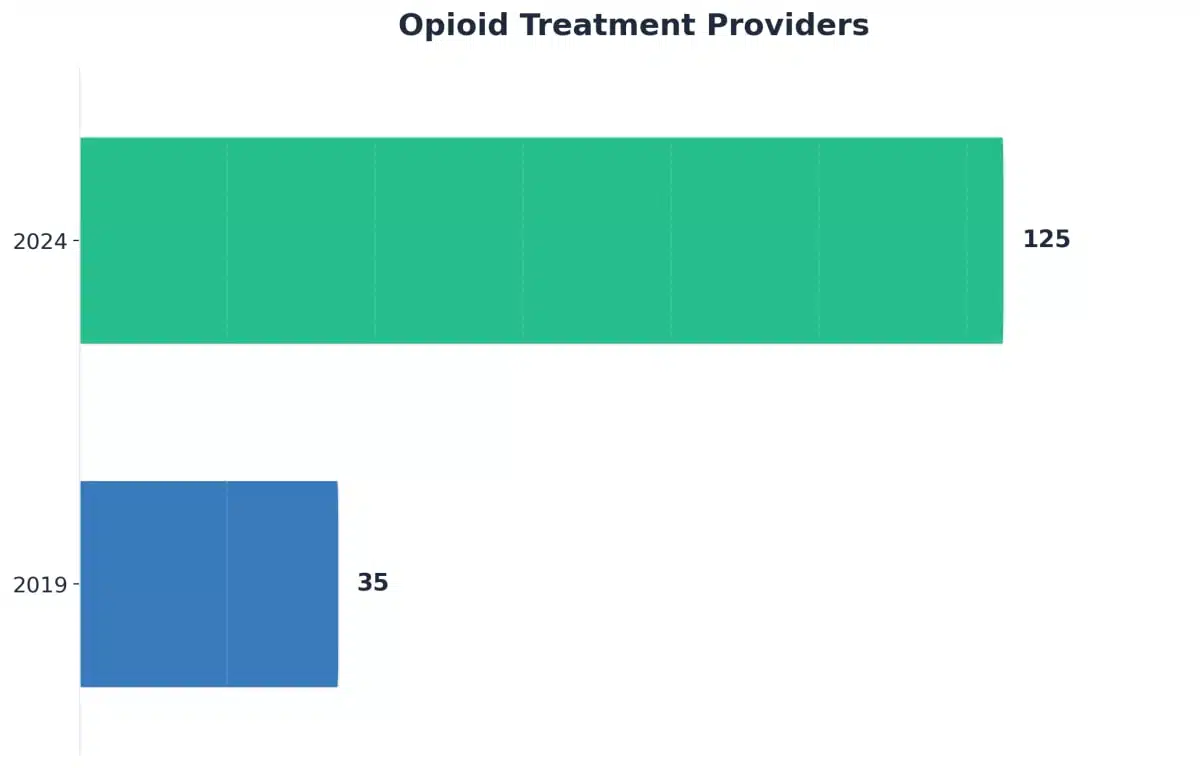
Ohio’s opioid crisis has demanded a statewide response that goes far beyond awareness campaigns—it has fundamentally reshaped how medical detox is delivered in every corner of the state. Since 2020, the number of opioid treatment providers in Ohio has soared by over 250%, reflecting an urgent investment in infrastructure and workforce to meet the growing need4.
Despite heartbreaking overdose rates in cities like Dayton and Akron, the most recent statewide data show a dramatic 23% drop in unintentional drug overdose deaths from 2023 to 2024. This suggests that expanded treatment access and integrated medical detox are making a real, measurable impact4. Every reduction in overdose deaths means more people are getting the chance to enter detox and take those first steps toward recovery.
In response to fentanyl’s rise and the complexities of polysubstance use, Ohio has prioritized rapid access to medical detox, the adoption of fentanyl-specific protocols, and stronger bridges to mental health care. The state’s approach isn’t just about stopping overdoses—it’s about building a recovery ecosystem where people in every region can find hope and effective care.
Evidence-Based Protocols and Treatment
Medication-Assisted Treatment Options
Medication-assisted treatment (MAT) has become a cornerstone of evidence-based medical detox across Ohio, especially as fentanyl and other potent opioids remain primary drivers of admissions in regions like Dayton, Cleveland, and the Columbus metro. MAT protocols typically involve carefully selected medications based on the patient’s substance use history, medical profile, and risk factors.
| Medication Type | Primary Application | Clinical Benefit During Detox |
|---|---|---|
| Buprenorphine (Suboxone) | Opioid Withdrawal | Reduces cravings and eases severe withdrawal symptoms safely. |
| Naltrexone (Vivitrol) | Alcohol & Opioid Use | Blocks the euphoric effects of substances to prevent relapse. |
| Methadone | Severe Opioid Dependence | Provides long-acting stabilization for highly dependent individuals. |
In Ohio, recent regulatory updates have expanded access to MAT, helping to address longstanding gaps in rural and urban communities alike4. It can be challenging to stabilize patients who arrive in acute withdrawal, often with anxiety about “trading one drug for another.” But the evidence is clear: MAT during medical detox increases engagement in ongoing care by up to 60% compared to abstinence-only approaches2.
These protocols don’t just ease withdrawal—they help reduce cravings, lower relapse risk, and support smoother transitions into residential or outpatient treatment. In practice, MAT is most effective when combined with counseling and mental health support, reflecting Ohio’s statewide push for integrated, whole-person care1.
Managing Co-Occurring Mental Health
Managing co-occurring mental health conditions alongside substance withdrawal is a daily reality for Ohio detox professionals. In fact, up to 80% of people entering opioid detox in Ohio present with anxiety, depression, PTSD, or other psychiatric diagnoses. This makes dual diagnosis treatment not just ideal, but essential for safe stabilization and long-term recovery8. You see this complexity in every region—from the urban stressors in Cleveland to the unique trauma histories in Appalachian counties.
Evidence shows that when mental health and addiction treatment are delivered together during medical detox, readmission rates can fall by as much as 40%, and patients are more likely to engage in ongoing care after discharge9. Ohio’s updated ASAM-aligned protocols encourage early screening and intervention, even when withdrawal symptoms are still active, because missing a psychiatric crisis or suicide risk can be catastrophic during acute detox1.
It can feel daunting to untangle symptoms—what’s withdrawal, and what’s an underlying mood disorder? But every time a clinical team validates a patient’s struggle, initiates a trauma-informed assessment, or coordinates with psychiatric colleagues, they build trust and safety. These are the moments that save lives and set the tone for recovery, especially as facilities like Arista Recovery continue to lead in dual diagnosis innovation.
Insurance Coverage and Costs for Medical Detox in Ohio
If you’re experiencing withdrawal symptoms right now, getting into safe medical care is the priority—and your insurance likely covers it. Withdrawal can be dangerous, and medically supervised detox isn’t just about comfort; it’s about keeping you safe through a critical medical situation.
Most major insurance plans in Ohio cover medical detox as an essential health benefit because it is essential medical care. Arista Recovery accepts major commercial insurance plans, including Aetna, Blue Cross Blue Shield, Cigna, Unicare, and United Healthcare. These plans typically include coverage for substance use disorder treatment, including emergency detox services. Mental health parity laws require insurers to cover addiction treatment the same way they cover other serious medical conditions—because withdrawal is a serious medical condition.
Here’s what matters right now: insurance verification happens quickly and shouldn’t delay you from getting help. Treatment centers can verify your benefits within hours, often while you’re already being admitted for detox. The verification process identifies what your plan covers, any copayments or deductible requirements, and whether prior authorization is needed—but acute medical needs typically bypass standard authorization delays.
Many Ohio residents find their insurance covers the full cost of detox after meeting their deductible, while others have manageable copayments. Your specific coverage depends on your individual plan details, but the key point is this: you can find out your exact benefits quickly, and financial responsibility is determined upfront.
If you’re worried about costs preventing you from accessing care, know that financial concerns won’t keep you from emergency detox services. Many facilities offer payment plans, sliding scale options, or financial assistance programs. Ohio also has state-funded programs and grants specifically designed to ensure people can access the medical care they need during a crisis.
Your safety comes first. Withdrawal symptoms require medical attention, and insurance coverage exists specifically to provide that care when you need it most. Reaching out to verify your benefits often reveals more coverage than you expected—and it happens fast enough that it won’t delay the care that’s keeping you safe.
Regional Access and Major Service Areas
Central Ohio: Columbus and Surrounding
Central Ohio, anchored by Columbus and its surrounding communities like Hilliard and Westerville, stands out as a major hub for medical detox access in the state. Columbus has seen a significant expansion in licensed detox facilities and integrated care programs over the past five years. This growth is driven by local leadership and targeted state investment to address the region’s high rates of opioid-involved emergencies4.
The emphasis on evidence-based medical detox—paired with early mental health assessment—reflects Central Ohio’s commitment to whole-person recovery and cultural inclusivity. Facilities in the Columbus metro, such as Arista Recovery in Hilliard, frequently pilot new approaches, including trauma-informed care for complex cases and specialized programming for veterans and the LGBTQ+ community.
While access is stronger here than in some rural counties, barriers still exist for uninsured individuals or those with limited insurance coverage. Every time professionals help a patient navigate these systems or advocate for family involvement, they make the recovery journey a little safer and more welcoming for Central Ohioans.
Access Considerations Across the State
Access to medical detox in Ohio looks different depending on where you live. In the Cleveland and Cincinnati metros, you’ll see more high-capacity facilities and specialized teams, but long waitlists and insurance navigation still create hurdles for those in urgent need. In contrast, rural areas—such as the Appalachian foothills and the Northwest—often rely on smaller clinics or hospital-based detox, with travel and limited public transportation making it even tougher for some to reach care.
The state’s efforts to expand telehealth and mobile crisis response have helped bridge some of these gaps, especially for those facing transportation or childcare barriers10. Cultural attitudes and local resources also play a big part in how people access detox. In some regions, stigma remains a major obstacle, and a lack of culturally specific services can leave significant gaps.
No matter where you are in Ohio, coordinating with local ADAMHS Boards, advocating for flexible admission protocols, and connecting families with transportation support makes a real difference. Every region deserves safe, timely access to medical detox, and ongoing statewide work helps level the playing field.
Frequently Asked Questions
How long does medical detox typically take in Ohio facilities?
The typical length of medical detox in Ohio facilities ranges from three to seven days, though some cases—especially involving alcohol, benzodiazepines, or polysubstance use—may require up to ten days of monitoring and stabilization 1. Your clinical approach will depend on the specific substances, the patient’s medical history, and the severity of withdrawal symptoms. Ohio facilities follow ASAM guidelines, which emphasize ongoing assessment to determine when a patient is medically cleared for the next level of care 1. Remember, the timeline is flexible—progress counts, even if it takes a little longer. Every safe transition is a victory for your patient’s recovery.
Can I detox from multiple substances at the same time?
Yes, it is possible to undergo medical detox from multiple substances at the same time in Ohio facilities, but it requires careful planning and around-the-clock medical supervision. Withdrawal from more than one substance—like opioids and benzodiazepines or alcohol—can increase the risk of complications such as seizures, delirium, and cardiac instability, especially given the rise of polysubstance use in regions like Columbus and Cleveland 6. Ohio programs follow ASAM guidelines, which recommend individualized protocols rather than a one-size-fits-all approach, adjusting medications and monitoring based on each person’s unique risks 1. If you’re managing a complex detox case, every extra measure you take for safety and symptom relief is a win for your patient’s recovery journey.
What happens if I experience a medical emergency during detox?
If you experience a medical emergency during medical detox in an Ohio facility, the onsite clinical team is trained to respond immediately. This means symptoms like seizures, severe agitation, or cardiac distress will be rapidly assessed and stabilized by licensed nurses and physicians, following state-mandated emergency protocols 1. Facilities are required to have emergency medications and equipment on hand, plus clear transfer agreements with local hospitals if a higher level of care becomes necessary 11. You know every second counts in a crisis. Reassure patients that your team’s quick action, monitoring, and expertise can make all the difference—helping turn a scary moment into another step forward in recovery.
Will my family be able to visit or stay in contact during detox?
Family support is recognized as a key factor in recovery, and most Ohio medical detox facilities encourage contact with loved ones during the detox process. While in-person visitation policies vary by facility and clinical acuity—especially in the first 24-72 hours—phone calls or virtual check-ins are typically allowed once it’s medically appropriate and does not disrupt care. Some programs in the Columbus and Cleveland metros even offer structured family engagement sessions to help foster hope and understanding. You know that keeping lines of communication open can reduce anxiety for both patients and families, helping everyone feel less alone in the journey 1.
What’s the difference between detox at a hospital versus a specialized facility?
Detox at an Ohio hospital typically focuses on managing acute medical emergencies—think severe withdrawal, delirium, or unstable vital signs—often in a busy inpatient or ER setting. In contrast, specialized medical detox facilities are designed for withdrawal management, offering dedicated, quiet spaces and access to addiction-trained staff. These programs follow ASAM guidelines, provide integrated mental health care, and create a more recovery-focused environment 1. You know that while hospitals are vital for high-risk stabilization, specialized facilities often allow for more personalized care, peer support, and smoother transition to ongoing treatment. Both options save lives—matching the setting to the patient’s needs is what truly makes the difference.
Do I need to complete detox before starting residential treatment?
Yes, completing medical detox is typically required before starting residential treatment in Ohio. The main reason is safety: withdrawal symptoms from substances like alcohol, opioids, or benzodiazepines can be dangerous and require medical supervision that residential programs aren’t equipped to provide 1. Once detox is complete and the patient is medically stable, the transition into residential care can focus on therapy, mental health, and building recovery skills. This sequencing is supported by ASAM guidelines statewide and helps reduce the risk of relapse or medical emergencies during early recovery. Every time you help someone make this transition smoothly, you’re strengthening their foundation for lasting change.
What if I’ve tried detox before and relapsed—will it work this time?
Relapse after medical detox is more common than most people realize, especially in Ohio, where up to 90% of individuals who complete detox without follow-up care will experience relapse 1. But that doesn’t mean hope is lost or that detox “didn’t work.” Each attempt is another opportunity for healing and another chance to connect someone with the right supports—like residential treatment, counseling, or medication-assisted treatment, all of which improve long-term outcomes 2. Yes, it’s hard to see someone struggle, but every step back is still part of the journey forward. Progress isn’t always linear, and your encouragement can help patients and families keep reaching for recovery.
Taking the Next Step Toward Recovery
Now that you understand how insurance can cover your care, there’s nothing standing between you and the safety you need right now. If you’re experiencing withdrawal symptoms or worried about what might happen if you stop using, medical detox provides immediate relief and medical supervision to keep you safe.
Withdrawal symptoms can worsen quickly—especially with alcohol, benzodiazepines, or opioids—but medical detox provides immediate relief and safety. At Arista Recovery’s Hilliard facility, you can start detox today. The center is open 24/7 for admissions, and board-certified physicians and experienced nursing staff monitor you around the clock during those critical first days. You won’t go through this alone or unprotected.
Here’s what happens in your first 24 hours: You’ll receive a comprehensive medical assessment, begin medications to ease withdrawal symptoms, and have your vital signs monitored regularly. The clinical team creates your personalized detox protocol based on what you’ve been using and your medical history. You’ll have a comfortable, private space to rest while your body begins healing under continuous medical supervision.
When you call Arista Recovery in Hilliard, the admissions team will verify your insurance coverage on the spot, answer your questions about the detox process, and—if you’re ready—help you start treatment today. You can be admitted within hours, not days. Recovery starts with one phone call, and that call can happen right now. You deserve medical care, safety, and the chance to feel better. Your bed is ready when you are.
References
- American Society of Addiction Medicine (ASAM) – Clinical Standards and Guidelines. https://www.asam.org/quality-care/standards
- National Institute on Drug Abuse (NIDA) – Research Reports on Drugs and the Brain. https://www.drugabuse.gov/publications/research-reports
- SAMHSA Treatment Services Data – Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/data-research/treatment-services-data
- CDC Opioid Data Portal. https://www.cdc.gov/opioids/data/index.html
- FDA Opioid Medications Information – U.S. Food and Drug Administration. https://www.fda.gov/drugs/information-drug-class/opioid-medications
- Withdrawal Syndrome (StatPearls) – National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK482199/
- CMS Fact Sheets – Medicare and Medicaid Coverage Policies for Substance Use Services. https://www.cms.gov/newsroom/fact-sheets
- National Institute of Mental Health (NIMH) – Co-occurring Disorders Research. https://www.nih.gov/about-nih/what-we-do/nih-almanac/national-institute-mental-health-nimh
- Mental Health Integration in Primary and Addiction Care – National Alliance on Mental Illness. https://www.nami.org/Get-Involved/Advocate/Policy-Platform/Behavioral-Health-Integration
- Medicaid and Substance Use Disorders: Addressing Key Challenges to Treatment Access – MedPAC. https://www.medicaid.gov/medicaid-chip-payment-and-access-commission/reports/publications/2023/substance-use-disorders-addressing-key-challenges-to-treatment-access.html
- Ohio Department of Mental Health and Addiction Services (OhioMHAS). https://mha.ohio.gov/
- Substance Abuse and Mental Health Services Administration (SAMHSA). https://www.samhsa.gov/
- National Institute on Drug Abuse (NIDA). https://www.nida.nih.gov/
- American Society of Addiction Medicine (ASAM). https://www.asam.org/
- CDC Opioid Data Portal. https://www.cdc.gov/drugoverdose/data/index.html
- Ohio Department of Health. https://odh.ohio.gov/
- State Medical Board of Ohio. https://med.ohio.gov/
- American Medical Association (AMA). https://www.ama-assn.org/
- Journal of Addiction Medicine. https://journals.lww.com/journaladdictionmedicine/
- SAMHSA National Helpline. https://www.samhsa.gov/find-help/national-helpline

