Key Takeaways: Navigating the Disease Model of Addiction
- Assessment Score: If you recognize addiction as a chronic condition rather than a choice, you are statistically more likely to engage with long-term medical support.
- Financial Strategy: Ohio Medicaid covers 100% of services under this model—check your eligibility immediately if cost is a barrier.
- Immediate Action: If you are in crisis, the “warm handoff” protocol in Ohio ERs connects you to peer support within hours, not days.
How Ohio Shifted to the Disease Model of Addiction
The Science Behind Addiction as Brain Disease
Let’s start with a simple picture: the disease model of addiction explains that substance use disorder is not about willpower or character, but about changes in how the brain works. Scientists have shown that repeated use of drugs or alcohol can actually alter brain circuits responsible for judgment, self-control, and motivation.
“This means that addiction is a chronic condition—like diabetes or asthma—that can be managed and treated, not a personal failing.”
Recent research confirms the biological roots of addiction. For example, studies have identified specific genetic markers that increase the risk for substance use disorders, and brain scans show that addiction changes how signals are processed. Specifically, it impacts dopamine, the brain’s “reward” messenger5. That’s why people with addiction may struggle to stop using even when they desperately want to.
Here in Ohio, this science has shaped how treatment and recovery are approached. When you understand that addiction is a brain disease, it becomes clear that medical care, therapy, and community support—not shame or punishment—are what truly help. This knowledge has led to more effective treatment programs and less stigma, opening doors for thousands of Ohioans to seek help1.
Next, we’ll look at how Ohio’s policies have changed since 2019 to reflect this scientific understanding.
Ohio’s Policy Evolution Since 2019
If you want to see real change in how addiction is treated in Ohio, tracking policy updates since 2019 is key. Here’s a simple checklist to spot progress in your area:
- Has the state increased funding for addiction treatment programs?
- Are there more providers offering evidence-based care?
- Are stigma reduction campaigns visible in your community?
- Is access to care expanding for people with Medicaid?
Since 2019, Ohio has taken big steps to treat addiction as a medical issue instead of a personal shortcoming. One major move was expanding Medicaid, which now covers behavioral health services for about 770,000 Ohioans—40% of those have a primary diagnosis of mental health or substance use disorder10. This means more families can get treatment without facing impossible costs.
The RecoveryOhio initiative also supported anti-stigma programs, making it easier for people to ask for help and get high-quality support3. Ohio’s focus on the disease model of addiction has driven a 250% increase in opioid treatment providers and an 11% drop in overdose deaths since 20202. This approach is ideal for communities that want to save lives and give people a real shot at recovery. If you’re in Ohio and wondering if support is available, Arista can help you understand these resources and find the right fit for your family.
Next, let’s see why this framework is making a life-saving difference in your local community.
Why the Disease Model of Addiction Saves Lives
If you or someone you love is facing addiction in Ohio, understanding how the state’s recovery system works can mean the difference between finding help and falling through the cracks. Ohio has developed an integrated framework—a coordinated network connecting emergency departments, treatment providers, and recovery support services—that’s designed to catch people at their most vulnerable moment and guide them toward recovery.

Instead of discharging you from the emergency room with a phone number and hope, healthcare teams now connect you directly to certified peer recovery supporters who meet you bedside. These peers have walked the same path and understand exactly what you’re experiencing.
The impact becomes clear when you consider what happens without this framework. After receiving emergency medical care for an overdose, you stabilize and then face a critical gap. You might want help, but you’re discharged into the same environment that contributed to your crisis. You’re handed a list of resources you’re expected to contact while dealing with withdrawal, shame, and the chaos that often surrounds active addiction. Most people never make that first call.
With an integrated framework, that gap disappears. Peer supporters connect with you while you’re still in the hospital, creating a warm handoff to treatment facilities that have available beds. Transportation gets arranged. Insurance questions get answered. If you have family members, they receive guidance on how to support you. The entire process flows smoothly because everyone involved knows their role and works from the same playbook.
This system also protects Ohio’s most vulnerable populations. Whether you’re experiencing homelessness, dealing with co-occurring mental health conditions, or have cycled through treatment multiple times, you benefit from coordinated care that addresses your complete situation rather than just your immediate medical crisis. Recovery support doesn’t end at discharge—it continues through community-based services that help you rebuild your life.
Ohio communities using this framework report fewer repeat overdoses, higher treatment engagement rates, and stronger long-term recovery outcomes. Emergency departments see the same individuals less frequently because they’re receiving comprehensive support that addresses root causes rather than just treating symptoms. First responders spend less time on repeat calls to the same addresses. Families find hope instead of helplessness.
The framework saves lives because it meets you where you are, connects you to what you need, and supports you through every step of your recovery journey. That’s the difference between a fragmented system and one designed around the reality of addiction and the promise of recovery.
How the Disease Model of Addiction Expands Treatment Access
Medication-Assisted Treatment Growth in Ohio
Medication-Assisted Treatment (MAT) has seen a remarkable rise across Ohio, thanks to the shift toward understanding addiction as a medical condition. If you’re wondering what MAT means, it’s simply using FDA-approved medications—like buprenorphine, methadone, or naltrexone—alongside counseling and support, to help people recover from opioid and alcohol use disorders. This approach isn’t about swapping one drug for another; it’s about stabilizing brain chemistry so recovery is possible and sustainable.
Here’s a quick self-check: Has your local clinic or hospital started offering MAT? Are you hearing less about “just quitting” and more about medical options in your area? If so, that’s evidence of the disease model of addiction at work in Ohio’s treatment landscape.
Since 2019, Ohio has boosted its number of opioid treatment providers from 35 to 125—a 250% increase. This expansion means more Ohioans can get proven help close to home, reducing travel time and waitlists2. Research shows that MAT can cut the risk of fatal overdose in half, especially when paired with counseling and steady support1. This solution fits families who want real, science-backed options rather than outdated approaches based on willpower alone.
Arista is here to guide you through these choices, offering information and support so you can find the MAT program that fits your needs. Next, let’s look at how this medical approach impacts insurance coverage for Ohio families.
Insurance Coverage Under Medical Framework
Navigating insurance for addiction treatment in Ohio has changed because of the disease model of addiction. When addiction is recognized as a medical condition, more treatment options become available under health plans, including Medicaid. Here’s a quick decision guide to help you see where you stand:
- Are you enrolled in Ohio Medicaid? Medicaid expansion now funds over $1.6 billion in behavioral health services for around 770,000 Ohioans, with 40% of these enrollees having a primary diagnosis of mental health or substance use disorder10.
- Does your private insurer cover outpatient counseling, medication, or residential treatment? Ohio law requires parity, which means addiction care must be covered like any other chronic illness.
Are you worried about losing coverage?
Some changes in federal funding could affect what Medicaid pays for in the future, so it’s smart to stay informed. Arista can help you review your coverage, understand benefits, and connect with services that fit your needs.
This approach works best when families and individuals understand their insurance options and ask for help early. The disease model of addiction makes it clear to insurers that treatment is necessary—not optional.
Next, you’ll see how Ohio measures recovery progress and why these numbers matter for your family’s future.
Measuring Ohio’s Recovery Success by the Numbers
You’ve seen how Ohio’s framework coordinates different types of support to address recovery holistically. But does this integrated approach actually work? Let’s examine the data to see what measurable outcomes this system produces across the state.
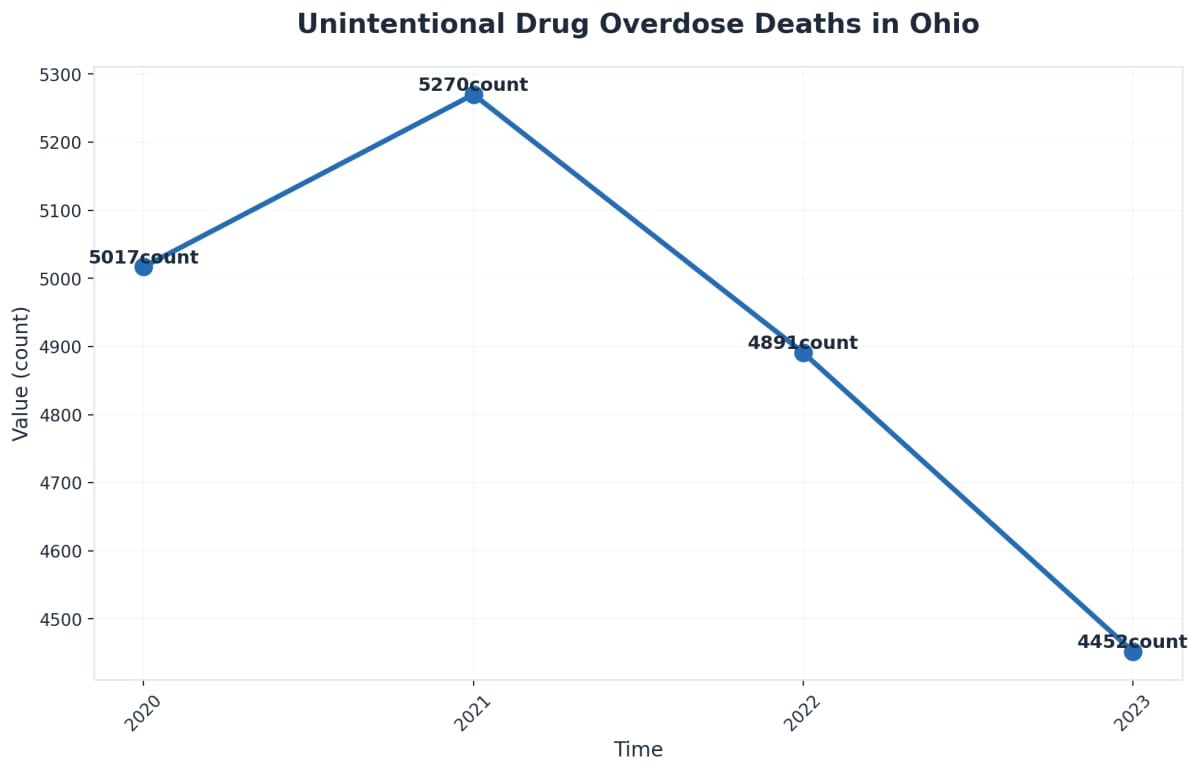
Understanding whether Ohio’s recovery programs are working requires looking beyond anecdotes to examine concrete evidence. The numbers tell a compelling story about what’s happening statewide and can help you understand what effective recovery looks like.
| Metric | Outcome | Significance |
|---|---|---|
| Substance Use Reduction | 65% reduction one year after treatment | Shows efficacy of the full continuum of care (residential + outpatient). |
| Treatment Retention | 70-75% retention through first 90 days | Staying in treatment >90 days significantly improves long-term outcomes. |
| Family Reunification | 60% report improved relationships within 6 months | Strong family connections serve as protective factors against relapse. |
| Housing/Vocational Impact | 3x more likely to maintain sobriety | Addresses practical challenges that often accompany early recovery. |
The state’s focus on reducing overdose deaths has also yielded measurable progress over the past five years. Community-based initiatives combining naloxone distribution, peer support programs, and increased access to medication-assisted treatment have contributed to stabilizing overdose rates in several Ohio counties. While challenges remain, these interventions demonstrate that coordinated efforts can make a tangible difference.
Perhaps most importantly, self-reported quality of life improvements paint a picture of recovery that extends beyond simply abstaining from substances. Recent surveys of individuals who have completed Ohio treatment programs show significant improvements in mental health, physical health, and overall life satisfaction. These subjective measures remind us that successful recovery means rebuilding a life worth living, not just stopping substance use.
When you’re evaluating treatment options, these statewide benchmarks can help you understand what effective recovery looks like and what outcomes research suggests are achievable during your own journey.
Frequently Asked Questions
Does understanding addiction as a disease mean my loved one isn’t responsible for their recovery?
Understanding addiction through the disease model of addiction doesn’t erase personal responsibility—it simply changes what responsibility looks like. Recovery still requires active steps from your loved one, like choosing to seek help, attending treatment, and working on change. The difference is, addiction is now seen as a chronic brain condition that makes these choices much harder—not impossible, but more challenging—because it affects judgment and self-control 1. This model encourages families to offer support without blame, while still holding loved ones accountable for their recovery actions. At Arista, we believe in both compassion and empowerment: you can encourage accountability while understanding the real barriers your loved one faces.
How does Ohio’s Medicaid expansion actually help families afford addiction treatment?
Ohio’s Medicaid expansion has made a real difference for families needing addiction treatment. Now, Medicaid covers services like outpatient counseling, psychiatric care, and residential drug treatment—support that many working families couldn’t afford before. In 2024 alone, more than $1.6 billion in federal funds helped pay for behavioral health care for about 770,000 Ohioans, and 40% of those covered have a primary diagnosis of mental health or substance use disorder 10. Because the disease model of addiction treats addiction as a medical condition, Medicaid is required to fund these services, giving families a pathway to affordable, ongoing recovery. Arista can help you understand what’s covered and connect you to the right resources.
If addiction is a brain disease, why do some people recover without professional treatment?
Some people do recover from addiction without formal treatment, even though the disease model of addiction shows that substance use changes the brain in powerful ways. These “natural recoveries” often happen when someone finds strong support, faces life-changing events, or builds new routines that help them avoid triggers. Recovery paths can look different for everyone; while professional help is recommended—especially for severe cases—research shows that about 1 in 4 people with substance use disorders eventually achieve recovery, sometimes outside of clinical care 1. This approach works best when you remember there’s no one-size-fits-all solution. Arista can help you find the path that fits your needs, whether that’s professional treatment or another recovery route.
What should I look for when choosing between Ohio treatment programs that use the disease model?
When comparing Ohio treatment programs that follow the disease model of addiction, start by checking if the staff includes licensed medical professionals and counselors trained in evidence-based care. Look for programs that offer medication-assisted treatment, therapy, and ongoing recovery support, not just detox. Ask if family involvement is encouraged, since support at home often helps recovery last longer. You’ll want clear, individualized care plans—avoid places with a one-size-fits-all approach. Confirm the program accepts your insurance or Medicaid, as most do under this medical model in Ohio 10. Arista can help you review your options, so you find a program that puts your recovery first.
Will my insurance cover long-term care if addiction is considered a chronic disease?
If addiction is recognized as a chronic disease under the disease model of addiction, both Ohio Medicaid and most private insurers are required to cover many forms of long-term care. This can include ongoing counseling, medication-assisted treatment, and sometimes residential programs—just like coverage for other chronic illnesses. Medicaid expansion in Ohio has helped over 770,000 people get behavioral health services, with 40% of those enrollees having a primary diagnosis of mental health or substance use disorder 10. Coverage details still vary by plan, so it’s smart to check with your insurer. Arista can walk you through your options so you don’t have to figure it out alone.
How has viewing addiction as a disease changed employer attitudes and workplace support in Ohio?
Viewing addiction as a disease has encouraged many Ohio employers to shift from punishment to support in the workplace. Now, more companies offer employee assistance programs, confidential counseling, and time off for treatment, treating addiction like any other medical condition. This change has helped reduce stigma at work and made it safer for employees to ask for help—key factors in keeping people employed and promoting recovery 7. The disease model of addiction is ideal for workplaces aiming to retain skilled workers and foster a healthier environment. If you or a loved one needs guidance on talking to your employer or accessing support, Arista can help you take the next step.
Conclusion
Recovery from addiction is a deeply personal journey, but you don’t have to walk it alone. Throughout Ohio, the evidence-based framework you’ve read about—connecting emergency departments to peer support specialists, creating warm handoffs to treatment, and coordinating care across providers—is producing the measurable results communities desperately need. The statistics show real progress: reduced overdose deaths in communities with expanded treatment access, improved employment rates among those who complete comprehensive programs, and thousands of individuals successfully connected to ongoing care through that critical safety net of peer support.
If you or someone you love is struggling with substance use, know that effective help is available right here in Ohio. The same peer support services, medication-assisted treatment, and coordinated care networks discussed in this article are operating in communities across the state. To find peer support services in your county or connect with Ohio’s network of treatment providers, contact the Ohio CareLine at 1-800-720-9616, available 24/7 for confidential support and referrals.
Taking that first step toward recovery is an act of courage worth celebrating. The warm handoff approach means you won’t navigate this alone—peer support specialists who’ve walked this path themselves are ready to meet you where you are, connect you with appropriate treatment, and provide ongoing support as you rebuild your life. Recovery is possible, and thousands of Ohioans are living proof. When you’re ready to begin, call the CareLine or visit your local emergency department, where compassionate professionals are standing by to guide you into this proven safety net of care.
References
- NIDA IC Fact Sheet 2025 | National Institute on Drug Abuse. https://nida.nih.gov/about-nida/legislative-activities/budget-information/fiscal-year-2025-budget-information-congressional-justification-national-institute-drug-abuse/ic-fact-sheet-2025
- Drug Overdose – Ohio Department of Health. https://odh.ohio.gov/know-our-programs/violence-injury-prevention-program/drug-overdose/
- New Case Study on APF’s Responding to Addiction Program Shows…. https://www.addictionpolicy.org/post/press-release-new-report-details-reductions-in-addiction-stigma-in-ohio
- Reflecting on NIDA’s 50th year and looking to 2025. https://nida.nih.gov/about-nida/noras-blog/2025/01/reflecting-nidas-50th-year-looking-to-2025
- New NIH study reveals shared genetic markers underlying substance use disorders. https://nida.nih.gov/news-events/news-releases/2023/03/new-nih-study-reveals-shared-genetic-markers-underlying-substance-use-disorders
- SAMHSA Releases Annual National Survey on Drug Use and Health. https://www.samhsa.gov/newsroom/press-announcements/20250728/samhsa-releases-annual-national-survey-on-drug-use-and-health
- Stigma and Discrimination | National Institute on Drug Abuse. https://nida.nih.gov/research-topics/stigma-discrimination
- Addiction as a brain disease revised: why it still matters, and why the criticisms are off target. https://pmc.ncbi.nlm.nih.gov/articles/PMC8357831/
- Understanding the Opioid Overdose Epidemic – CDC. https://www.cdc.gov/overdose-prevention/about/understanding-the-opioid-overdose-epidemic.html
- HPIO analysis: Medicaid expansion cuts could limit Ohioans’ access to mental health, addiction treatment. https://www.healthpolicyohio.org/about-us/press-releases-amp-news/2025/05/05/hpio-analysis-medicaid-expansion-cuts-could-limit-ohioans-access-to-mental-health-addiction-treat


